Reducing the Side Effects of Leukemia Treatments
Doctors want to improve leukemia treatment for kids. Currently, a test called minimal residual disease (MRD) is used to help determine what kind of treatment a patient will get. To improve the accuracy of that method, doctors are adding genetic data to the existing test to select the best therapy for each patient; it will also lessen the side effects suffered by patients. The work is briefly summarized in the following video.
"Risk stratification is a key component of improving survival rates and reducing side-effects for children with leukemia,” explained Anthony Moorman, a Professor of Genetic Epidemiology, who co-leads the Leukemia Research Cytogenetics Group at Newcastle University. "This study indicates that using a traditional MRD threshold to assign patients to different treatment groups should be refined with the integration of detailed genetic testing, to more accurately identify children with a lower or higher risk of relapse.”
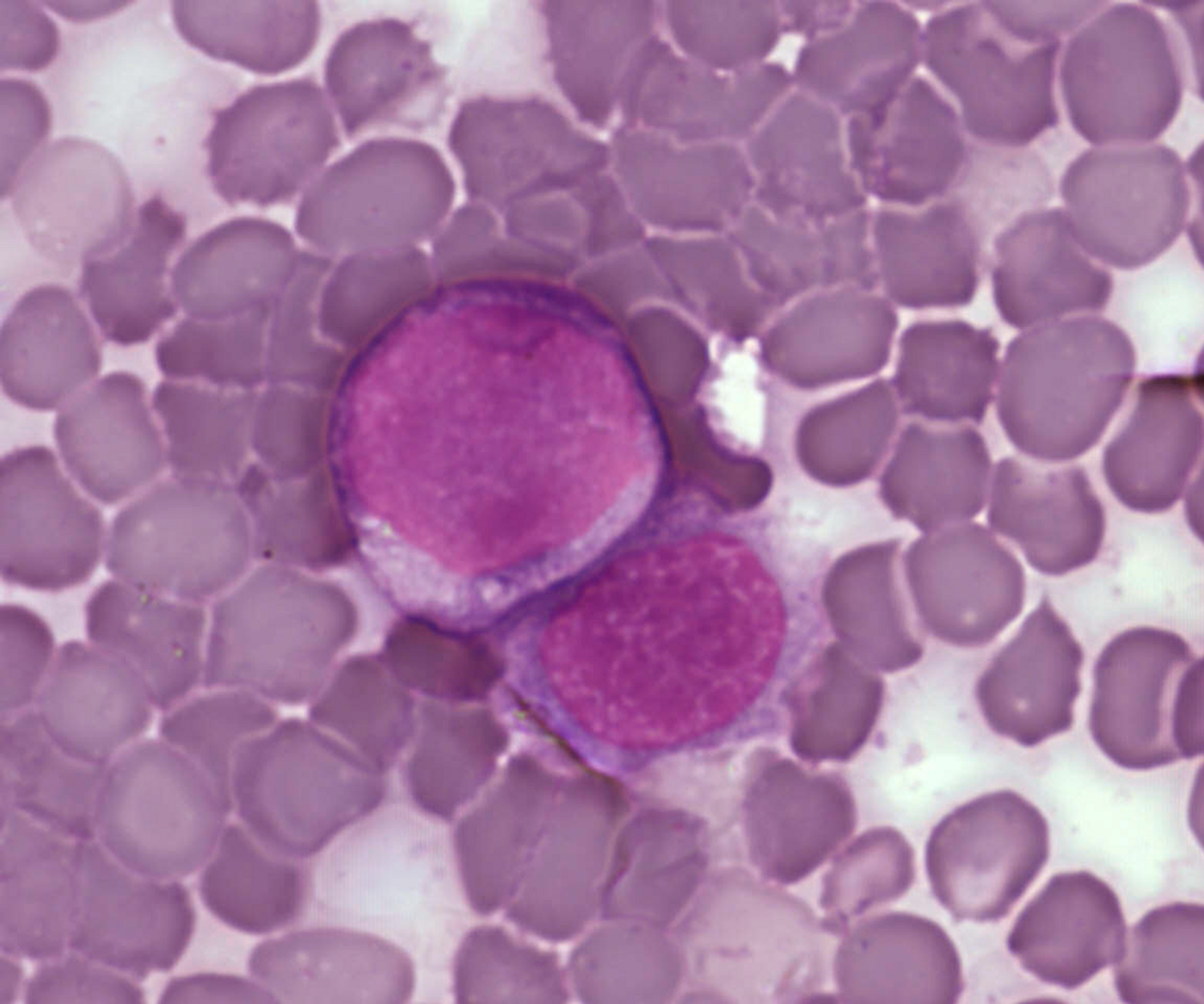
Now, at least eight of ten kids that are diagnosed with acute lymphoblastic leukemia (ALL), the most common type of childhood cancer, will survive the disease. The treatment is also extremely hard on the body. When patients have a relapse of the disease, the outlook is poor; fewer than six of ten of those children with survive more than five years.
"Current treatments for children with leukemia are highly toxic and can have devastating side-effects both in the short and the long term. New ways to reduce treatment intensity, without reducing chances of survival, are desperately needed,” commented Dr. Alasdair Rankin, Director of Research at Bloodwise. "This study represents another advance in personalizing care and should mean that more children get the right treatment for them."
For this work, patients were placed in groups depending on the genetic information carried by their leukemia cells. Genetic mutations have been associated with either a good, intermediate or high risk of relapse. Although the genetic risk of relapse carried by a patient broadly corresponded with the results of their MRD test, that did not happen for each individual. It seems that in those that with a blood content of 0.01 to 0.1 percent leukemia cells, which is just over the threshold for MRD, standard or intensive treatment would give them an excellent chance of survival.
That reduces treatment toxicity for about 50 patients every year in the UK, without affecting their chance of survival.
This work adds to recent advances in tailored treatments, a burgeoning field entering mainstream medical care. "Through this new research we have been able to take an important step forward to identify, earlier on, leukemia patients who require more targeted therapy,” said Dr. David O'Connor, Consultant Pediatrician in Hematology at Great Ormond Street Hospital. "This study suggests that early detection of patients' specific treatment needs can improve patient outcomes, and reduce the risk of relapse and complications for those patients identified. This study represents an exciting advance in personalized medicine.”
Cliff O'Gorman, chief executive of Children with Cancer UK, commented: "By developing a new method of measuring MRD, we can significantly improve the accuracy of predicting how likely it is that a child with leukemia will relapse. This has made more personalized treatment a possibility for young patients since we launched the trial in 2003 and helped to drive five-year survival for childhood acute lymphoblastic leukemia above 80%.
"But there is still much more to do. Children and young people diagnosed with cancer face aggressive treatments that can have a long-term impact on their health and well-being. It is crucial that we build on this breakthrough and continue to fund further studies and clinical trials to develop kinder, more effective treatment for young cancer patients in the UK."
Sources: Medical Xpress, Journal of Clinical Oncology