How are macrophage immune cells activated during an inflammatory response when pathogens invade? Scientists thought they knew this and more, but recent studies from the Luxembourg Centre for Systems Biomedicine (LCSB) at the University of Luxembourg discovered something different.
Upon activation, macrophage metabolism pathways lead to the production of antimicrobial substances and fatty acids which deliver important resources during an infection. With their new discoveries into how these pathways work, the researchers, who study was recently published in the
Journal of Biological Chemistry may have also developed a new approach for treating chronic inflammatory diseases.
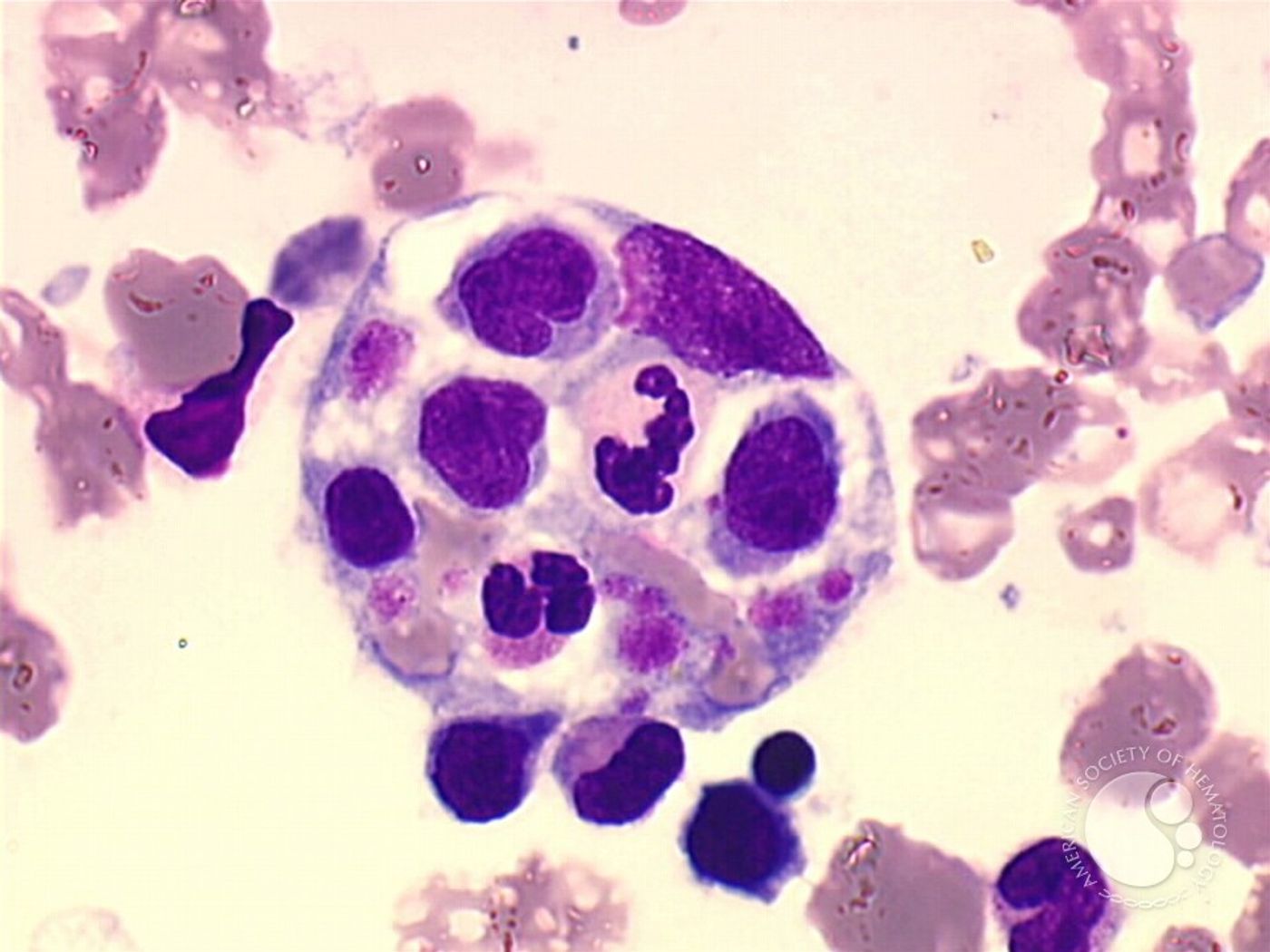
Macrophages are key immune cells of the innate immune system, the system of first-responder cells that react when pathogens invade. Macrophages are activated upon recognition of pathogen antigens or contact with cytokines, and their activation reprograms macrophage metabolism.
Hif1 is important protein for this very metabolism reprogramming, but it is also known to exist in cases of cancer. Cancer cells exist in an oxygen-poor tumor environment, which stabilizes Hif1 and prevents the tumor from being degraded. This causes less pyruvate to be introduced into the citric acid cycle, which is vital for producing energy for the body to perform multiple functions.
Apparently, Hif1 is also found in its stabilized forms in activate macrophages even though it is not an oxygen-poor environment. Previously, scientists thought this meant the metabolic pathways stemming from macrophage activation were similar to cancer cell pathways. However, the recent study from the University of Luxembourg instead showed that macrophages are able to facilitate pyruvate into the citric acid cycle despite Hif1 stabilization, allowing energy production to continue like normal.
"Conversion of pyruvate is a pivotal step in the inflammatory event, and thus presents a starting point for developing anti-inflammatory therapies," said Karsten Hiller, PhD. "This would be helpful for diseases associated with an excessive inflammatory response, such as allergies or septic shock."
Because of their ability, macrophages can also produce an “endogenous antibiotic” called itaconic acid and fatty acids needed for macrophage growth.
Source:
University of Luxembourg