The Rise of Carbapenem Resistance
European scientists are warning about the rise of a dangerous group of microbes that resist the effects of an important class of drugs called carbapenems. These drugs, which include doripenem, ertapenem, imipenem, and meropenem, work against many different kinds of pathogenic microbes and are used when other drugs fail. However, bacteria are becoming resistant to them; such pathogens are now thought to pose a significant threat to the patients in the healthcare clinics of every country in the European Union. A Rapid Risk Assessment about these conclusions has been released by the European Centre for Disease Prevention and Control.
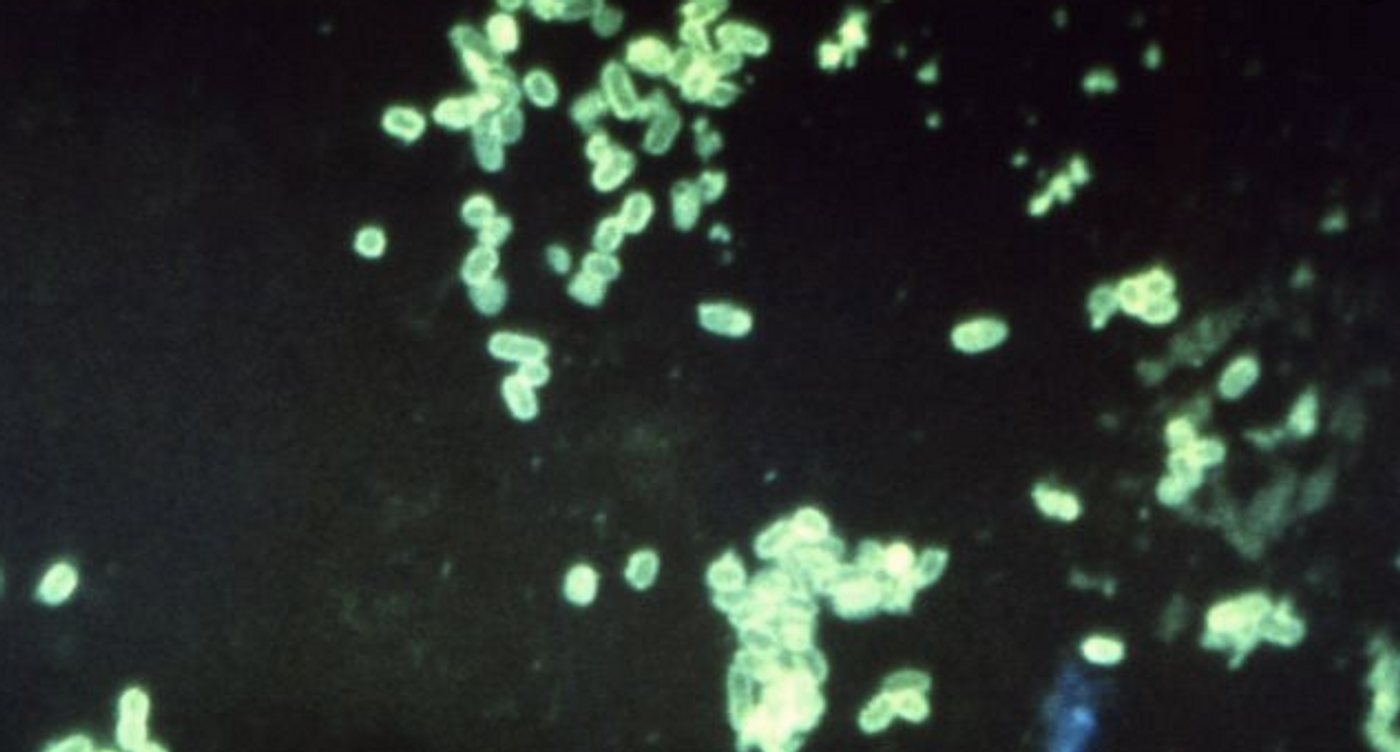
First reported in the nineties, resistance to carbapenems has since become more common and spread to more areas of the globe. It’s one type of bacteria, Enterobacteriaceae, that is gaining the upper hand on the drugs, as they become carbapenem-resistant Enterobactericaeae, or simply CRE. CRE infections pose a real danger.
"We should be very concerned about the rise in carbapenem resistance in the EU/EEA as there are very few options for the treatment of patients with CRE infections,” said Dominique Monnet, the Head of ECDC's Antimicrobial Resistance and Healthcare-Associated Infections Programme. "In recent years, the proportions of carbapenem resistance in Klebsiella pneumoniae - a type of Enterobacteriaceae - rapidly increased to high levels in Greece, Italy, and Romania. The same could happen to other EU/EEA countries if appropriate measures are not taken. But the spread of CRE can likely be controlled in most countries through the implementation of appropriate prevention and control measures in hospitals and other healthcare settings."
CRE infections of the bloodstream and urinary tract are not unusual in hospitals, and they can make a patient's stay in the hospital longer and increase the cost of treating patients. They can also contribute to failures in treatment and cause death; treating these infections is challenging, and there are limited options, especially for patients in hospitals.
While the prevalence of these infections is still low, in Europe the national percentages of bloodstream infections caused by Klebsiella pneumonia that is carbapenem-resistant ranges from zero to 67 percent. The highest rates are in Romania, Italy, and Greece; those countries have rates of 31, 34 and 67 percent, respectively.
When antibiotic resistance becomes a frequent occurrence, that antibiotic ceases to be recommended for use. There aren’t any antibiotics that are a good choice for fighting a CRE infection.
Global travel and patient transfer can introduce CRE into new countries or countries where the prevalence is low. Some places, like Southeast Asia and India, have high levels of CRE.
It will be important for clinics to monitor for these infections carefully, and to mount an effective response when they occur. The ECDC's Rapid Risk Assessment highlights steps doctors can take.
Sources: AAAS/Eurekalert! via ECDC, Merck Manuals