Gut Microbes Linked to Development of Liver Disease
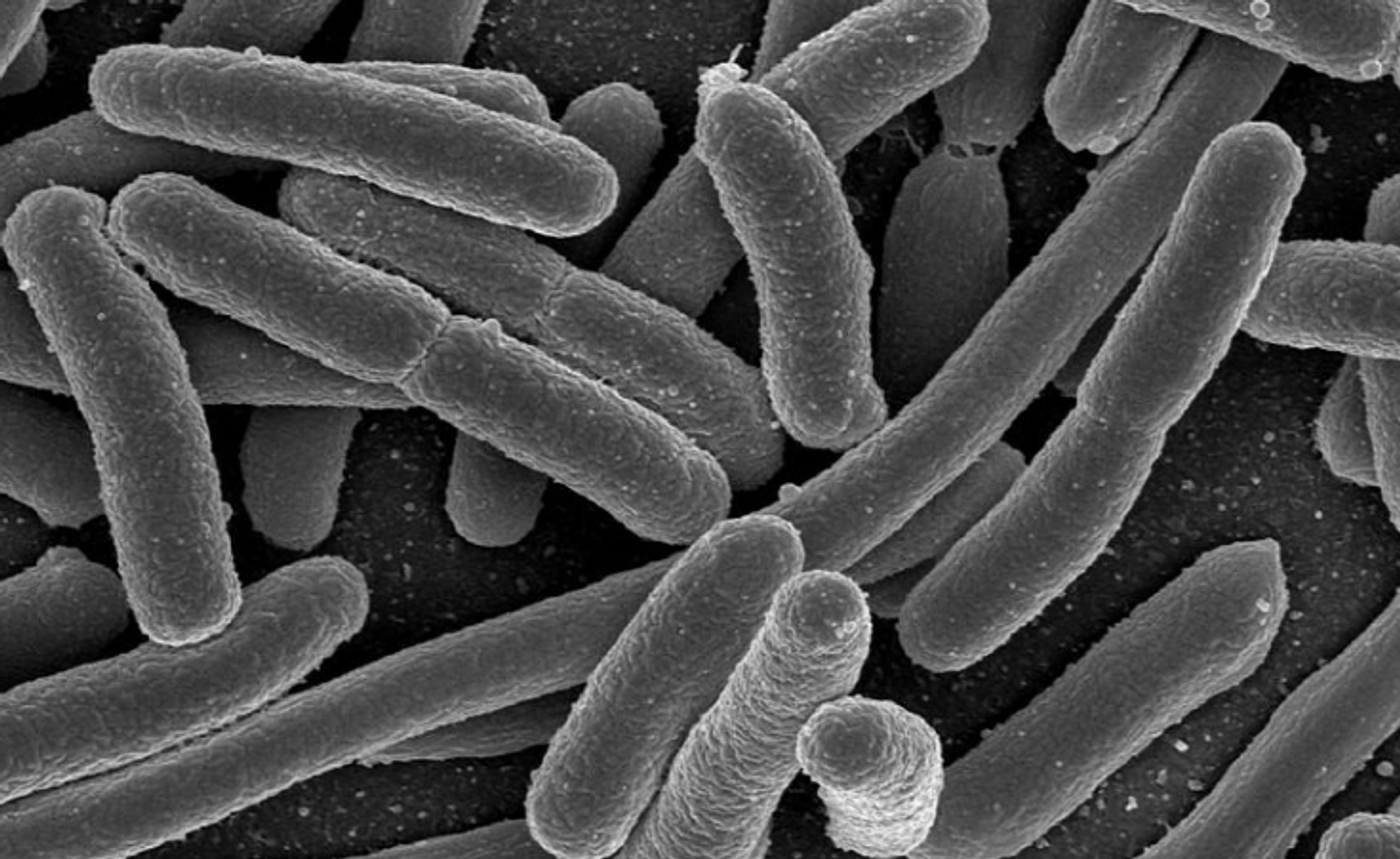
The community of microbes that lives in our gut, the gut microbiome, release compounds, and new research has suggested that early signs of liver disease could be found by assessing those chemicals. The findings indicate that not only do the bacterial strains in the microbiome have something to tell us about health and disease, we can also learn from the stuff they secrete. It may one day be possible to use a blood test to look for these secreted chemicals, some of which may be strongly associated with a disease. This work has been reported in Nature Medicine.
The research began with an international team looking to learn more about how the gut microbiome is connected to the development of non-alcoholic fatty liver disease (NAFLD). The disease starts with an accumulation of fat in the liver and subsequent scarring. That can lead to cirrhosis, in which the organ shrinks and the risk of disease rises. Few symptoms occur before the disease reaches advanced stages, and it’s estimated that one on three adults is in the early stages. It can be diagnosed with a blood test and ultrasound, but it may also go unnoticed.
In this work, the scientists found that the onset of NAFLD is linked to the presence of a chemical called phenylacetic acid (PAA) in the blood. Gut bacteria produce PAA, which could be a useful biomarker.
"Through this work, we may have uncovered a biomarker for the disease itself. Overall, it demonstrates the microbiome is definitely having an effect on our health,” said the leader of the work, Dr. Lesley Hoyles, from the Department of Surgery & Cancer at Imperial College.
Th team found the biomarker by assessing samples from one hundred obese women that had fatty livers, as well as healthy patient samples. PAA was found to be increased in the fatty livers compared to healthy livers. Changes in the gut microbiome and NAFLD were also connected; in the case of more advanced disease, the diversity in the microbiome was reduced.
The investigators found that there were far fewer active bacterial genes in fatty liver, echoing previous research that looked at bacterial diversity in obese people. It’s known that the bacteria we carry bring about ten million genes to our bodies, about 500 times more than our own genes. That genetic diversity is lost in people with metabolic disorders.
"The collapse in genetic diversity of the gut bacteria observed in metabolic disorders is worrying. Our gut microbes seem to lose the ability to make beneficial compounds and instead they start producing the ones setting us on a disease track,” said senior author Dr. Marc-Emmanuel Dumas, from the Department of Surgery & Cancer.
"The concept that we could use chemical signals produced by our gut bacteria to spot disease is an exciting one. It opens the possibility that simple screening test at a GP clinic could one day be used to spot the early signs of disease. But these kinds of tests may still be a number of years away from the clinic,” he continued.
"We now need to explore this link further and to see if compounds like PAA can indeed be used to identify patients at risk and even predict the course of disease. The good news is that by manipulating gut bacteria, we may be able to prevent fatty liver disease and its long-term cardiometabolic complications,” he added.
The team used an animal model for further study; when healthy mice were exposed to PAA, fat accumulated in their livers. When they performed fecal transplants, which moved gut bacteria from fatty liver patients to mice with antibiotic-cleared microbiomes, those treated animals developed fatty livers.
The researchers have suggested that a decrease in microbial diversity, and by extension, the loss of certain important gut microbes or a shift in the bacterial population is connected with disease development. The compounds made by those bacteria may be acting as a biomarker of that shift or might be a part of the disease development, which one is still unclear.
"The scientific literature shows that the microbiome changes in a range of diseases. But it may be a case of 'chicken and egg', and not necessarily cause and effect,” noted Hoyles. "It's clear that the microbiome influences us because at any one time we have around 200 metabolites in our circulation from our gut bacteria, so they have long-term effects and may be influencing disease."
Sources: AAAS/Eurekalert! Via Imperial College London, Nature Medicine