How A High-Risk Heart Surgery Changed in 10 Years
A rip in the lining of the aorta requires immediate attention; 40 percent of people with this condition die immediately, and 19 percent die during the high-risk operation to repair the aorta. Over time, though, the surgical procedure to treat this condition, called Type A aortic dissection, has become more complex and more effective.
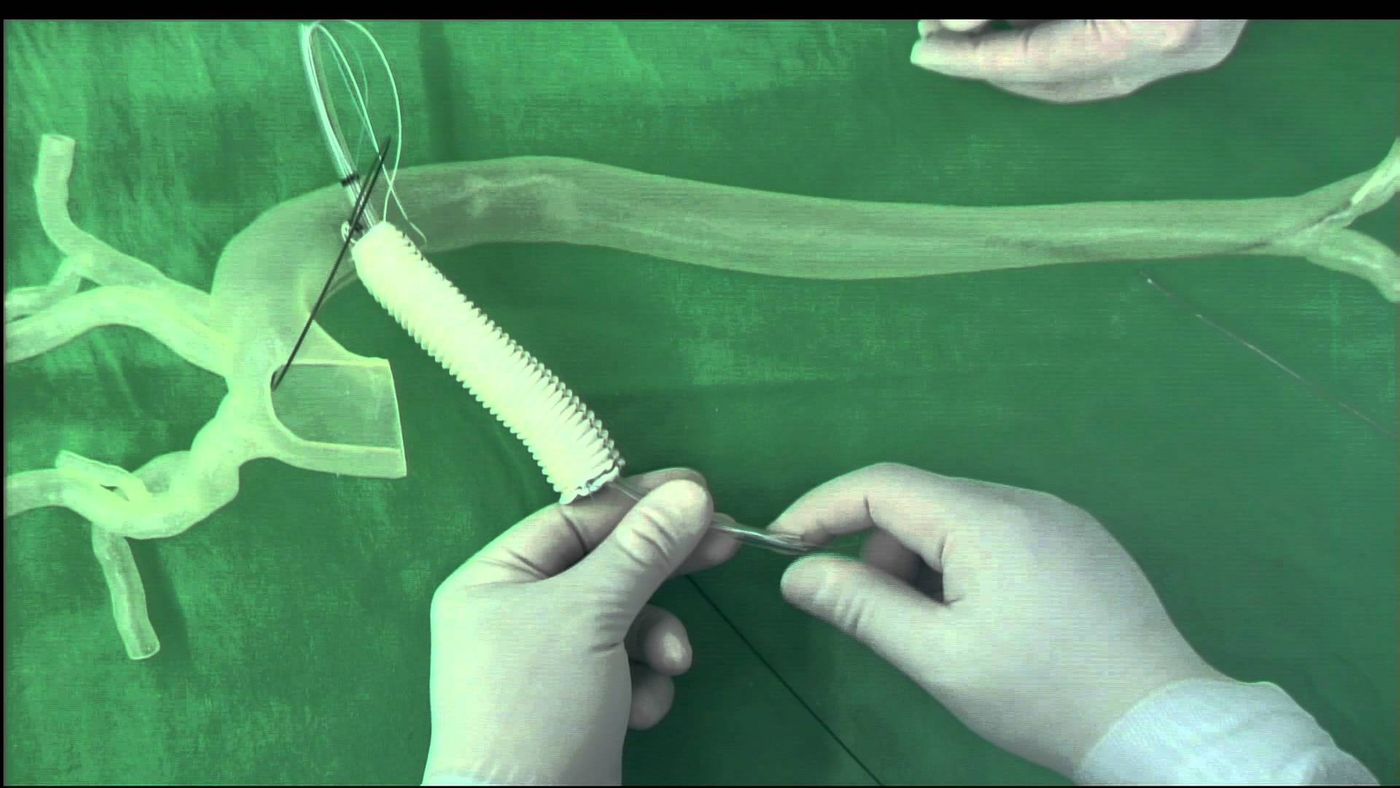
Type A aortic dissection describes a condition where the inner lining of the aorta tears due to high blood pressure or a tightening of the arteries. Blood pours out of the main channel of the artery and flows into the arterial walls. Tears begin in the ascending aorta near the heart and have been known to extend as far as to the arteries in the legs. Immediate surgery to mend the dissection is necessary to prevent stroke, heart attack, congestive heart failure, and dangerous bleeding.
New surgical techniques and improved postoperative care over the past decade have reduced the risk of complications, such as pneumonia or the need for reoperation and improved long-term outcomes, but the surgery’s mortality rate has stayed relatively the same at 19 percent.
Researchers conducted a study to assess the evolution of the surgery to repair type A aortic dissection, analyzing medical records of 884 people who had the procedure. The surgeries occurred over a period of time, from 2003 to 2015. Researchers looked to see if mortality rate, risk of complications, and the complexity of the surgeries changed over the years. Mortality rate stayed the same, risk of complications decreased, and operations became increasingly complex.
"Surgeons are increasingly comfortable with performing more extensive repairs of the aorta and utilizing new surgical techniques, and they are doing so without increasing risk," explained senior author Ravi K. Ghanta, MD. "However, while the operative mortality numbers are lower than historical outcomes, 19% is still significant and further improvement is needed."
In the future, Ghanta is interested in looking at the influence of individual patient anatomy of surgical outcomes, short-term and long-term. "We need to discover how to make these complex surgeries faster and easier; in doing so, it will be important to learn as much as possible so that surgeons can tailor the surgical repair to the patient and balance upfront surgical risks with improved long-term outcomes," explained study researcher Robert B. Hawkins, MD.
"This study shows that surgeons are adapting their surgical strategies to more aggressively treat aortic dissections, surprisingly, without additional upfront risk,” Ghanta explained. “Therefore, patients are benefiting from more extensive repair of aortic dissection, which may lead to improved long-term outcomes."
This study was recently published in the journal Annals of Thoracic Surgery.
Sources: Columbia University Department of Surgery, Elsevier