How Penicillin Blows Up Bacteria
Penicillin was discovered in 1928, when Alexander Fleming saw that mold had started to grow on a plate containing bacterial colonies, and the mold was preventing the bacteria from growing. But scientists are still learning about how it works. Scientists have finally revealed more about why pathogenic microbes burst when they encounter the drug. The findings, which can aid in the development of drugs that can destroy antibacterial resistant bacteria, were reported earlier this year in eLife.
“We’re finally getting mechanistic clues as to how penicillin and related drugs cause bacterial cells to explode,” said Harvard Medical School (HMS) microbiologist Thomas Bernhardt, a Howard Hughes Medical Institute Investigator (HHMI).
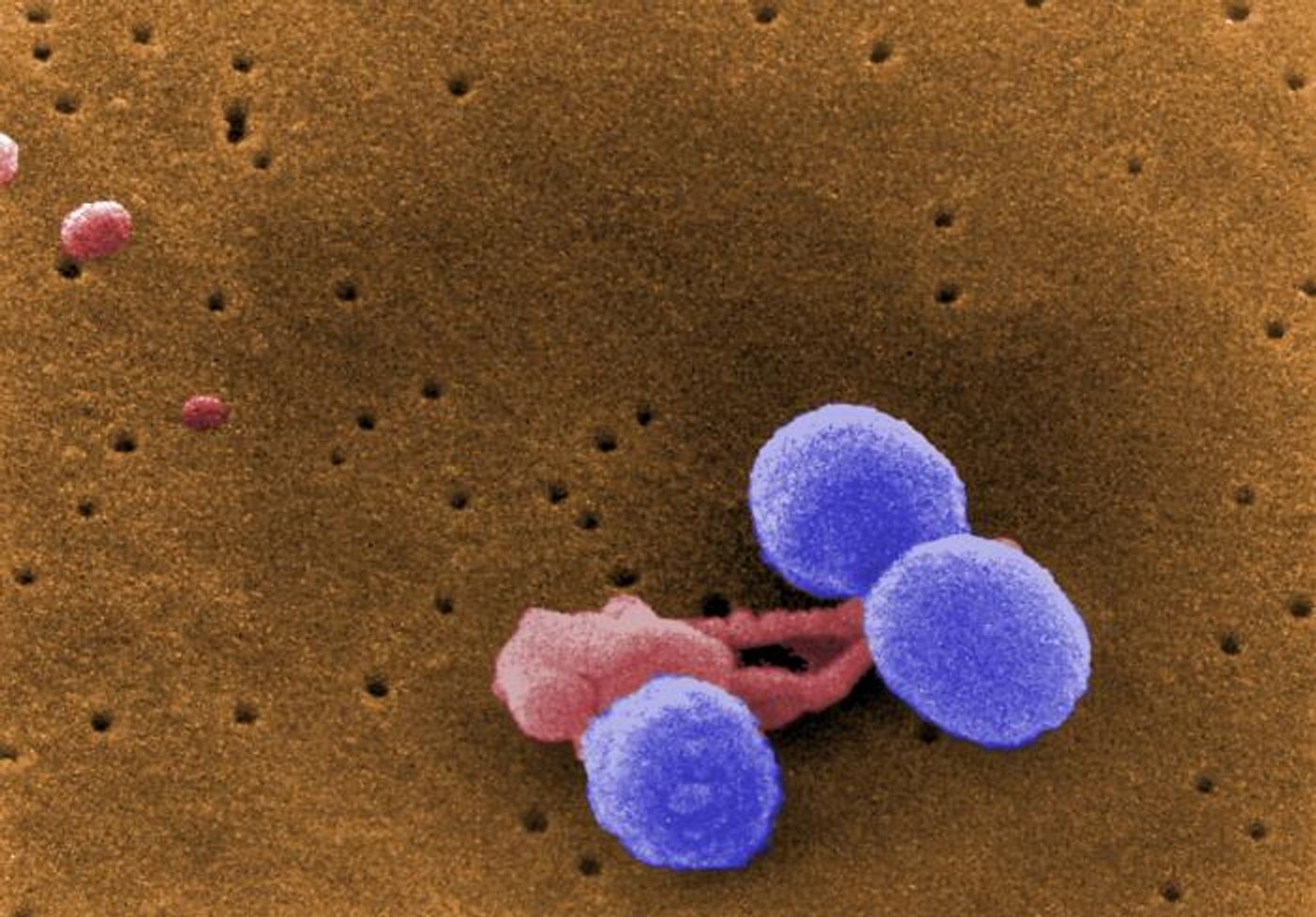
Like many other antibiotics, penicillin is a beta-lactam drug. Bacteria are beginning to resist the effects of these drugs, however, and antibiotic resistance is considered a growing threat to public health. Beta-lactams can be effective against many types of bacteria; they interfere with molecules that are crucial to the integrity of the microbial cell wall. When a bacterium is exposed to beta-lactams, the cell wall can break down and let in water, and eventually, the microbe explodes.
The microbial proteins that penicillin can attach to were discovered decades ago, and were named penicillin-binding proteins. These proteins play a critical role in the synthesis of the cell walls of bacteria. But some pathogens, like the one used in this research, Streptococcus pneumoniae, don’t burst open when their cell wall is under threat; another enzyme is required, called LytA.
LytA can break parts of the cell wall down like a sledgehammer. In the course of normal cell division, bacteria have to break their cell walls open. But if the enzyme causes too much breakage, the cells will explode, noted Bernhardt. He wanted to know more about how this activity is controlled.
A postdoctoral fellow at HMS, Josué Flores-Kim, found that another enzyme called TacL and several other molecules control where LytA is located, and thus, modulate its activity. TacL helps generate a kind of molecular chain that sits in the cell membrane, Flores-Kim explained. Another, similar molecule, resides in the cell wall. Together, they compete for LytA; the molecule in the membrane keeps LytA there, apart from the wall, Rudner said. When TacL is removed or it breaks down, which can happen after penicillin exposure, the molecule in the cell wall moves LytA there, where the enzyme causes major structural damage. Surrounding water can then flow in and cause the cell to explode.
“The finding that TacL is required to prevent bacteria from exploding suggests it would be a good antibiotic target,” Bernhardt said. “If we can block its activity with a drug, the cells will burst.”
Other bacteria also have similar control mechanisms, so this research may also apply to other bacterial pathogens.