Molecular Gene Switches Linked to Autoimmune Disease
A multitude of factors contribute to autoimmune disease, either those people are exposed to in their environment or those that come from their genes. In a new study from the Wellcome Trust Sanger Institute, scientists investigate the genetic portion of factors that increase the risk of autoimmune disease.
Type 1 diabetes, rheumatoid arthritis, and celiac disease are all examples of autoimmune diseases, where the body’s immune system mounts an inflammatory response despite there being no normal reason for it, like a bacterial or viral infection. The new study, published in the journal Nature Genetics, could provide new information for researchers looking to build better treatments for people with autoimmune disease.
During the study, researchers looked at more than just the genes associated with autoimmune disease; they also looked at those genes’ regulatory regions, so-called “molecular switches” that control each gene’s expression. By studying both components, they could uncover the whole picture of how genetic variation influences the immune response.
"We have found that the impact of genetic variants on how people's immune cells respond to a pathogen like Salmonella are condition-specific - they are only visible at certain stages of infection,” explained senior author Dan Gaffney. “This means that the effects of genetic differences in immune disorders could be missed in research, if scientists aren't studying both the genes and their control regions, the regulatory elements, of immune cells at all stages of an infection."
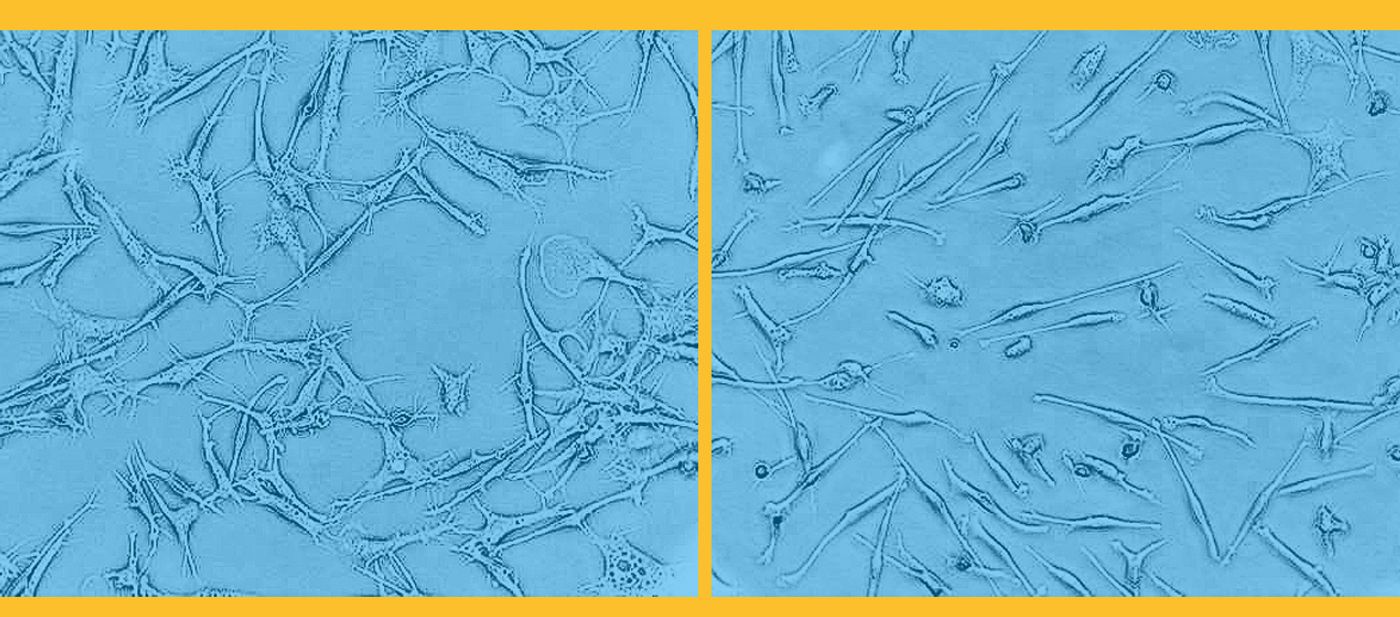
Gaffney and other studied macrophages, a type of white blood cell, which were differentiated in the lab from human induced pluripotent stem cells (HiPSCs). By using stem cells instead of macrophages isolated from the blood, researchers had the benefit of stem cell flexibility, studying the macrophages in four different states:
- Unstimulated
- After 18 hours of stimulation with interferon-gamma, a signaling molecule
- After five hours of infection with Salmonella
- After interferon-gamma stimulation and Salmonella infection
They analyzed the genes that were expressed during each stage of infection and monitored the activity of the regulatory region. “This novel combination of tools enabled us to see otherwise hidden effects of genetic variation on immune response,” said Kaur Alasoo.
They found that genetic variation affects the way immune cells prepare to respond to an infection. Some macrophages took longer to respond to the Salmonella infection than others. This is partly a result of “enhancer priming,” an occurrence characterized by an alteration in the regulatory region where some genes were activated before the Salmonella infection actually occurred,
The effect of enhancer priming is beneficial when providing a quicker than normal response to an infection, but the same response in the absence of an infection could produce an autoimmune reaction. Based on the study’s findings, researchers hope to learn how to interfere when enhancer priming leads to autoimmune disease and leave it alone when it improves the immune response to infections.
Source: Wellcome Trust Sanger Institute