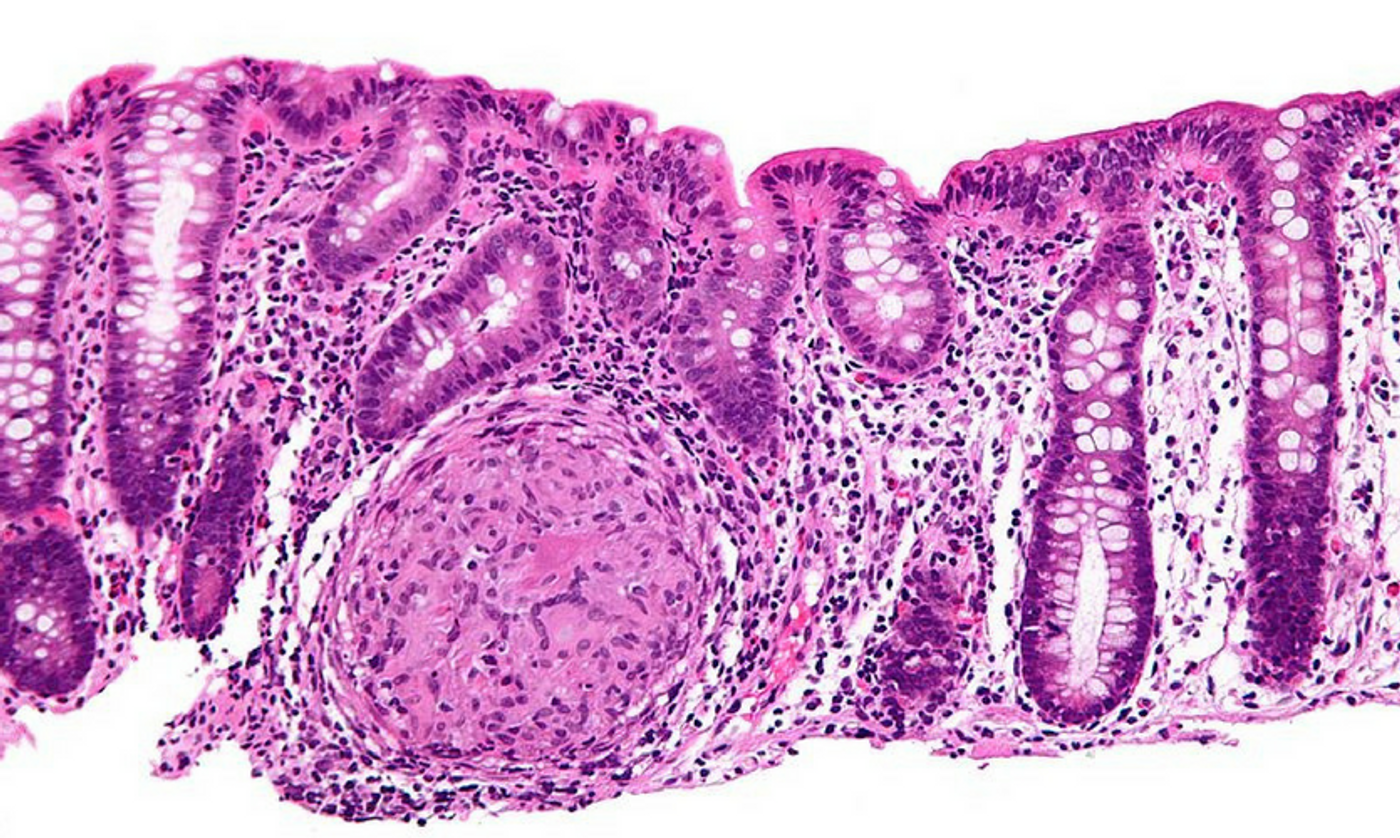
Circulating Immune Cells Accidentally Promote Crohn's Disease
Immune cells that travel from tissue to tissue need to be able to adapt to different tissues, including the high-acidity conditions of the gut necessary for digestion and protection from microbes that enter the body through food. From the Scripps Research Institute, scientists investigate what goes wrong when T helper 17 (TH17) cells fail to adapt.
TH17 cells produce an inflammatory chemical messenger called interleukin 17 (IL-17), which is helpful during pathogenic infections but harmful during healthy conditions. When and where TH17 cells release IL-17 depends on how they adapt to different tissues, so it’s easy to see how important it is for TH17 cells to adapt to tissue, especially in the gastrointestinal (GI) tract.
Lead researcher Mark Sundrud, PhD, hopes he and his team might learn to target areas like the GI tract specifically to dampen inflammation “instead of just generally suppressing the entire immune system."
TH17 cells, as they are involved in both immune defense and promotion of chronic inflammation, are often implicated in Crohn’s disease, an inflammatory bowel disease in the GI tract usually found at the end of the small intestine, an area called the ileum. Crohn’s disease affects about 700,000 people in the United States.
Sundrud’s new study builds off of previous research that found that TH17 cells boost expression of a gene called MDR1 as they enter the intestine, shown in human tissue samples. MDR1 is a protein that “transports chemotherapeutic drugs out of tumor cells,” but what does it do in the context of TH17 immune cells? Do TH17 use “different tools” to adapt to different tissues? Do they activate different genes in different places?
They found that MDR1 protects TH17 cells in the gut from bile acids, helping TH17 cells that need to adapt to the acidity of the gut. When they don’t, Crohn’s disease can develop.
Using a mouse model genetically modified to illustrate the importance of MDR1 in TH17 adaption in the gut, researchers saw that there was increased expression of the gene as TH17 cells enter the gut in mice with a normal MDR1 gene. But in mice who lacked the ability to express MDR1, TH17 cells were exposed to severe cell damage and led to Crohn’s disease.
Using human blood samples, researchers discovered a portion of human patients with Crohn’s disease who also had “severely impaired MDR1 expression.” A class of drugs called bile acid sequestrants brought T cell function back to normal and successfully treated the developing Crohn’s disease.
This study, published in the journal Immunity - both Identifies a cause of Crohn’s disease - cell damage from missing MDR1 expression - and provides a new treatment option for Crohn’s patients with this particular issue.
Sources: Immunological Reviews, Crohn’s & Colitis, Scripps Research Institute