Nanoparticle "Immunoswitch" Reduces Cancer Growth
Johns Hopkins scientists have a new tool against cancer, and it’s a thousand times smaller than a human hair: a nanoparticle immunoswitch. New studies with this new approach have shown in mouse models to drastically slow - sometimes completing stopping - the growth of melanoma and colon cancer, and usage against other types of cancer are on the horizon.
The best defense is a good offense
The new approach improves upon the limitations of current immunotherapy techniques, specifically checkpoint inhibitor-based treatments. These drugs only work for some cancer patients and only against certain cancer types. For example, studies have shown that checkpoint inhibitors are about 30 percent effective against melanoma, bladder cancer, Hodgkin’s lymphoma, and non-small cell lung cancer. While giving a patient more of a drug might be more effective, concentrations of these drugs at a certain level can cause extremely undesirable side effects.
"The improvement here was to make, for the first time, a nanoparticle that can interact simultaneously with multiple types of cells in the complex tumor microenvironment, dramatically increasing its effectiveness,” explained Jonathan P. Schneck, MD, PhD from Johns Hopkins.
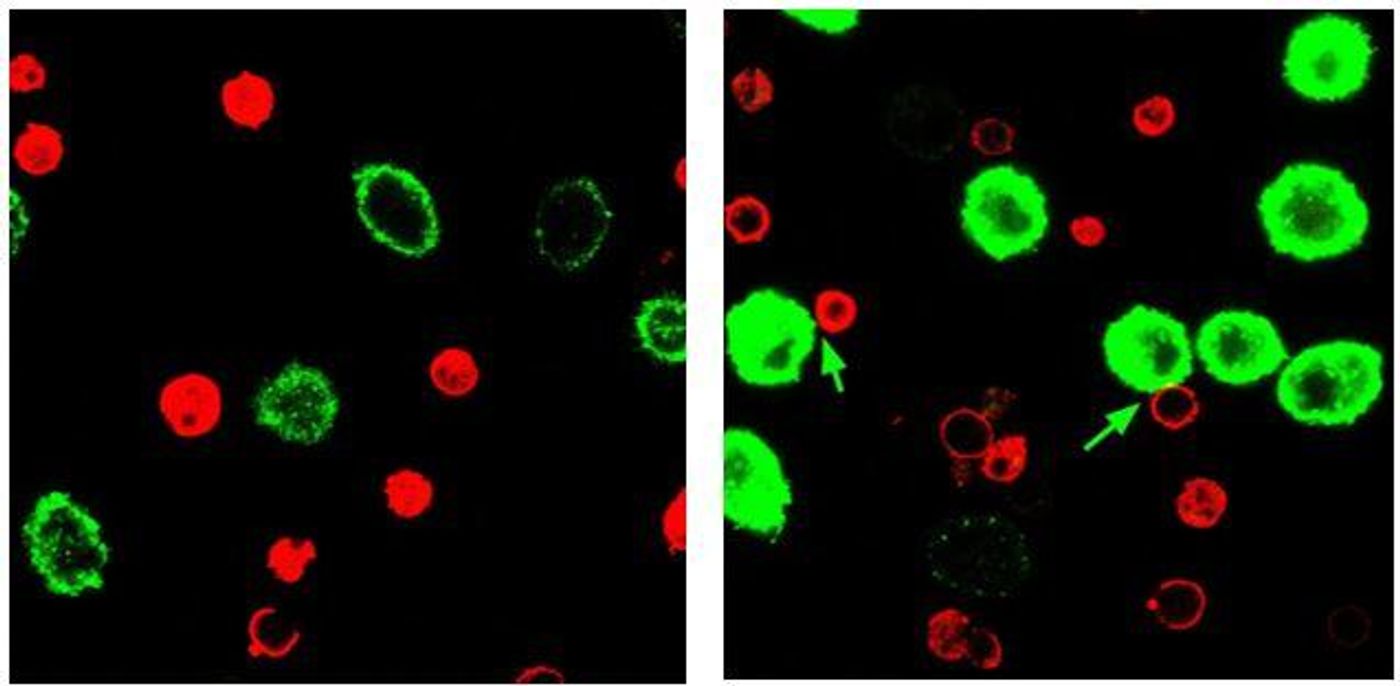
Schneck conducted his study with the nanoparticle immunoswitch using two different immunotherapy strategies, with two different types of antibodies bound to separate nanoparticles: programmed death ligand 1 (PD-L1) inhibitor and a T cell stimulator. Both nanoparticles were injected into a mouse model of melanoma, and Schneck soon observed the significant halt done to tumor progression. These mice lived much longer than their companions who received no treatment. Later, Schneck saw even more dramatic results in mouse models of colon cancer.
"The double-duty immunoswitch particles were clearly more effective than a mixture of nanoparticles that each targeted just one protein and acted in a synergistic fashion, but we don't yet know why," Schneck said. "It may be that the immunoswitch particles' success comes from bringing T cells and their targeted tumor cells into close proximity."
The particles owe their success, in part, to their “enhanced permeability and retention effect,” meaning they are more easily absorbed by tumor cells than by healthy cells, keeping the healthy cells safe. Plus, each individual nanoparticle could hold multiple antibodies at one time, allowing for a multifaceted attack on tumors and less of a chance of side effects.
In the future, Schneck and his team plan on improving the nanoparticle immunoswitch by looking for even more effective antibody combinations. And with the possibility of tailoring different therapies for specific types of cancer, this new technology could be a great tool.
The present study was published in the journal ACS Nano.
Source: Johns Hopkins Medicine