Why the Brain Parasite You May Carry Isn't a Problem
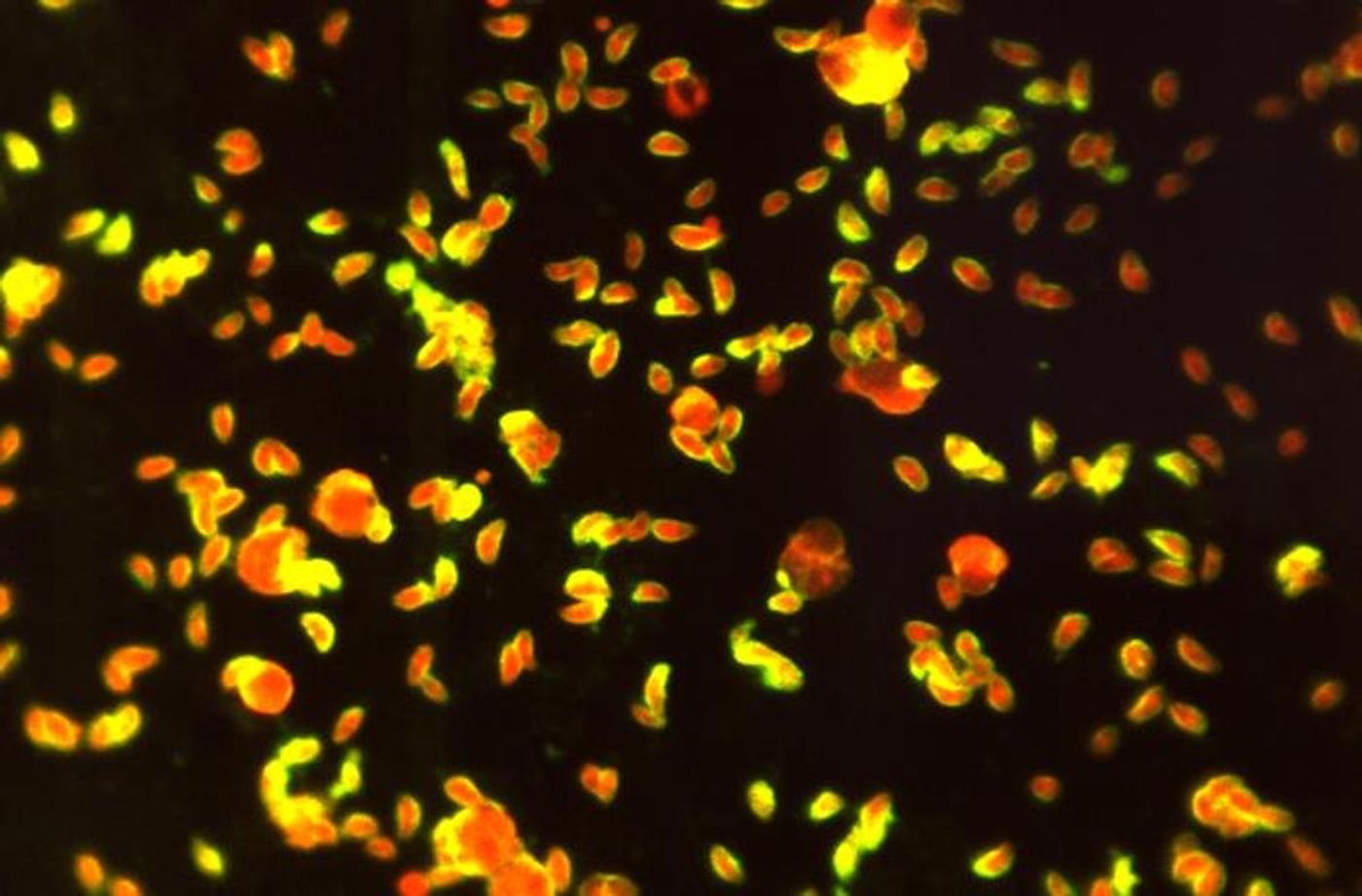
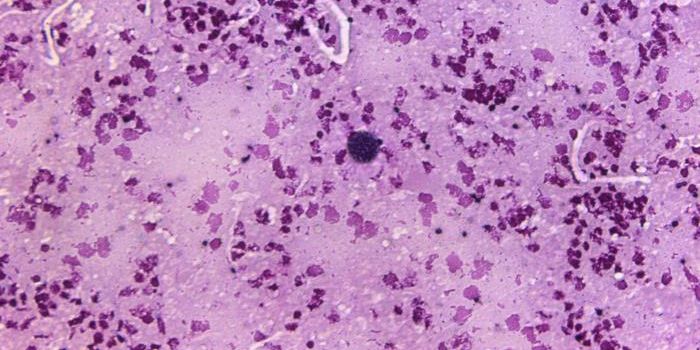
Toxoplasma gondii is a parasite transmitted by cats and contaminated meat, and it's thought that over 30 million Americans are infected with it. Scientists have now learned more about how the parasite can spread to the brain but doesn't cause symptoms in the vast majority of people. The findings, reported in Nature Communications, showed that special cells in the brain called microglia, which act as immune defenders and can clear debris, release a molecule called IL-1α in response to the infection, dying off in the process. This molecule brings more immune cells into the brain from the blood to control the parasite.
Microglia were once thought of as the only immune cells that reside in the brain. Recent studies have shown that various immune system processes beyond microglia can happen in the brain. This work now shows that when necessary, more immune cells can enter the brain, a finding that could have major implications for brain disorders involving the immune system like infections or injury, autoimmune disorders, or neurodegenerative diseases.
In the lab of Tajie Harris, Ph.D. at the University of Virginia's Department of Neuroscience, graduate student Samantha J. Batista has been investigating the role of microglia in the brain. With colleagues, she determined that during an infection, microglia die through inflammatory pathways, though closely related immune cells don't behave in this way.
"Microglia must die to save the brain from this infection," said Harris, the interim director of the Center for Brain Immunology and Glia (BIG). "Otherwise the IL-1α remains stuck inside the microglia and wouldn't alert the immune system that something is wrong."
The scientists found that the microglia will burst, signaling to immune cells called macrophages to come get the Toxoplasma gondii under control. This shows how most people can easily deal with these parasitic infections and show no symptoms, and why people who are immunocompromised can end up getting very sick.
"Understanding pathways like this could be beneficial for other diseases involving neuroinflammation," Batista said. "We can ask whether promoting this pathway is helpful in situations where you need more of an immune presence in the brain, such as infections or cancers, and also whether inhibiting this molecule could be helpful in diseases driven by too much neuroinflammation, like multiple sclerosis. Targeting one specific pathway like this one could have less off-target effects than targeting inflammation more broadly."
The researchers want to know more about how microglia are able to detect the presence of T. gondii in the brain, and how they identify tissue damage in the brain, a feature of many brain diseases.
"The immune system must enter the brain to fight dangerous infections," said Harris. "We now understand how microglia sound the alarm to protect the brain. We suspect that similar signals are missed or misinterpreted in Alzheimer's disease, opening up an exciting new research avenue in the lab."
Sources: AAAS/Eurekalert! via University of Virginia Health System, Nature Communications