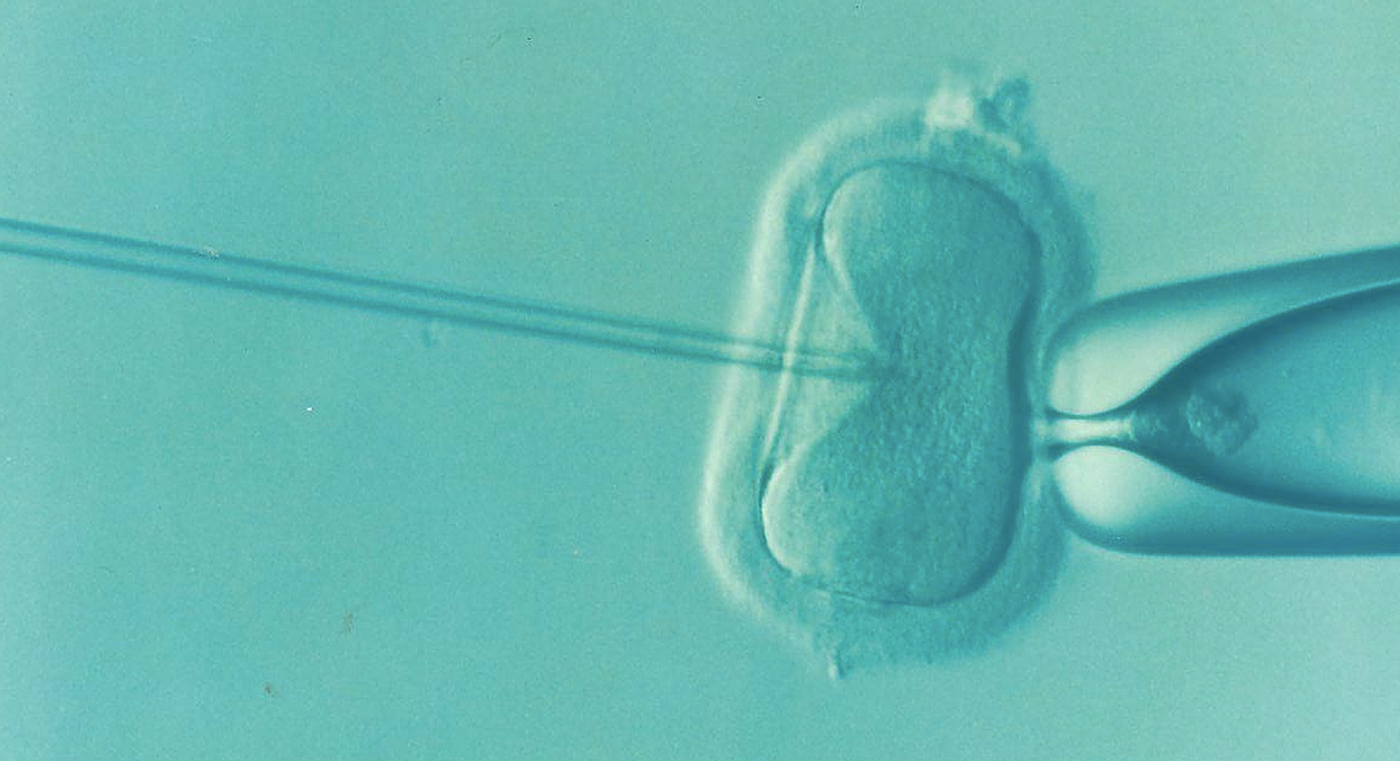
Is the Preimplantation Genetic Diagnosis of Embryos Being Oversold?
A wide array of technologies have converged to make genetic testing of embryos possible. But this practice is now expanding beyond early tests that were used to inform parents of well-established links between genetic or chromosomal errors and disorders like Down syndrome or Huntington's disease. About 600 tests have been approved for those types of conditions. People can now also opt for tests that assess conditions that are far more complex, and have unclear etiologies. But those complex disorders, such as type 2 diabetes, have convoluted genetic associations that may vary from one population to another, or even one individual to another, and which may be affected by all their other genes. Genetic testing in IVF has been regulated in some countries, while in others it is not. Now, scientists are warning about the application of such genetic testing, and have called for debate and regulation on their use.
Complex disorders can be influenced by very small changes in hundreds of different genes. For some disorders, what's called a polygenic risk score can be calculated, which can estimate how likely it is that a person might develop a particular disease. Though these scores have been used reliably in some instances, for the most part, researchers still have a lot to learn about all the many changes that can occur in one person's genome, and how they all add up to raise or lower the risk of a complex disease.
People who use IVF might now be told that they can select certain embryos that may have a lower risk of certain complex diseases, but there is not much hard evidence to back those claims up. Scientists are still teasing apart all the connections between various genes are diseases, and how tiny alterations in those genes affect a person's disease risk. Aside from the reliability of the tests themselves, there are serious ethical considerations. In new papers in Nature Medicine, scientists have called attention to this issue.
When it comes to testing the genes of embryos, there are also major technical challenges. Only a small amount of genetic material is typically obtained when performing a biopsy on an embryo. In one study, the researchers generated sequences for over 100 embryos, and combined it with data from their parents to fill in the gaps. These results were compared to data from siblings that had been born. This illustrated that polygenic risk scores could be calculated with 97 to 99 percent accuracy for twelve conditions, by implementing the protocl they developed.
So this type of screening does seem to be feasible for certain conditions. But it's not that simple for most disorders. Many polygenic risk scores are based on studies that used data from people of European descent, and these datasets lack diversity. Therefore, the scores may only apply to those people, or even only to specific groups within that population. Small genetic changes may also have wide-ranging impacts on various conditions, many of which we haven't revealed yet. So it's difficult to say with certainty whether it's beneficial to reduce the frequency of certain variants in people. A variant that raises the risk of one disorder slightly, for example, may dramatically lower the risk of another.
There is also the influence of the environment to consider. It's still very hard to predict which people will develop type 2 diabetes or heart disease at birth, for example, when one doesn't yet know what kind of diet they might consume, what pollutants they may be exposed to, or whether they will consume alcohol or tobacco, for example. None of us can say with certainty what kinds of medical treatments might eventually be available either.
Since risk assessments for embryos are already being marketed to people considering IVF, researchers have stressed the need for ensuring that individuals are properly informed of the uncertainties in the technique. If these scores lead some women to harvest additional oocytes or destroy embryos, they might be harmful.
The study authors suggested that polygenic risk scores should not be offered as a part of IVF until rigorous trials have been conducted. Such clinical trials should also include clear guidelines so that volunteers understand what is and is not known, they noted.
The researchers also added that the technology is advancing, and it's only a matter of time before such tests can be used with accuracy. Now is the time for a frank discussion about how and when they should be applied.
Sources: Nature, Johnston & Matthews Nature Medicine 2022, A Kumar et al Nature Medicine 2022