Fibromyalgia Linked to Gut Microbes
Genetic technologies advanced incredibly in recent years, allowing researchers to take stock of the microbial community living in the human gastrointestinal tract. Since then, the gut microbiome has been shown to have a close connection to our health and well-being. Some diseases with unclear causes have been linked to this microbial community, which can impact digestion and nutrient absorption, our mental health, and the function of the immune system, among other things. Now researchers have found an association between the gut microbiome and a chronic pain disorder - fibromyalgia.
For a time, people with fibromyalgia were told that their disorder was psychological, or a figment of their imagination. But this debilitating condition is now estimated to affect two to four percent of the population. There is no cure; treating the disorder is challenging and only applies to the symptoms - widespread pain and sensitivity.
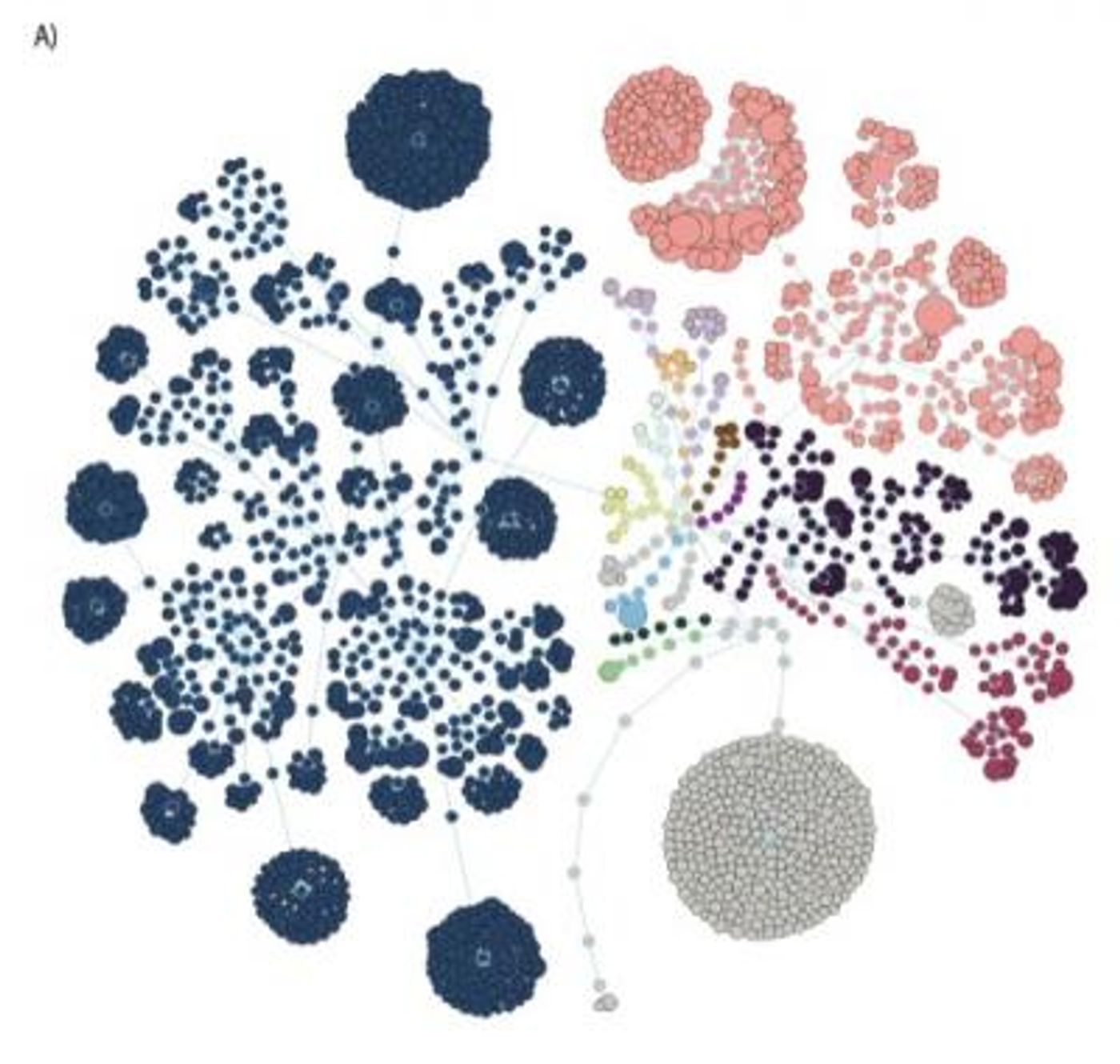
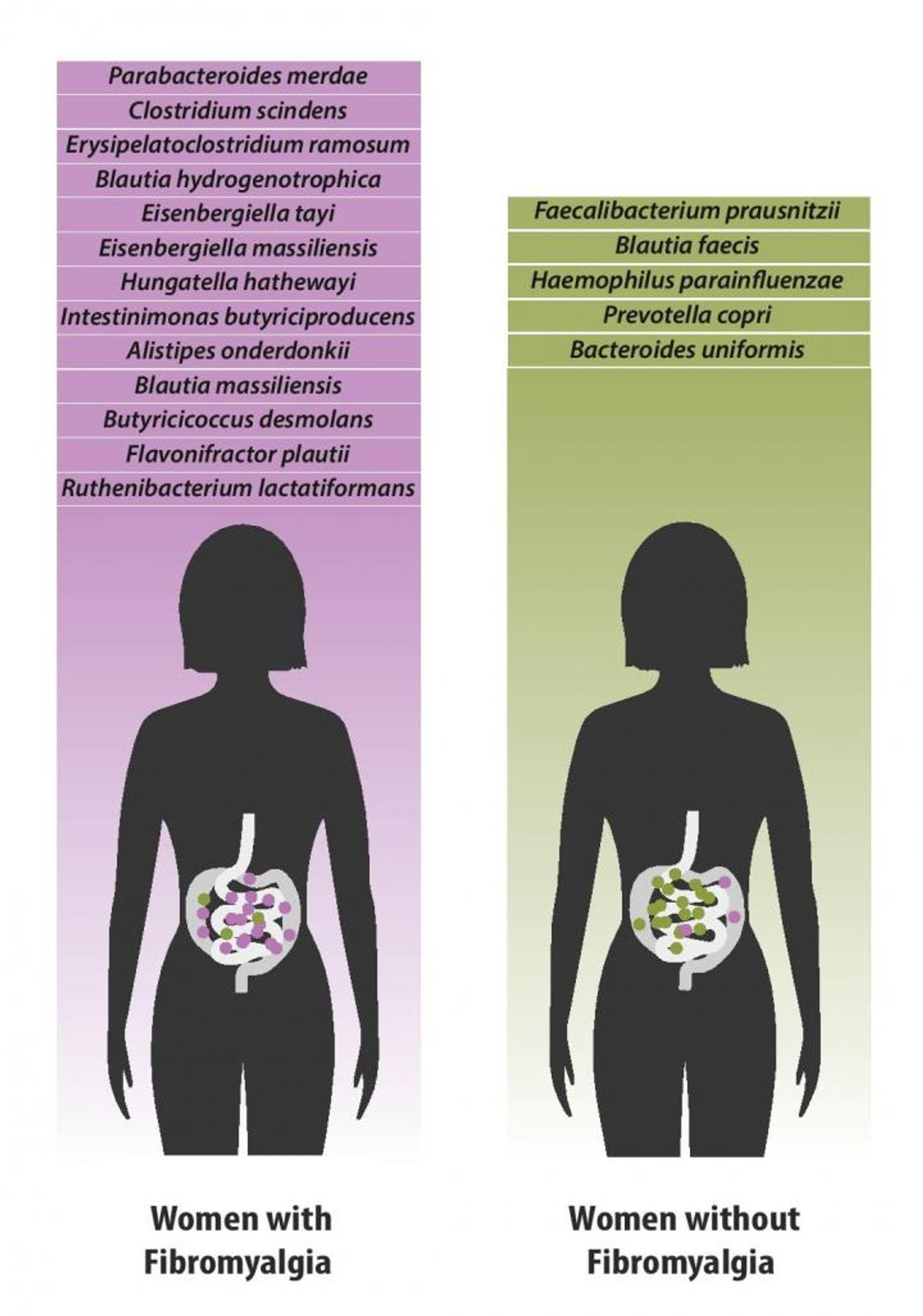
This new study, which has been published in Pain, assessed biological samples and questionnaires from 156 Canadian individuals, 77 of whom have fibromyalgia. The scientists identified differences in the microbial population in the guts of people with fibromyalgia. There were either more or less of around twenty types of bacteria in those suffering from the disease than the healthy people, as shown in the figure.
"We used a range of techniques, including artificial intelligence, to confirm that the changes we saw in the microbiomes of fibromyalgia patients were not caused by factors such as diet, medication, physical activity, age, and so on, which are known to affect the microbiome," noted the first author of the study Dr. Amir Minerbi of the Alan Edwards Pain Management Unit at the McGill University Health Centre (MUHC).
"We found that fibromyalgia and the symptoms of fibromyalgia - pain, fatigue and cognitive difficulties - contribute more than any of the other factors to the variations we see in the microbiomes of those with the disease," Minerbi added. "We also saw that the severity of a patient's symptoms was directly correlated with an increased presence or a more pronounced absence of certain bacteria - something which has never been reported before."
It’s too early to know whether the microbes are causing the disease or are markers of it, and the researchers want to investigate whether the changes in the gut microbiome are seen in people with other kinds of chronic pain. They also want to find out whether bacteria play a role in the development or progression of pain or fibromyalgia.
People can wait years for a conclusive diagnosis. This work may help open up new diagnostic avenues or treatment options.
"We sorted through large amounts of data, identifying 19 species that were either increased or decreased in individuals with fibromyalgia," said Emmanuel Gonzalez of McGill University. "By using machine learning, our computer was able to make a diagnosis of fibromyalgia, based only on the composition of the microbiome, with an accuracy of 87 percent. As we build on this first discovery with more research, we hope to improve upon this accuracy, potentially creating a step-change in diagnosis."
Fibromyalgia is outlined in the video above.
"People with fibromyalgia suffer not only from the symptoms of their disease but also from the difficulty of family, friends and medical teams to comprehend their symptoms," added senior study Yoram Shir, the Director of the Alan Edwards Pain Management Unit at the MUHC. "As pain physicians, we are frustrated by our inability to help, and this frustration is a good fuel for research. This is the first evidence, at least in humans, that the microbiome could have an effect on diffuse pain, and we really need new ways to look at chronic pain."
Sources: AAAS/Eurekalert! via McGill University Health Center, Pain