Gut Bacteria in Bees Share Resistance Genes
Antibiotic resistance has become a threat that is serious enough to get the attention of government groups like the United Nations. New work performed in honeybees has suggested that it is possible for human gut bacteria to spread this resistance. This study, by investigators at Arizona State University and Norwegian University of Life Sciences, has been reported in Molecular Ecology.
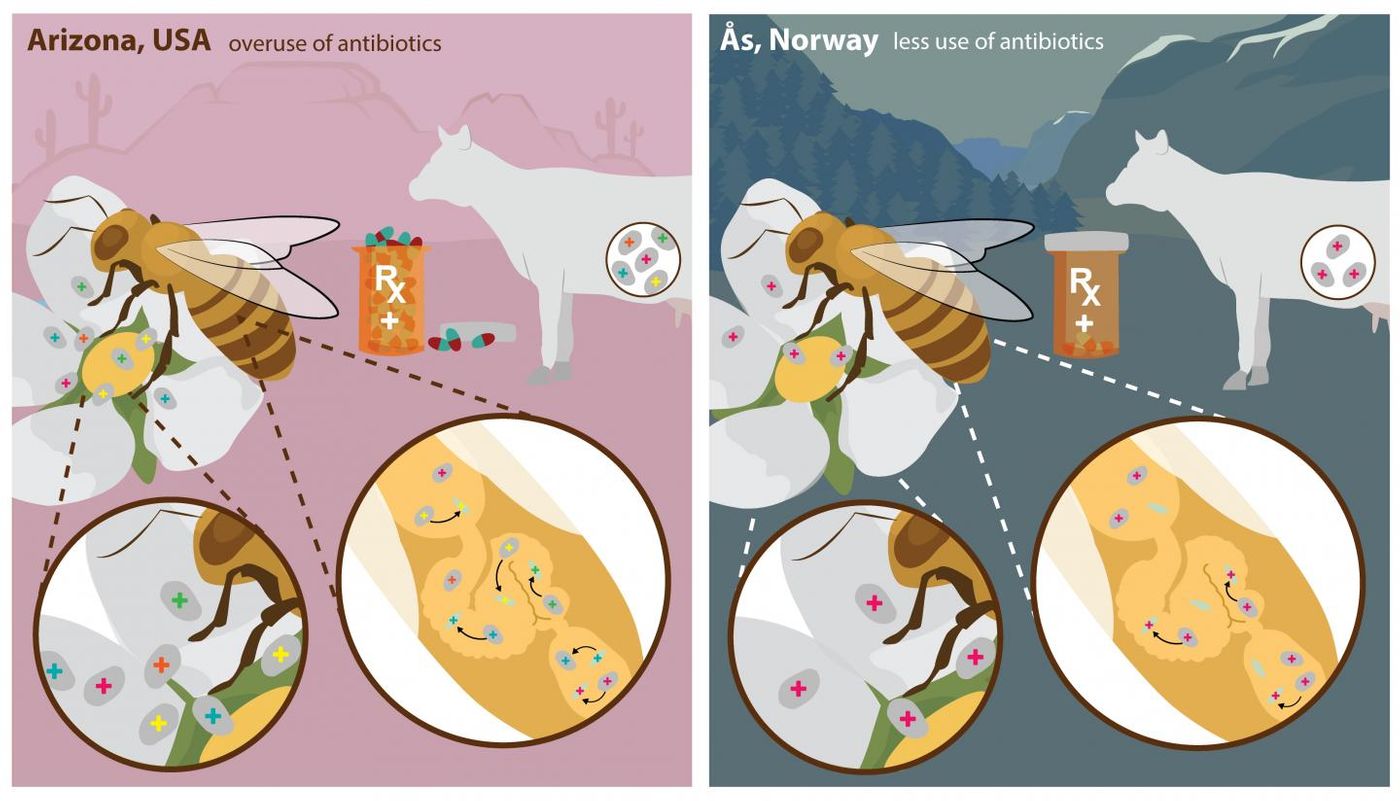
In this investigation, the scientists wanted to explore how long-term antibiotic use impacts gut bacteria. They observed microbes that live in the guts of honeybees, which have similarities to the microbial community or microbiome in our guts.
"To our surprise, we found that instead of one gut bacterium acquiring resistance and outcompeting all the other gut bacteria in honey bees, the resistance genes spread in the bacterial community so that all strains of bacteria survived," noted co-author of the work Gro Amdam, a professor with ASU School of Life Sciences.
Resistance to antibiotics was entering the honeybee microbiome.
"There is an important similarity between honey bee and human gut bacteria, in that some bacteria are in symbiosis with the host -- these are important for host health," explained lead author Jane Ludvigsen, a doctoral student at the Norwegian University of Life Sciences. "The bacteria we investigated are symbiotic for the honey bee, and they each have important functions. Because they must all be there for the host to be well, we think this is the reason that antibiotic-resistant genes have spread to all."
Because the antibiotic tetracycline has been widely used in agriculture, from apple trees to pig farming, and is commonly prescribed to people, the study focused on microbes that are resistant to the drug. When exploring antibiotic resistance genes from different geographical areas, significant differences were found.
"In the bees from Arizona, we saw that even though they have not been in contact with tetracycline for many years, the resistance genes are still there," noted Ludvigsen. "Also, in the Norwegian population, we found some antibiotic-resistant genes, but few.
"I think that if there are more resistance genes in the environment, more transfer happens. Also, if the bees are exposed to tetracycline in their environment, they may need to get and keep the resistance genes. Tetracycline is used still in the U.S., so that might be a trigger. That deserves further study, as it was not the focus of this paper."
In the Arizona honey bee, there were six different variants of the antibiotic resistance gene under investigation, while in Norway, only one variant was found.
Amdam suggested that microbes that are resistant to tetracycline are everywhere, even inside our bodies. But if antibiotic use is reduced, some of that resistance can be expected to go away over time. Antibiotics cause selective pressure in a population and promote antibiotic resistance. Amdam and Ludvigsen noted that this emphasizes the importance of eliminating antibiotic use agriculture and using it only when necessary in patients.
Although antibiotic resistance genes can be found in hospitals, they can live practically anywhere.
"Our paper predicts that if there is already antibiotic resistance in your gut, then most or all of your gut microbes will also carry this resistance. Basically, we've become potent reservoirs for carrying antibiotic-resistant genes," said Amdam. "This is not good news from an epidemiological point of view. If our paper is right, then from what we see in the U.S. and Norway, you can keep accumulating multiple versions of antibiotic-resistant genes. If pathogenic bacteria pass through your body, they can also pick up this resistance."
Some information about bees and the gut bacteria they carry can be found in this video.
Sources: AAAS/Eurekalert! Via Arizona State University, Molecular Ecology