A Genetic Risk Factor is Shared by Alzheimer's and Severe COVID-19
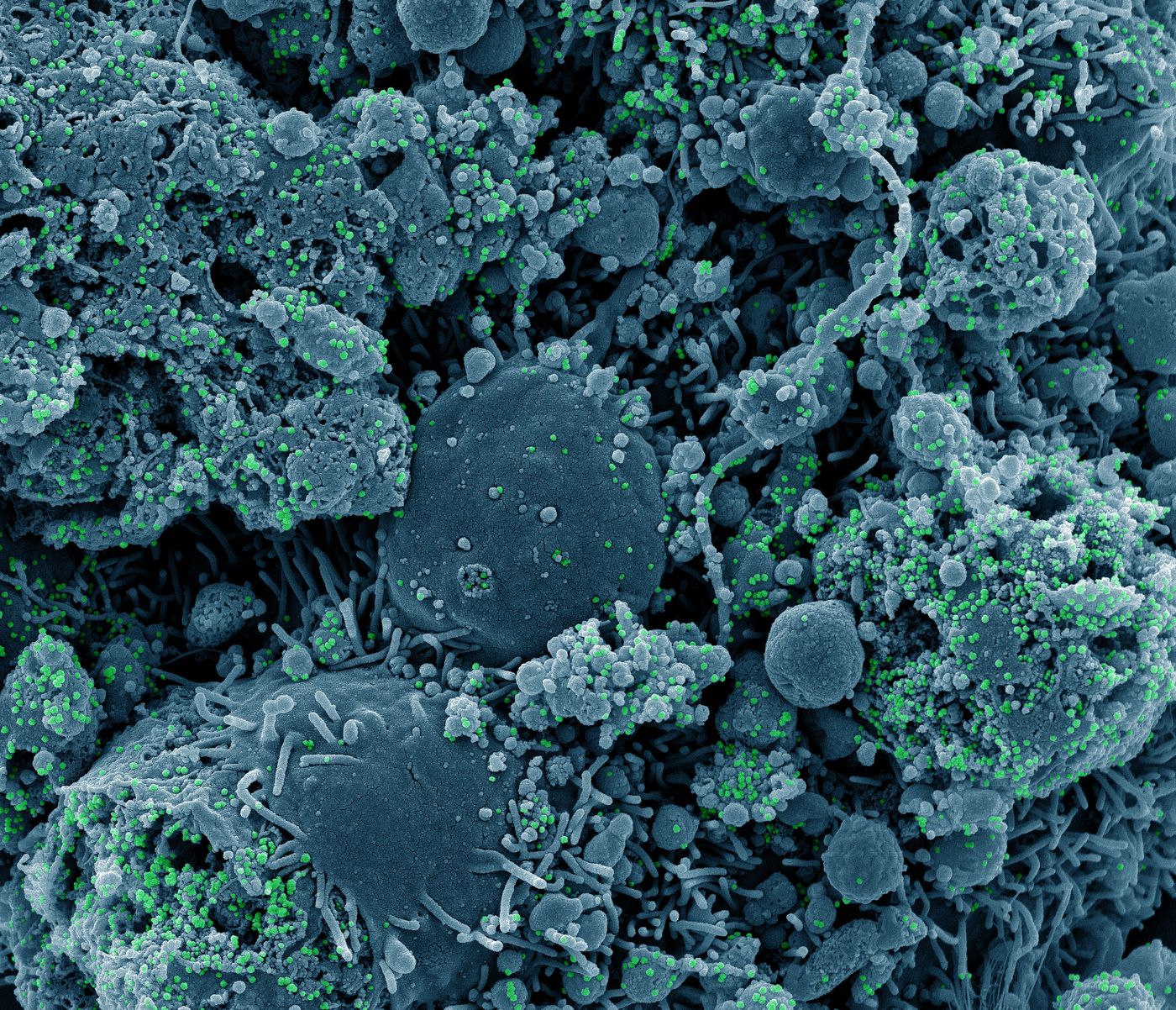
While amyloid plaques are a hallmark of Alzheimer's disease, the neurological disorder has also been linked to inflammation and viral infections. Now, researchers have identified a genetic risk factor that is common to both Alzheimer’s disease and severe COVID-19. Small changes in the sequence of a gene called OAS1 can increase a person's risk of developing Alzheimer's, while related variations in the same gene can raise the chances of a serious case of COVID-19. The work, which has been reported in Brain, could help scientists develop new treatments for both disorders, and potentially, other causes of dementia.
The researchers noted that during a COVID-19 infection, inflammation may occur in the brain. This study has found a gene that could be increasing brain inflammation by exaggerating the immune system's response to COVID-19, said lead study author Dr. Dervis Salih of the UCL Queen Square Institute of Neurology and UK Dementia Research Institute at UCL. “We have found that some of the same immune system changes can occur in both Alzheimer’s disease and COVID-19."
The OAS1 gene is active in a type of brain cell called microglia. These cells are known to be involved in immunity in the brain, and are thought to make up about 10 percent of all the brain's cells.
In this study, the researchers assessed genetic sequence data from 2,547 people; half of these individuals had Alzheimer’s disease. One specific gene variant in OAS1 that's known as rs1131454 increased a person's likelihood of developing Alzheimer’s disease anywhere from 11 to 22 percent compared to people that did not carry the variant. This variant is common in Europeans; about half of them are thought to carry it, and its impact on Alzheimer's is more significant than several other known risk genes.
The four variants that the study focused on all decrease the OAS1 gene's activity. The study also determined that the variants that increase Alzheimer's risk are usually inherited together. The OAS1 variants can raise a person's chances of a severe COVID-19 case if they are infected with SARS-CoV-2 by as much as 20 percent.
Additional work suggested that when OAS1 is less active in microglia than normal, there is a heightened response to tissue damage, and the immune system turns on the body and attacks its own tissue. In this case, that autoimmune dysfunction would be occuring in the brain, with serious consequences.
The expression of OAS1 changes over a person's lifetime, so this work could also help explain why older people are more vulnerable to COVID-19 and other disorders including Alzheimer’s.
“If we could develop a simple way of testing for these genetic variants when someone tests positive for COVID-19, then it might be possible to identify who is at greater risk of needing critical care, but there is plenty more work to be done to get us there. Similarly, we hope that our research could feed into the development of a blood test to identify whether someone is at risk of developing Alzheimer’s before they show memory problems," Salih noted.
Sources: University College London (UCL), Brain