Fungal Infections Impair Brain Function in a Mouse Model
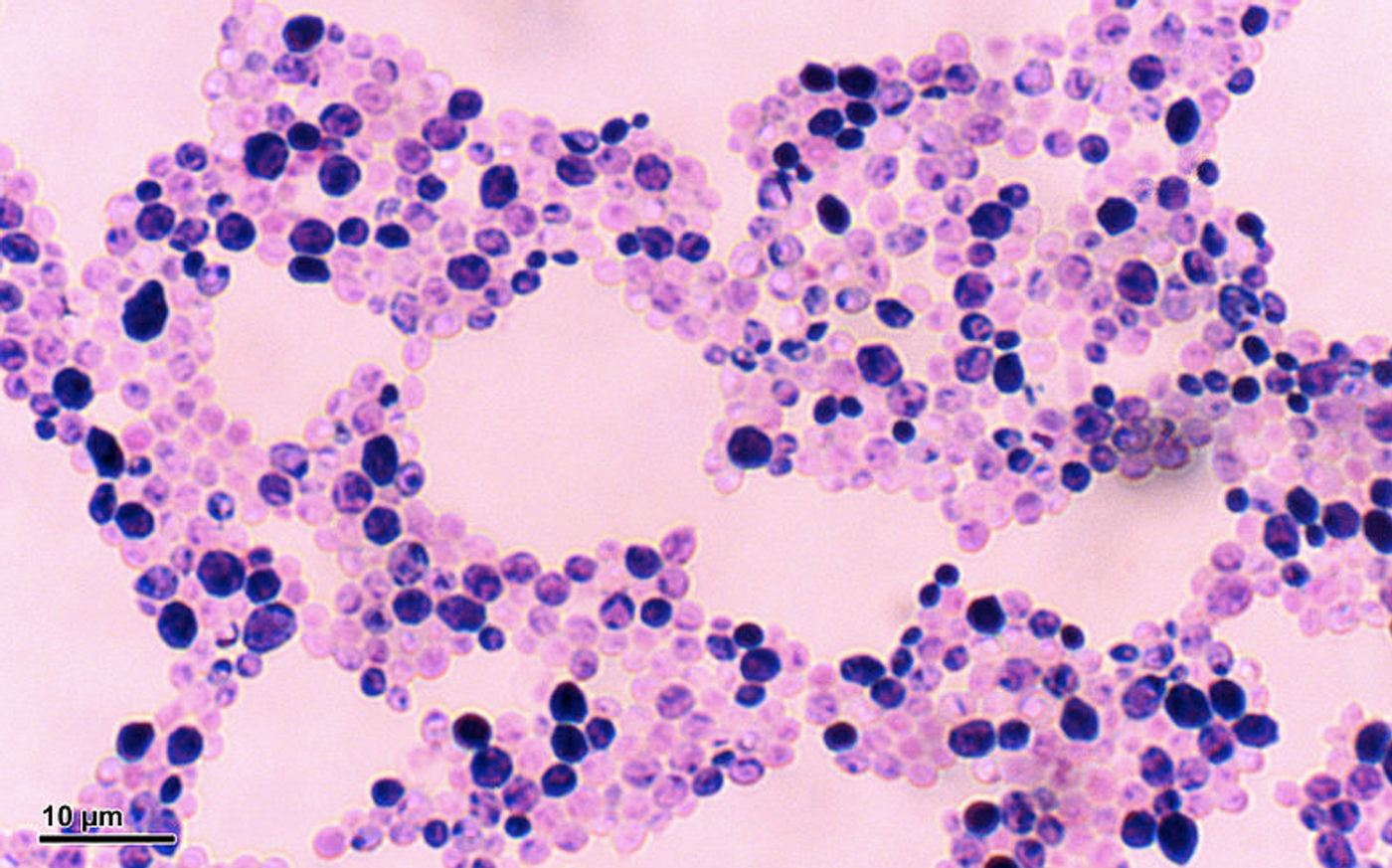
Many types of fungi in our environment are being linked with increasing frequency to a wide array of health problems, like chronic inflammatory disorders such as eczema, colitis, or laryngitis. A team of researchers at Baylor College of Medicine has now used a mouse model to show that Candida albicans, a common yeast that’s a type of fungus, is able to get across the barrier protecting our central nervous system. The fungus caused structures that resembled granulomas to form in the brain and mild memory impairment in those mice. The granulomas had similarities to Alzheimer’s plaques, suggesting that researchers should follow up on these findings to learn more about what a chronic C. albicans infections may do to the brain.
"An increasing number of clinical observations by us and other groups indicates that fungi are becoming a more common cause of upper airway allergic diseases such as asthma, as well as other conditions such as sepsis, a potentially life-threatening disease caused by the body's response to an infection," said corresponding author Dr. David B. Corry, professor of medicine-immunology, allergy and rheumatology and Fulbright Endowed Chair in Pathology at Baylor College of Medicine.
Corry noted that fungal infections that cause sepsis or allergic disease have been linked to an increased risk of dementia. "These observations led us to investigate the possibility that fungus might produce a brain infection and, if so, the consequences of having that kind of infection," noted Corry, who also is a member of the Dan L Duncan Comprehensive Cancer Center.
For this study, the research team created a mouse that modeled low-grade C. albicans fungal infections; it would not result in a major disease but could illustrate the long-term impact of the infection on the brain. The mice received an injection of C. albicans to their bloodstream, and the scientists were surprised to find that the yeast could get across the blood-brain barrier. That barrier can exclude many types of potentially harmful molecules and microbes.
"We thought that yeast would not enter the brain, but it does," Corry said. "In the brain, the yeast triggered the activity of microglia, a resident type of immune cell. The cells became very active eating and digesting the yeast. They also produced a number of molecules that mediated an inflammatory response leading to the capture of the yeasts inside a granule-type structure inside the brain. We called it fungus-induced glial granuloma, or FIGG."
Candida albicans is shown in the video above.
After testing the memory of the infected animals and non-infected controls, the team found that infected mice had problems with spatial memory. That dysfunction was reversed when the mice were cured of their infection, which took about ten days.
However, the microglia that were triggered by the fungus stayed active, with the FIGGs continuing to persist for at least another 21 days. When the FIGGs formed, the researchers were intrigued to see amyloid precursor proteins built up around the periphery, while amyloid beta molecules accumulated around yeast cells that sat in the center of FIGGs. These amyloid molecules are also found in a hallmark of Alzheimer's disease.
"These findings suggest that the role fungi play in human illness potentially goes well beyond allergic airway disease or sepsis," Corry said. "The results prompted us to consider the possibility that in some cases, fungi also could be involved in the development of chronic neurodegenerative disorders, such as Alzheimer's, Parkinson's and multiple sclerosis. We are currently exploring this possibility."
"For these reasons, if we better understand how our immune system deals with this kind of constant threat and what are the weaknesses in our immunological armor that occur with aging that allow fungal disease to take root, then we would likely [increase] the possibility of finding ways to fight back, " Corry said.
Corry is featured in the interview below discussing his career and research.
Sources: AAAS/Eurekalert! Via Baylor College of Medicine, Nature Communications