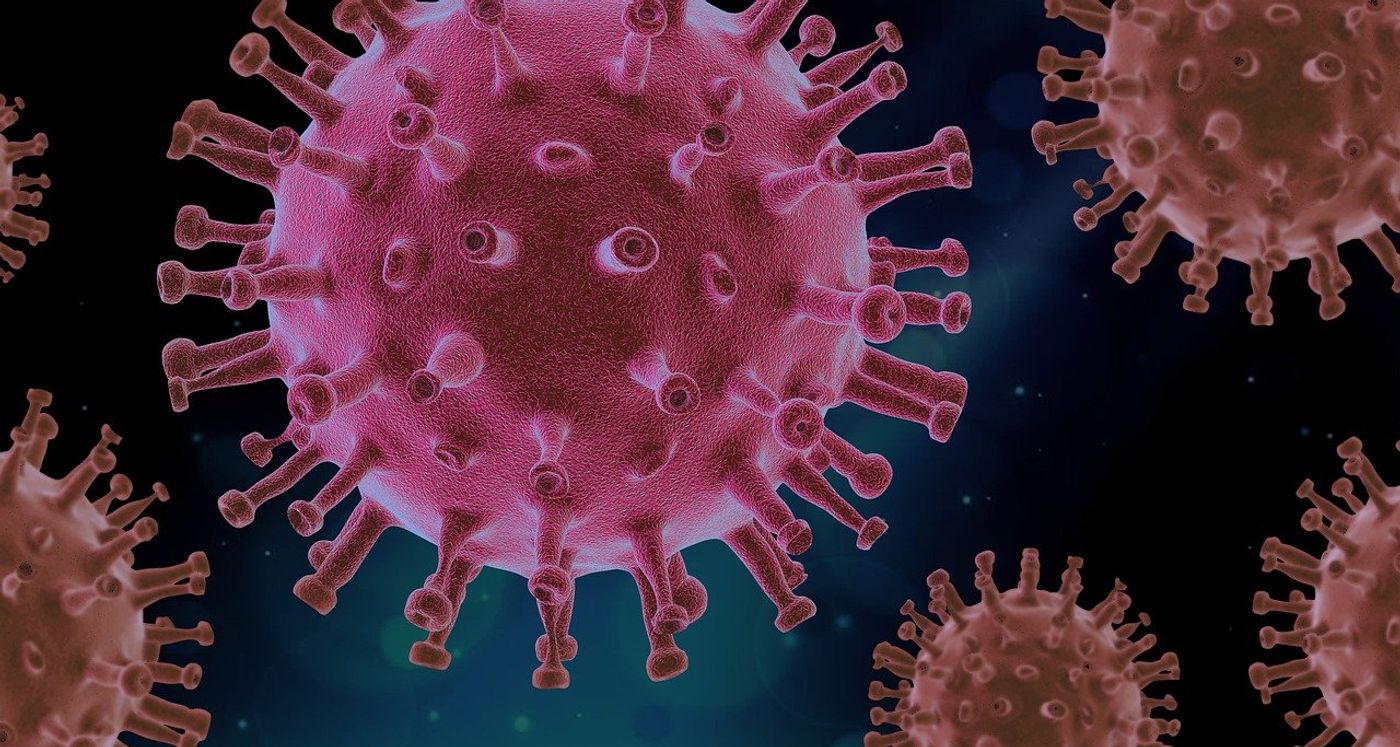
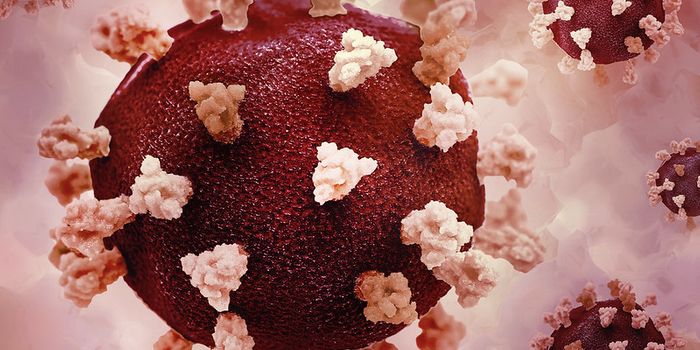
COVID-19 has directly impacted lives around the globe, and as researchers learn more about the respiratory disease, they’re also learning more about the scope of disruptions to survivors’ long term health. News stories about “long haul,” or “long COVID” have emerged, full of anecdotes that chronical severe fatigue, shortness of breath, and cognitive issues like memory loss and difficulty concentrating. As scientists have begun chronicling and cataloging these symptoms, a new question has arisen: Does the disease and its lingering symptoms change the brain? More specifically, is there an underlying physiological explanation of mental health disorders in COVID-19 survivors, such as posttraumatic stress?
A new study published in the journal, Neurobiology of Stress, show abnormal brain connectivity patterns associated with increased posttraumatic stress symptoms (PTSS) in COVID-19 survivors, in contrast to the control group. New approaches to fMRI no longer assume a static state for the brain’s functional connectivity, but instead, “capture dynamic functional brain connectivity, showing the way brain patterns change over time in fundamental and reoccurring ways,” according to Georgia State University psychologist, and the study’s co-author, Vince Calhoun.
Researchers identified three distinct and reoccurring dynamic functional network connectivity (dFNC) states in the brains of the COVID-19 research participants. Increased occurrences of one dFNC state in particular, which involves the sensorimotor and visual domains, correlated with pronounced posttraumatic stress symptoms (PTSS). Calhoun, along with co-author, Zening Fu, emphasize “the importance of evaluating dynamic functional network changes with COVID-19 survivors.”
Sources:
-
MAY 07, 2024Is It Anti-RNP or Anti-Sm/RNP?
- See More
-
APR 30, 2024Immuno-Oncology Virtual Event Series 2024
-
MAY 07, 20243rd International Biosecurity Virtual Symposium
-
MAY 23, 2024For the Love of Digital PCR 2024
- See More