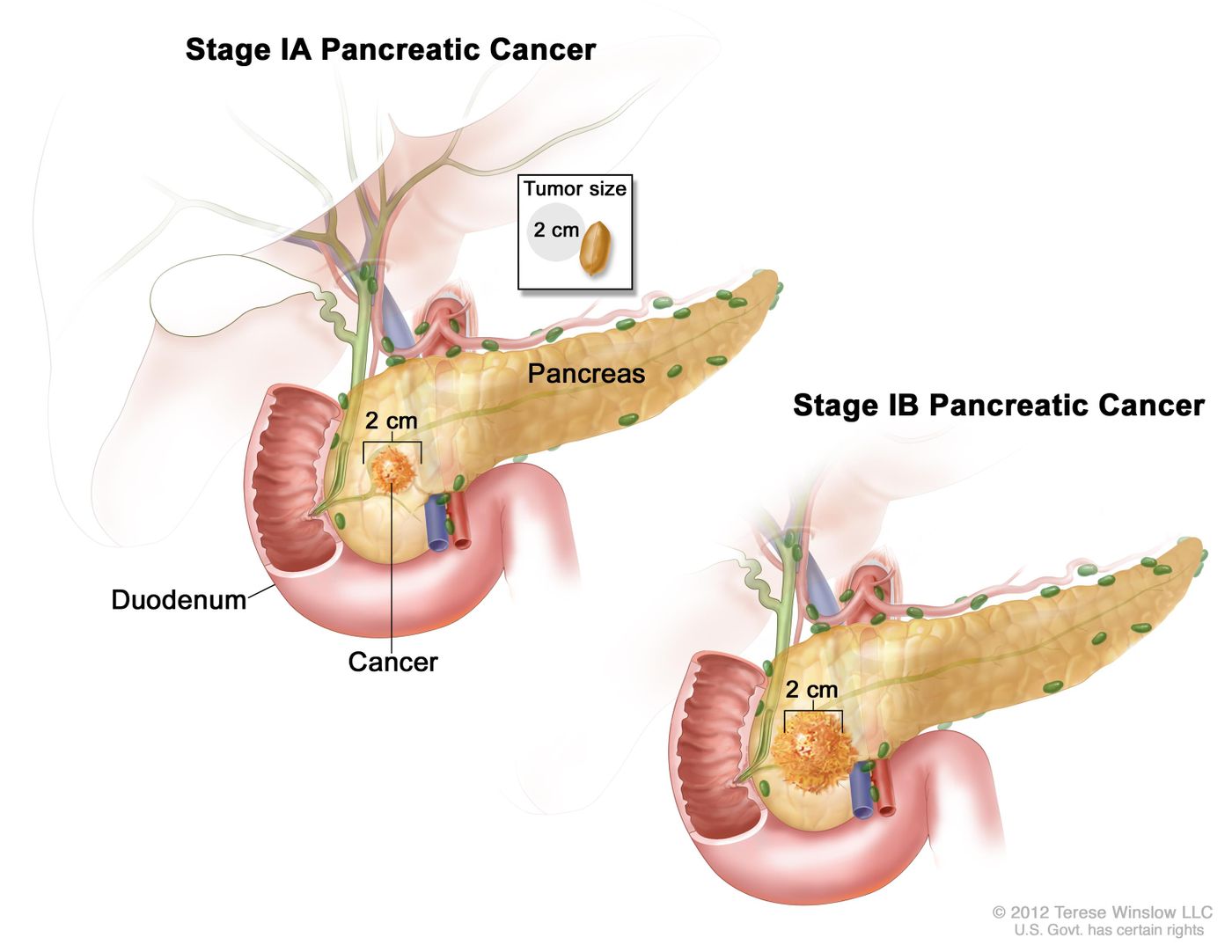
In 2016, the five-year survival rate for pancreatic cancer increased from seven to eight percent (American Cancer Society). Not a monumental increase, but scientists are still working on therapies to get the numbers even higher.
Scientists from the Abramson Cancer Center University of Pennsylvania School of Medicine, in their new preclinical study published in the journal
Cancer Discovery, investigated the potential of macrophages to break down protective walls around pancreatic tumors, also known as their microenvironment. They found that sending certain signals to macrophages with an experimental immune therapy can be successful in influencing them to strip away the protective parts that pancreatic tumors use to evade the harsh chemicals of chemotherapies.
“We’ve learned how antibodies that target a cell surface molecule called CD40 work with the immune system to tear back that wall,” said study leader Gregory Beatty, MD, PhD. Plus, the same antibodies were found to actually enhance the effect of chemotherapy once the tumor’s defenses were stripped away.
The ACC study recently published followed a previous study by the same researchers. In 2011 they illustrated the ability of CD40 to prompt monocyte and macrophage populations to destruct the tumor microenvironment. However, until their newest study, the team couldn’t pinpoint the precise mechanism behind the connection between CD40 and the immune cells.
Their new study involved mouse models of pancreatic cancer, and they were able to identify two immune factors released after CD40 antibody treatment. The suspects are chemokine ligand 2 (CCL2) and interferon gamma. While CCL2 recruits macrophage tumor infiltration, interferon-gamma prompts macrophages to release enzymes called metalloproteinases, which degrade the “fibrotic scaffold” of the tumor microenvironment, the structure that protects the cancerous cells from destruction by chemotherapy.
The tag team effort of CCL2 and interferon-gamma, as a result of CD40 antibody stimulation, leads to fibrosis degradation, identified by the scientists as the final blow in breaking down the tumor defenses.
While this discovery is promising in the fight against pancreatic cancer, the research team also realized that the timing of CD40 treatment followed by chemotherapy is extremely critical: too soon and patients are at risk for a 30 percent mortality rate, and too late and the chemotherapy is ineffective. They found that the “sweet spot” for chemotherapy delivery is five days post-CD40 treatment, where they saw the treatment well-tolerated and tumor cells shrinking and dying.
“Macrophages can be very potent killers of cancer,” Beatty said. “Since keeping them out of tumors is a challenge, why not harness their recruitment?”
Source:
University of Pennsylvania School of Medicine