Resilient T Cells Provide Cancer Treatment and Immunity
A key part of the process to create immunotherapies for the treatment of cancer involves rapid expansion protocols (REPs) and immune cells extracted from hosts. The idea is to put the immune cells back once they have been altered to be bigger and better at killing cancer, but previous targets, namely CD8+ T cells, lose their power after going through REPs. However, scientists have now identified a better target cell that could completely change immunotherapy approaches.
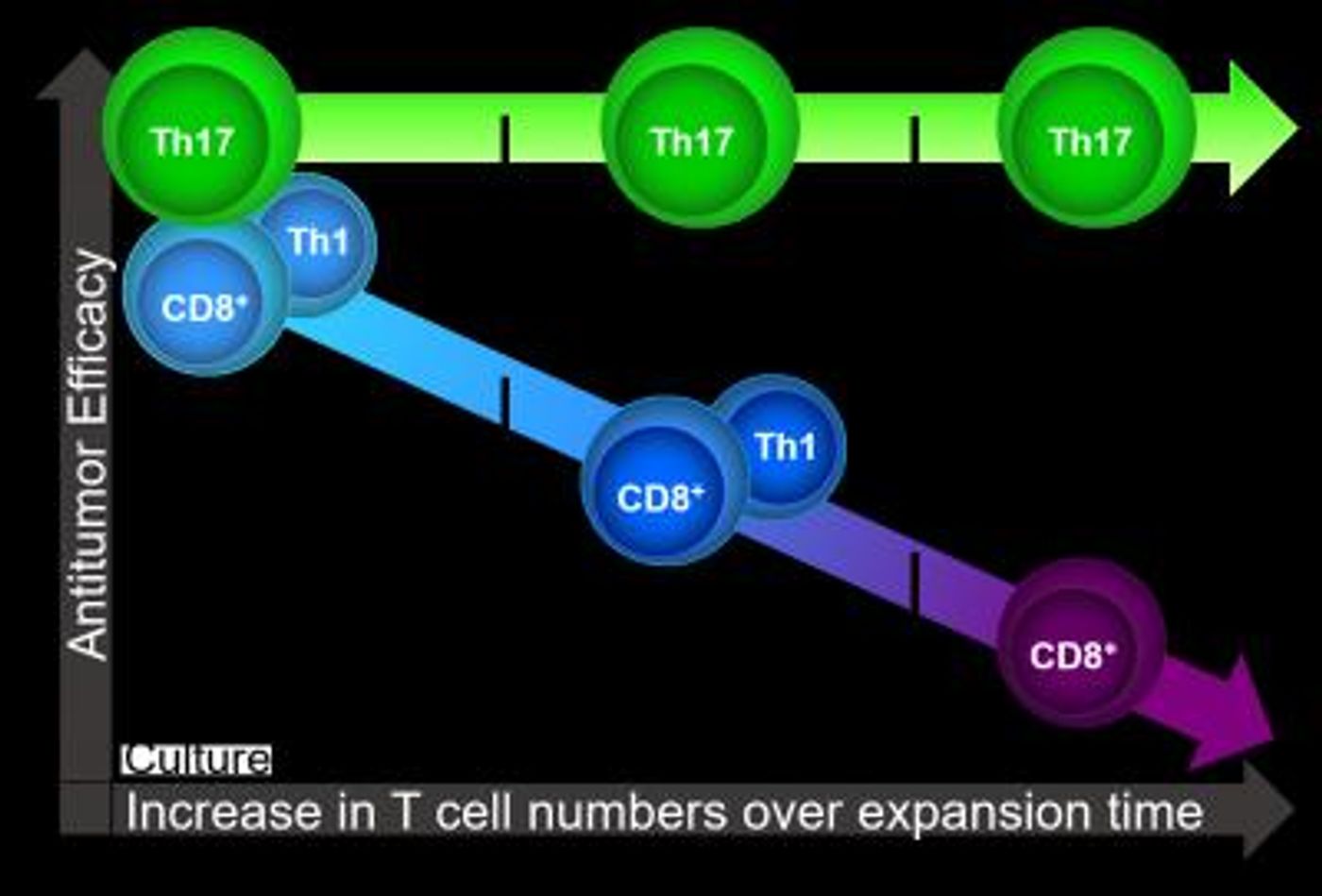
CD8+ T cells might not be cut out for long-term REPs, a necessary step in adoptive cancer immunotherapy (ACT). Th17 cells, though, appear to be uniquely eligible for the task; as compared to CD8+ T cells that show reduced efficacy after going through REPs, Th17 cells are more resilient and durable throughout the expansion process.
As an immunotherapy approach, ACT revolves around “The Three Es:” extracting, expanding, and enhancing host T cells for eventual return to the body to fight cancer. REPs are necessary but tough on T cells, and it can take up months to adequately prepare cells. After several weeks of preparation, CD8+ T cells often lose their power, but Th17 cells have been shown to be “resistant to expansion-induced degradation,” making them an obvious replacement for the seemingly “delicate” CD8+ cells.
"Th17 cells have a natural propensity to logarithmically expand without restimulation,” explained research leader Chrystal Paulos, PhD. “And, if we did restimulate them, this approach didn't dramatically impair the antitumor response as with CD8+ T cells."
What makes Th17 cells special? Stem cell-like properties. Paulos’s study showed that Th17 cells produced five thousand times the original number of cells when expanded for three weeks outside of the body thanks to their “natural propensity.”
In addition to retaining stem memory, resisting degradation, and effectively targeting melanoma in a mice model, after extraction and two weeks of expansion Th17 cells also remained in the tumor-bearing host after being returned to the body, indicating a protective effect for any possible recurrences of the cancer.
“When we rechallenged the same animals with another lethal tumor dose, these mice were protected but the control mice died quickly,” Paulos said. “Then we came back again 100 days later and gave these mice lung tumors and they were all still protected many months later."
Even more promising, the “remarkably potent antitumor response” seems to be extendable to the treatment of other cancer types, with an anti-cancer immunity effect “superior” to that obtained by classic applications of immunotherapy.