Thousands of deaths in patients with hepatic cirrhosis result from bacterial infections that individuals with healthy immune systems could easily clear on their own. Without quick treatments of antibiotics, these people can quickly die from a treatable illness. Scientists knew that hepatic cirrhosis patients had compromised immune systems, but they couldn’t figure out why or how to repair the damage - until now.
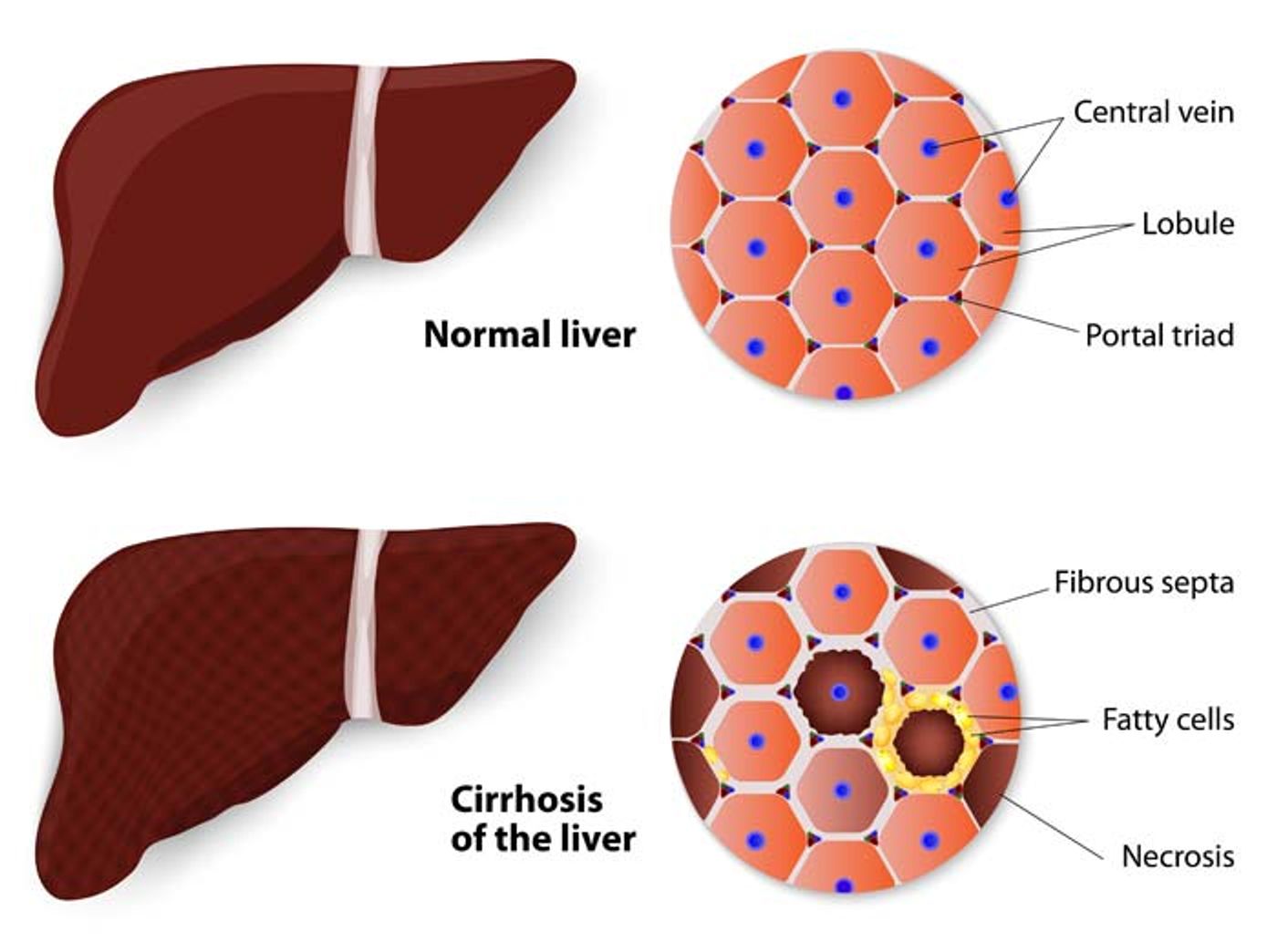
Patients with hepatic cirrhosis have damaged livers that are slowly but surely waning, a condition that results from alcohol abuse, fatty liver hepatitis, or chronic viral hepatitis. While it can take years for the liver to fail completely, without proper intervention or, in the worst case scenario a liver transplant, the disease is fatal.
In a new study from the University of Bonn and TU Munich, researchers might have finally found the way to prevent unnecessary deaths due to complications from hepatic cirrhosis. “One-third of the fatal cases of hepatic cirrhosis are attributable to bacterial infections,” said Dr. Jonel Trebicka, an experienced liver cirrhosis researcher. So what is stopping the immune system from handling the problem like it is designed to do?
As hepatic cirrhosis takes its toll on the liver, cells die and are replaced with connective scar tissue. The more liver cells that are replaced by scar tissue, the less blood is able to travel through hepatic blood vessels to the rest of the body. Blockages lead to elevated blood pressure in intestinal blood vessels, intestinal bacteria leak into the blood, and they travel to the liver, causing an abnormal immune imbalance. While previous findings brought this relationship to light, scientists still couldn’t make the connection between gut bacteria in the liver and the impaired immune function.
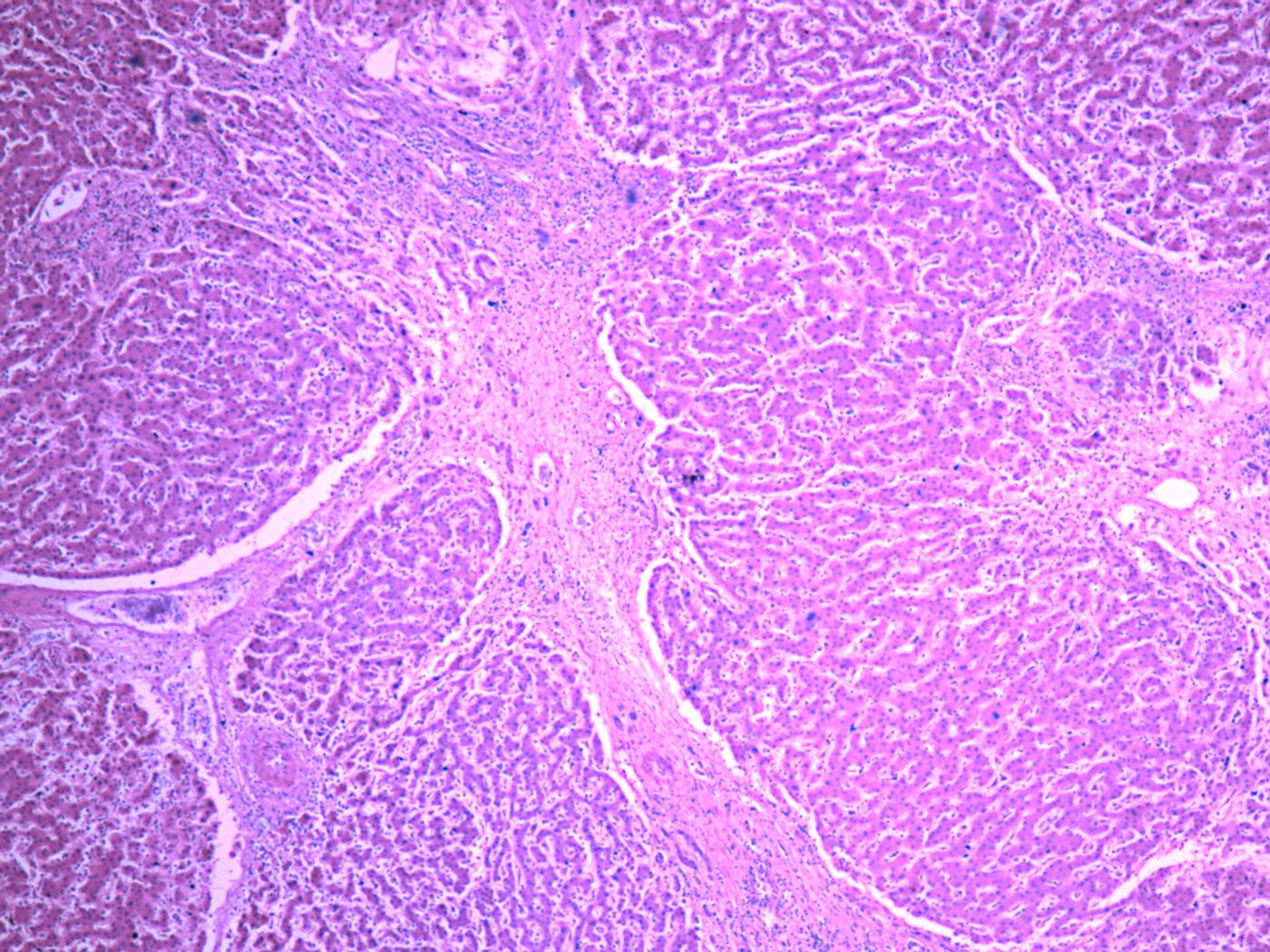
In the first stages of the study, researchers looked at mice with induced conditions of liver cirrhosis, first noticing that a large amount of type-1 interferon was regularly being produced by macrophages and monocytes in the liver, two immune cells vital for defense against infection.
Type-1 interferons are a type of chemical messenger called cytokines that have immunoregulatory roles within the response of T cells and Natural Killer cells to an incoming infection. Once the researchers introduced an infectious bacterium called
Listeria into the bloodstream of hepatic cirrhosis mice subjects, the production of type-1 interferon skyrocketed.
The large influx of type-1 interferon led to the release of another immunoregulatory factor called interleukin-10, which ultimately was to blame for the damage done to anti-bacterial functions of the macrophages. The infection ran rampant and killed the subjects.
The researchers performed the same experiment in human monocytes isolated from the blood of hepatic cirrhosis patients, achieving almost identical results. University Hospital Bonn researcher Dr. Zeinab Abdullah said that the study identified the “blind spot of the immune system that is responsible for the failure of the immune response to bacterial infections.”
The battle may be won, but the war isn’t over. In order to capitalize on the new understanding of the role of type-1 interferon and interleukin-10 in the fatal bacterial infections of hepatic cirrhosis patients, scientists must figure out how to prevent overproduction of these cytokines without disturbing the rest of the immune equilibrium that relies on these signals for regular function.
Researchers hope that by “reinvigorating” the immune system, patients with hepatic cirrhosis will be safe from fatal bacterial infections.
The study was recently published in the journal
Gut.
Sources:
University of Bonn,
PLOS Pathogens,
National Institute of Diabetes and Digestive and Kidney Diseases