Personalized Anti-Inflammatory Treatment for Type 1 Diabetes
The diversity of proteins in the blood that promote inflammation in people with type 1 diabetes and related kidney disease calls for personalized treatments tailored to an individual’s specific inflammatory protein profile. To achieve this goal, Medical College of Georgia at Augusta University scientists screened patients’ blood samples for 12 inflammation-promoting proteins.
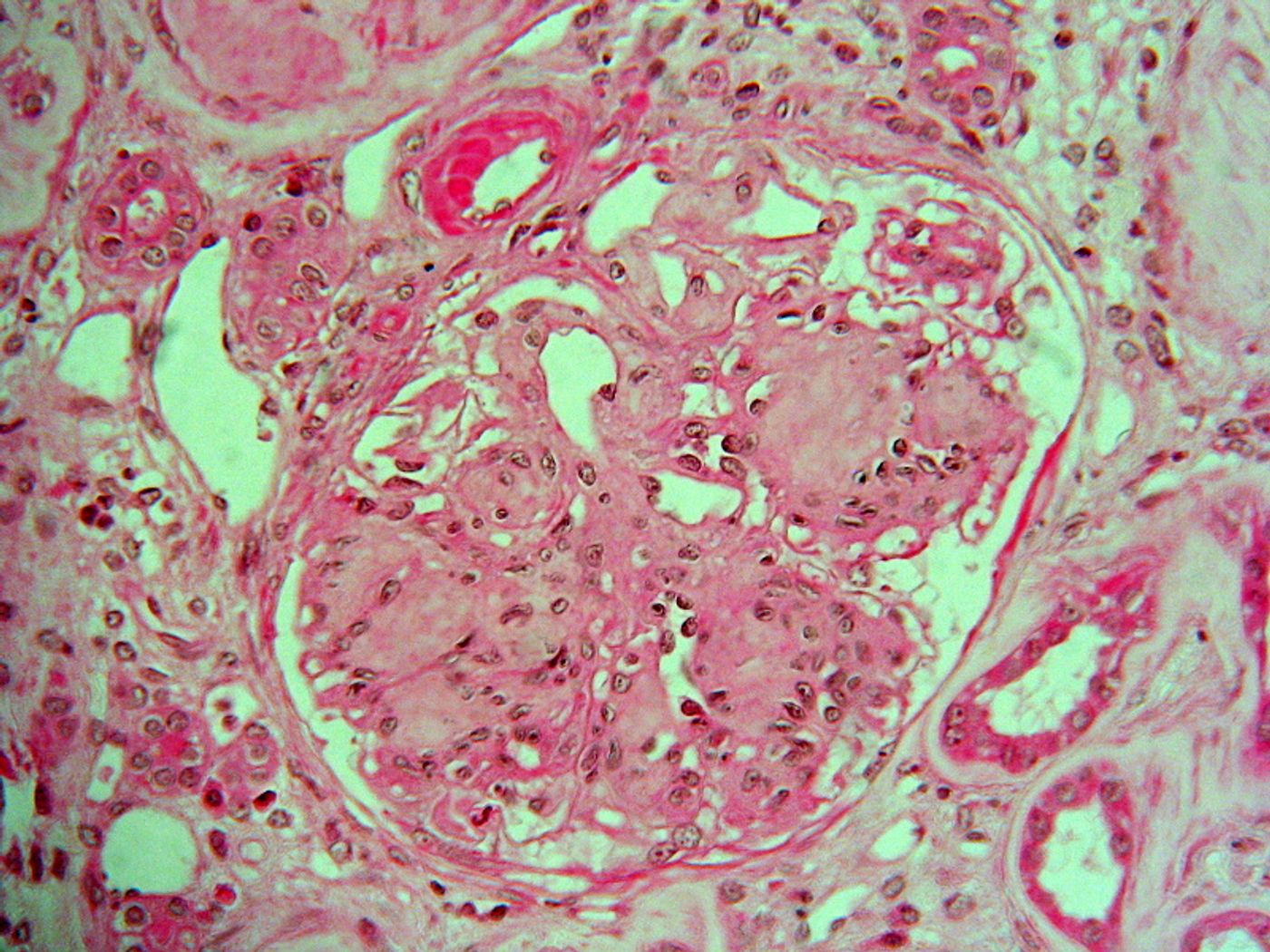
Perpetually high levels of blood glucose characteristic of type 1 diabetes trigger the inflammatory response, which can damage organs, nerves, and blood vessels. This includes the kidneys. Over time, high levels of blood glucose can damage the kidneys, which are responsible for cleaning the blood of waste and fluids. Without proper kidney function, waste products build up in the body instead of exiting via urine.
Proteins that drive those perpetually high blood glucose levels are diverse even among people with that same condition. So scientists believe that patients would benefit from an anti-inflammatory treatment designed specifically for them. Additionally, learning more about the diversity of inflammation-promoting proteins could help scientists identify biomarkers for diagnosing diabetes-related kidney disease and predicting the likelihood of who will develop it. And lastly, this study will help researchers test the effectiveness of existing treatments and prevention strategies.
"We all think that prevention of inflammation will help prevent or delay diabetic kidney disease and probably other consequences of type 1 diabetes," explained corresponding author Dr. Jin-Xiong She. "But not all inflammation is the same and not all patients have the same inflammation, even patients with the same condition like type 1 diabetes.”
To effectively prevent or treat type 1 diabetes and related kidney disease, scientists first had to identify the proteins responsible for driving inflammation in these conditions. Then, they can design drugs that specifically target those proteins; not every type 1 diabetes patient will have the same inflammation-driving proteins.
“That is really predictive, preventive personalized medicine and that is exactly what we are trying to enable," She said.
She and the other researchers analyzed the blood levels of inflammation-driving proteins in 89 patients with diabetes-related kidney disease and 483 patients with diabetes but no kidney disease. They found that ten proteins elevated in diabetes patients with kidney disease. Those proteins in the TNF-alpha and IL-6 families were significantly elevated in 40 percent of patients - compared to diabetes patients with no kidney damage. Another 40 percent had moderately elevated levels of the same proteins. Thus, treatment for TNF-alpha and IL-6 protein families might be effective for the first group, but not for the second group.
Researchers also saw that C- reactive protein (CRP) and serum amyloid A (SAA) were not significant inflammatory mediators compared to other proteins. However, these two proteins are commonly measured in hospitals for diabetes-related kidney disease.
Going forward, researchers are interested in both larger studies with type 1 diabetes patients and initial studies with type 2 diabetes patients. Using the current findings, they are interested in investigating the best method for targeting the inflammatory proteins most significantly involved in exacerbating diabetes and diabetes-related kidney disease.
The present study was published in the journal Frontiers in Immunology.
Sources: MedlinePlus.gov, Medical College of Georgia at Augusta University