Killer Antibiotic-resistant Pathogen Isolated in the US
For decades, people have relied on antibiotics and similar drugs to treat microbial infections, and those drugs have been very effective until recently. Their widespread and sometimes irresponsible use has made them less effective, and antibiotic-resistant microbes are seen as a rising public health threat. Of the two million people that are infected with these pathogens every year, around 23,000 patients die; that number is projected to rise to ten million by 2050. Now researchers at the Emory Antibiotic Resistance Center have investigated a new strain of highly resistant bacteria to learn more about it, and how to combat it.
"The problem of antibiotic resistance is becoming increasingly alarming. The combination of increased virulence and multidrug resistance makes the situation worse," said Dr. David Weiss, director of the Emory Antibiotic Resistance Center, which is featured in the video below.
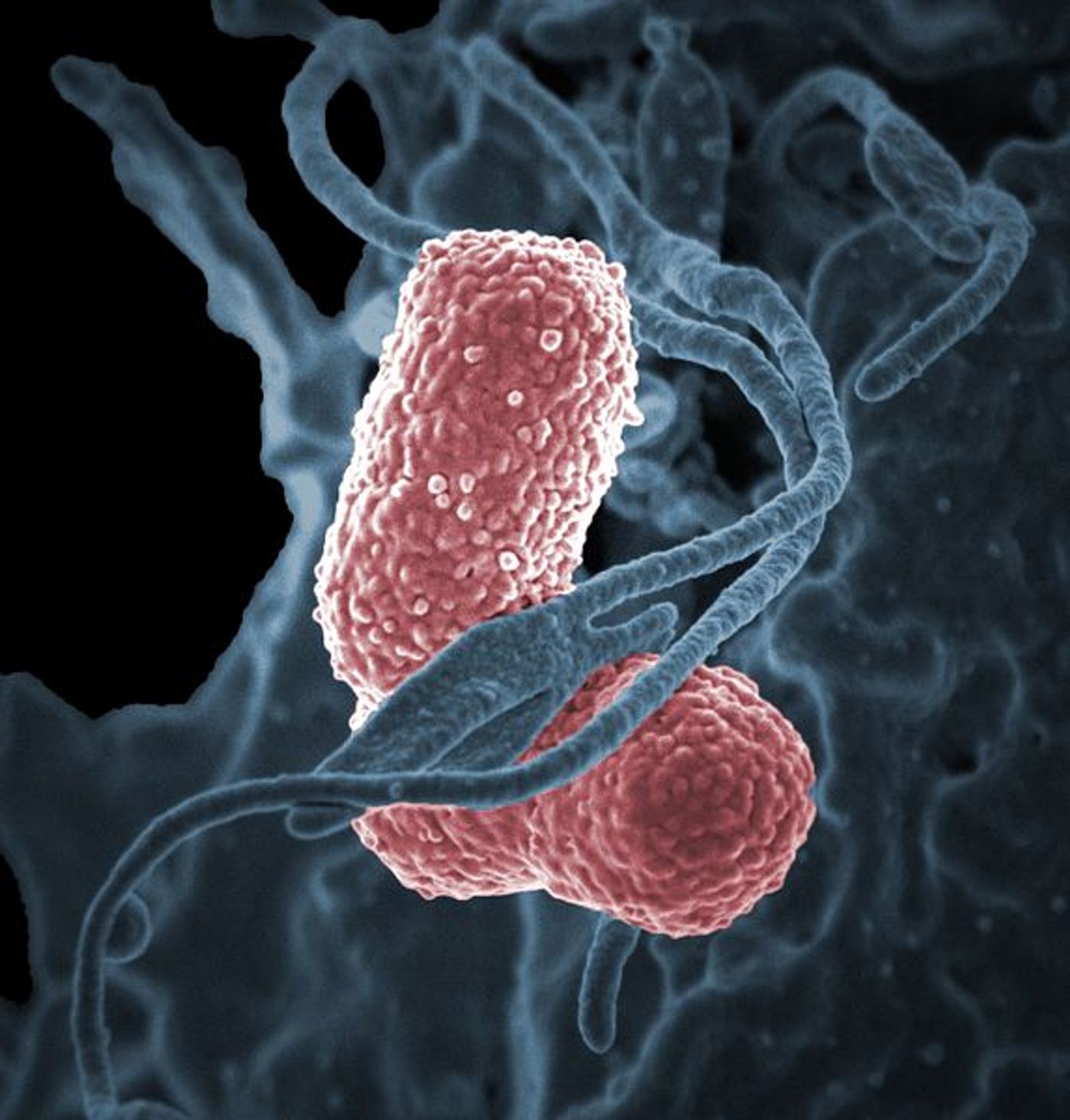
The researchers sequenced the entire genome of the bacterium, which is the first known strain of carbapenem-resistant hypermucoviscous Klebsiella pneumoniae, with enhanced virulence (indicating its likelihood to cause infection) and heteroresistance to colistin. Colistin is a last-resort antibiotic that is used only in dire cases. The bacterium is a member of the carbapenem-resistant Enterobacteriaceae (CRE) superbug family, which the CDC considers an urgent threat.
Heteroresistance characterizes a mixed population in which some cells are resistant to a drug and others are not. That can render an antibiotic treatment ineffective.
In 2016, a hospital in China experienced an outbreak from hypervirulent, carbapenem-resistant, K. pneumoniae. An analysis was recently reported in Lancet Infectious Diseases.
"The isolate we are studying is not nearly as virulent in a mouse model as the bacteria from China," said Dr. Weiss, "However, finding the combination of antibiotic resistance and enhanced virulence from a clinical isolate in the United States (New York) is still alarming."
The scientists suggested that doctors and clinics should be watching out for this kind of bacteria; it has the potential to be very dangerous in healthcare settings.
The research team, which included Jessie Wozniak, a Microbiology and Molecular Genetics graduate student at Emory University School of Medicine, used a simple “string test’ on 265 isolates of carbapenem-resistant K. pneumoniae bacteria.
"The string test is very low-tech. You take a loop, touch it to the bacterial colony, and pull back. The hypermucoviscous one looks like a string of cheese being pulled from a pizza,” Wozniak explained. The stretchiness comes from a compound the microbes make, capsule polysaccharide. Previous work has linked the chemical to virulence.
The researchers also used whole-genome sequencing to find several antibiotic resistance genes the bacterium carried, which were in a new arrangement. Similar isolates of K. pneumoniae from Asia have a different set.
The team stressed that these findings could indicate that colistin may not be useful much longer as a treatment of last resort, and that heterogeneous populations of bacteria could help explain why the treatment fails in some patients. Tests that are meant to indicate how effective colistin will be may also not be reliable when confronted with these heteroresistant bacteria.
Sources: AAAS/Eurekalert! via ASM, CDC, mBio