During Deadly Lung Infections, the Nervous System Gets in the Way
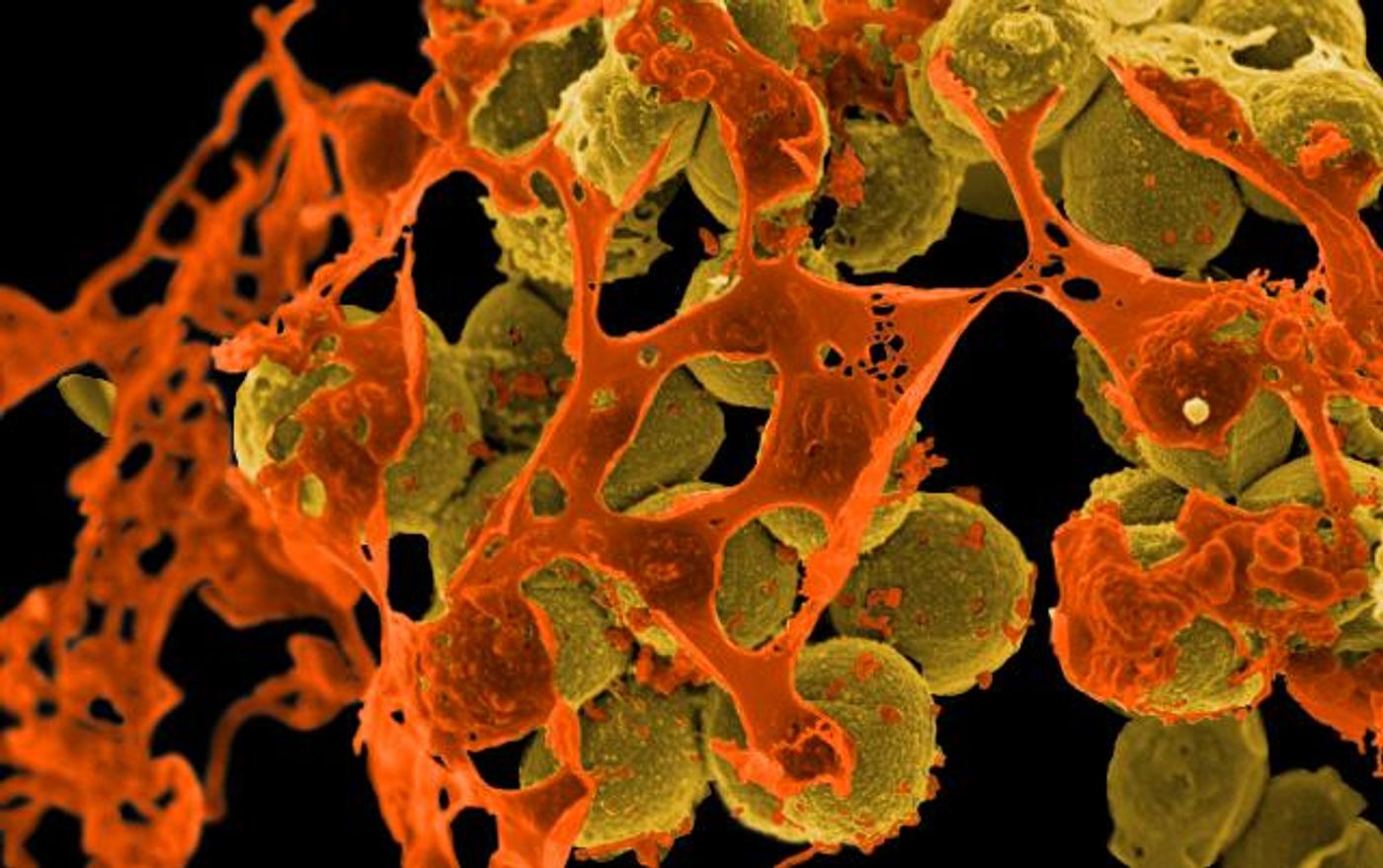
A new, non-antibiotic approach to targeting bacterial infections like Staphylococcus aureus - which are notoriously difficult to treat - may stem from inhibiting neuron activity. In a new study from Harvard Medical School, scientists show how neurons disrupt the immune response during an infection in the lungs.
While in the past scientists thought that the nervous and immune systems rarely crossed paths during an infection, the new Nature Medicine shows that nothing could be farther from the truth. Neurons carrying nervous signals in the lungs suppress the immune response during an S. aureus infection. This pathogen is already particularly dangerous due to its resistance to antibiotics and tendency to afflict weak and immunocompromised hospital patients.
"The traditional delineation between nervous and immune systems is getting blurry and our findings underscore the idea that these two systems cross-talk to regulate each other's function," said senior study investigator Isaac Chiu. "As we move forward, immunologists should think more about the role of the nervous system, and neuroscientists should think more about the immune system."
Harvard scientists conducted their study in mice, groups of which either had normal neurons in the lungs or neurons disabled with genetics or chemicals. Researchers compared each group’s ability to respond to drug-resistant S. aureus infections, including immune cell recruitment, body temperature control, and overall survival.
Researchers began the study theorizing that nerve cells would promote the immune response in the lungs to help fight bacterial infections. Neurons in the lungs are responsible for informing the brain when they sense things like mechanical pressure, inflammation, temperature changes, or chemicals. We experience this in the form of pain, airway constriction, and coughing. However, neurons apparently also prevent immune cells in the lungs from effectively fighting back against infection.
Researchers found that mice with disabled lung neurons were overall more effective at recruiting immune cells, clearing bacteria, and surviving. Specifically, infected mice with disabled neurons were better than mice with normal neurons at recruiting cytokines and neutrophils. Additionally, the neurons they recruited were more effective at fighting infection.
"We observed a striking difference in neutrophil presence and behavior between the two groups," explained first author Pankaj Baral. "Neutrophils in mice with disabled neurons were simply better at doing their job."
On the other hand, researchers saw increased production of an immune signaling molecule, a neuropeptide released by neurons called CGRP, in mice with intact neurons, while production of CGRP was nearly absent in mice with disabled neurons. CGRP disrupts both neutrophil recruitment and cytokine production, and it weakens immune cells’ bacteria-killing powers. Thus, inhibiting CGRP production improved the immune response to S. aureus.
Going forward, scientists will use the findings from their study to develop different non-antibiotic approaches to treating dangerous infections like S. aureus. They will have to consider that there may be different classes of sensory neurons, some that help and some that inhibit the immune response during infection. Or, S. aureus and other bacteria could be capable of turning sensory neurons against the lungs, inhibiting the immune response so the bacteria can continue infecting cells.
"With the rapid emergence of drug-resistant organisms, such as methicillin-resistant Staph aureus, nonantibiotic approaches to treating bacterial infections are sorely needed," Chiu said. "Targeting the nervous system to modulate immunity and treat or prevent these infections could be one such strategy."
Source: Harvard Medical School