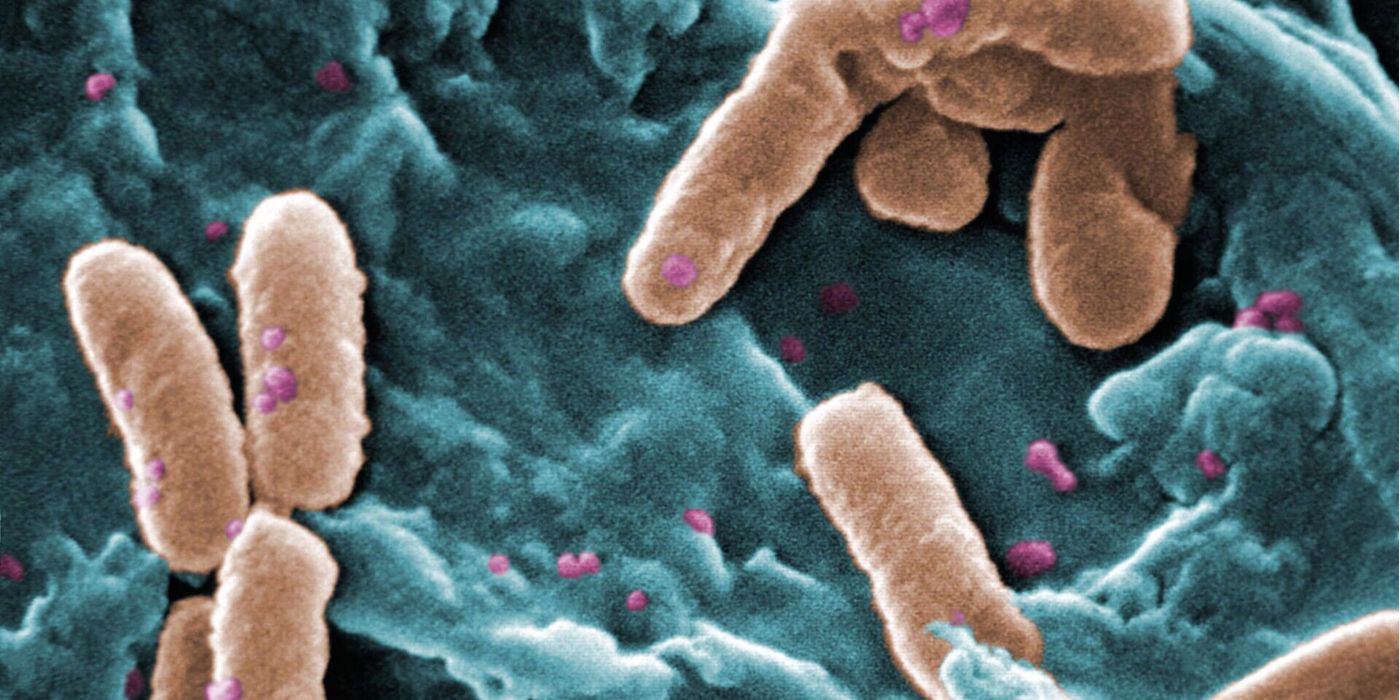
A Novel Therapeutic Target for a Severe Bacterial Infection
Pseudomonas aeruginosa (Pa) is an opportunistic human pathogen that can cause severe illness and even death in people that are hospitalized or have weakened immune systems. Further complicating Pa infections is the pathogen’s high rate of antibiotic resistance. Indeed, the CDC has given multidrug-resistant Pseudomonas a threat level of serious. Researchers at Stanford University found that a bacteriophage harbored by Pa contributes to its pathogenesis. They demonstrate in Science magazine that targeting this phage is a successful non-antibiotic therapy that leads to Pa clearance.
As an opportunistic pathogen, Pseudomonas aeruginosa exploits breaks in the host defenses to infection. Though Pseudomonas species normally inhabit soil, water, and vegetation, Pa can infect almost any compromised tissue. Pa is associated with chronic wounds and other infections such as urinary tract infections, respiratory system infections, dermatitis, soft tissue infections, bacteremia, bone and joint infections, gastrointestinal infections and a variety of systemic infections. Patients who are immunosuppressed or have cystic fibrosis, severe burns, or cancer are particularly susceptible to infection. Only a few antibiotics are effective against Pa, and multidrug-resistant strains are currently on the rise in hospitals. Thus, Pa represents a deadly and ever-increasing threat to patients in critical care.
Researchers in the Bollyky lab in the Division of Infectious Diseases and Geographic Medicine, Department of Medicine, at Stanford University, previously showed that a filamentous Pf bacteriophage (Pf phage) promoted chronic Pa infection in the lung by reducing inflammation. To build on that work, they sought to determine how Pf phage contributed to Pa infection in chronic wounds. After sampling chronic wounds in over one hundred patients, they detected Pf phage in 68% of the Pa-infected chronic wounds. Pf-positive strains of Pa were also more frequent in older chronic wounds and in the wounds of younger patients.
Using a mouse model of Pa-infected chronic wounds, they learned that Pf phage entered human cells, produced RNA and triggered viral immunity. This inhibited bacterial clearance and allowed Pa to persist in the wound. Since Pf phage was preventing Pa from being cleared by the immune system, they next vaccinated animals against Pf phage before Pa infection in their chronic wound model. Amazingly, prior vaccination against Pf phage allowed the immune system to clear Pa infection! Administering monoclonal antibodies against Pf phage to fresh wounds also resulted in successful clearance of Pa. Hopefully, similar results will be seen in patients.
“We envision that individuals newly diagnosed with cystic fibrosis or diabetes could be immunized against Pf phage to prevent subsequent Pseudomonas infections. It might even be possible to administer antibodies to burn victims before Pseudomonas infections set in.” -Paul Bollyky
Pseudomonas aeruginosa is a serious, potentially fatal pathogen in susceptible populations. It is surprising to learn that Pf phage has a pathogenic role in Pa infection. Future work will examine if other bacteriophages also modulate non-bacterial cells and if targeting Pf phage leads to immune clearance of multidrug-resistant Pseudomonas. Pf phage is a novel target for treatment of Pa-infected chronic wounds. Successful development of a Pf phage vaccine could mean that Pseudomonas aeruginosa chronic infections are no longer life-threatening.
The Science magazine article referred to in this article can be found here.
Check out the video above to learn more about Pa infections.