Learning More About Racial Disparities in COVID-19
Racial minorities are disproportionately impacted by health problems and mortality, which is due in part to systemic racism in the healthcare system. During the pandemic caused by SARS-CoV-2, Blacks have also experienced higher rates of infection and death due to the virus; in some cases, at rates more than two or three times as high as other segments of the population in the same geographical area. Researchers set out to learn more about why this is happening. Their findings have been reported in the Journal of the American Medical Association (JAMA).
"Our study suggests one factor that may partially contribute to COVID-19 risk among Blacks," said the lead study author Supinda Bunyavanich, M.D., M.P.H., Professor of Genetics & Genomic Sciences and Pediatrics, Icahn School of Medicine at Mount Sinai Hospital.
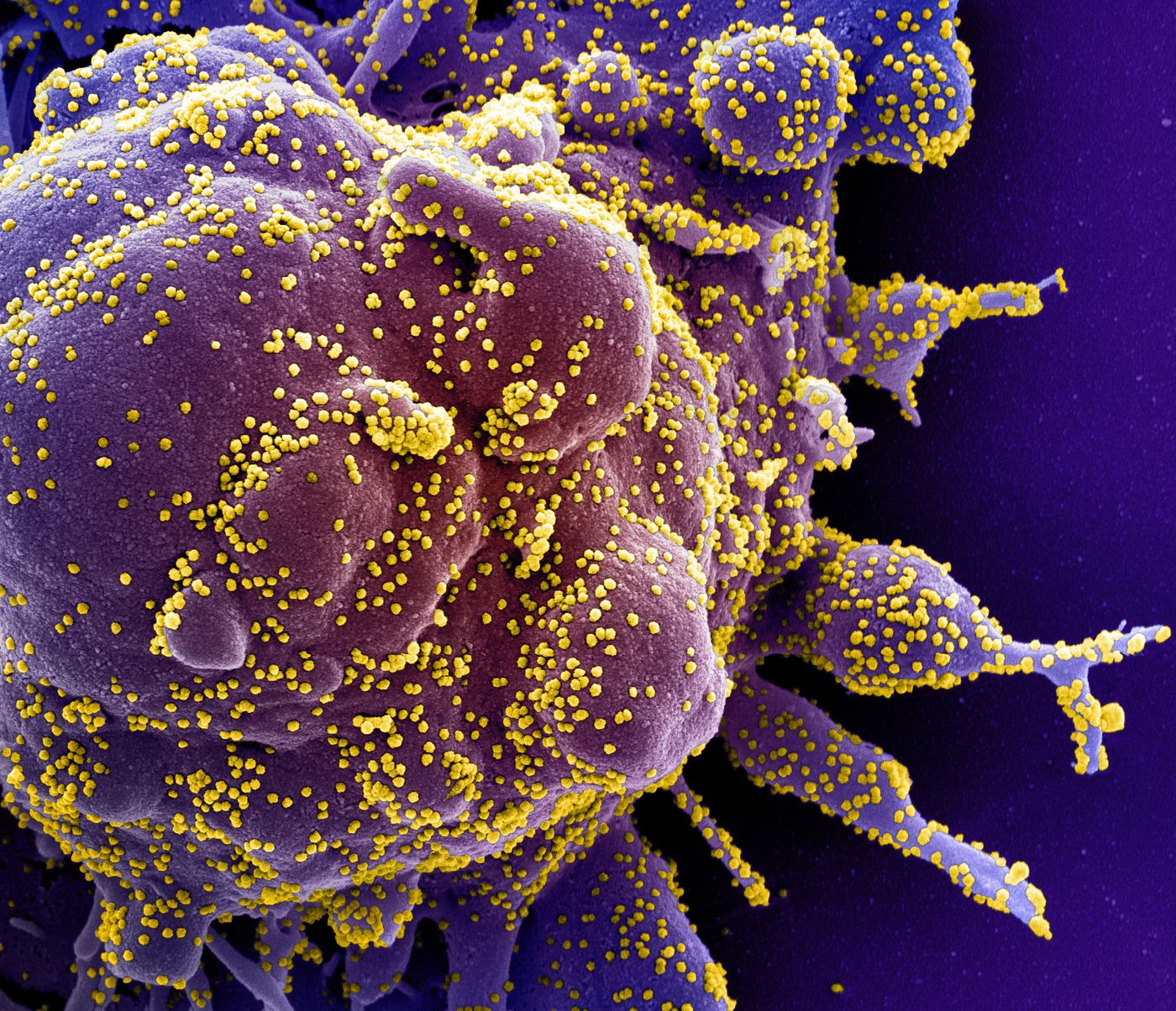
During a viral infection, viral proteins attach to proteins on the surface of host cells. This can enable the virus to gain entry, and the cell becomes the new host for the virus. SARS-CoV-2 can bind to several receptors including ones called ACE2 and TMPRSS2 on human cells, especially human nose cells.
"The virus that causes COVID-19, SARS-CoV-2, uses transmembrane serine protease 2 (TMPRSS2) to facilitate entry and spread in the body," explained Dr. Bunyavanich. "The degree to which a person expresses TMPRSS2 may affect how easy it is for the virus to get in and spread. We found that nasal expression of TMPRSS2 was significantly higher in Blacks than in Asians, Latinos, those of mixed race/ethnicity, and Whites. An important point is that gene expression is a dynamic reflection of personal, social, and environmental history, and many complex factors contribute to health disparities."
While people carry more or less the same genes in their genomes, small variations in the sequences of those genes can cause biological changes; in some cases, very small variants lead to huge changes. Variants carried by Blacks may be leading to the increased expression of the TMPRSS2 receptors.
In this study, the researchers collected nasal swabs from 305 patients aged 4 to 60, with diverse racial/ethnic backgrounds. It was only conducted within one area, however.
"One of the key takeaways of our findings is the critical importance of including diverse participants in clinical trials," noted Dr. Bunyavanich. "In clinical trials of TMPRSS2 inhibitors, it's possible that different effects may be seen depending on racial/ethnic background. More broadly, we also need to address the social determinants of health, economic disparities, and differential access to health care that drive racial/ethnic disparities in health."
Previous work by Bunyavanich and colleagues has suggested that differences in ACE2 receptors may explain, in part, why COVID-19 doesn't affect that many children.
"In that study, we found age-dependent expression of the SARS-CoV-2 receptor angiotensin-converting enzyme 2 (ACE2) in nasal epithelium, with levels lowest in young children and increasing with age into adulthood. Lower ACE2 expression may help explain why children have been largely spared in the pandemic, while possibly pointing to a potential biomarker of susceptibility to SARS-CoV-2," said Dr. Bunyavanich.
Sources: AAAS/Eurekalert! via The Mount Sinai Hospital / Mount Sinai School of Medicine, JAMA