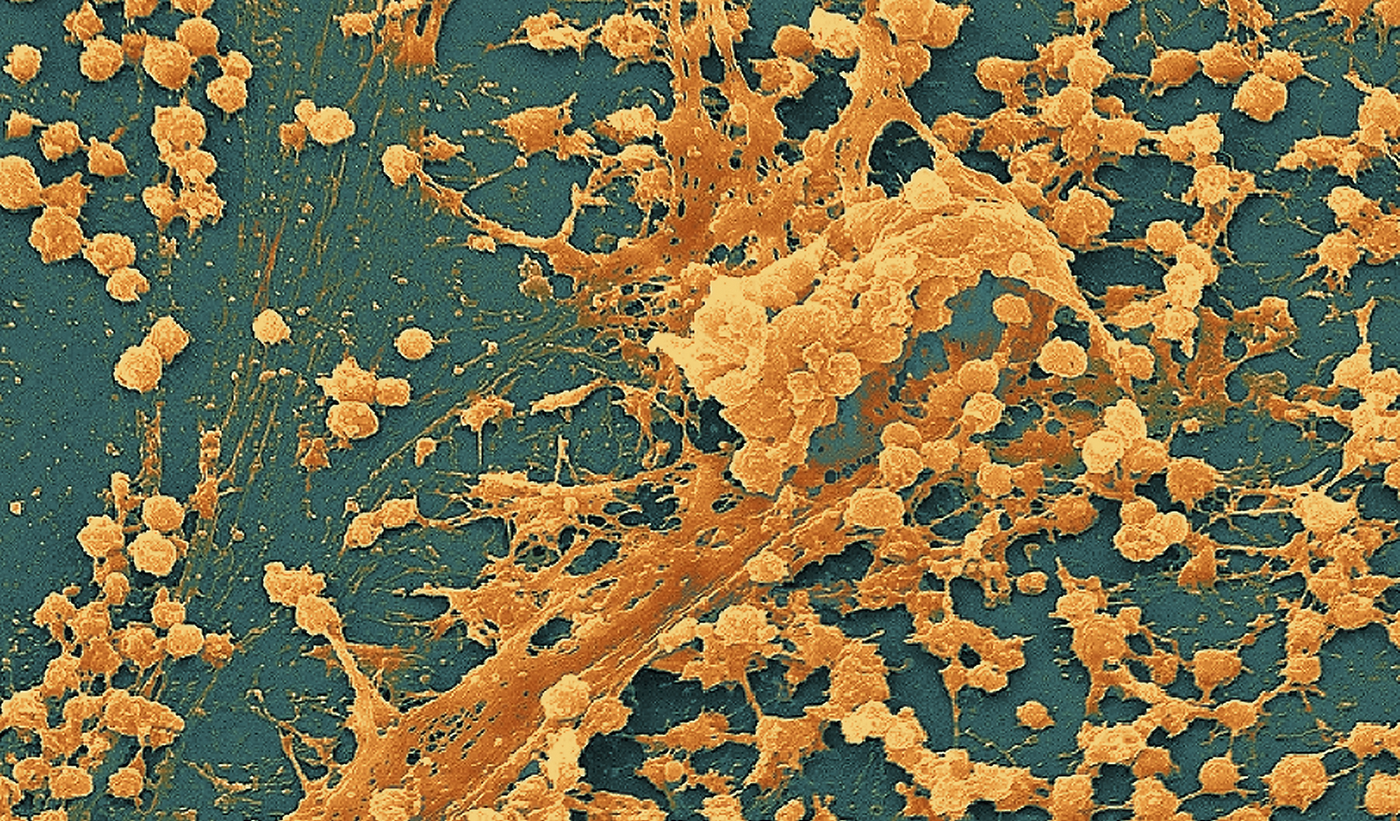
Staphylococcus aureus is notorious for forming
biofilms on indwelling medical devices (things like urinary and vascular catheters, orthopedic implants, and prosthetic heart valves). The biofilms, sticky aggregates of bacteria, polysaccharides, and protein, are notorious for shielding bacteria from antibiotics and immune cells.
Researchers at the University of Gothenburg in Sweden knew that
S. aureus uses a blood clotting factor called
fibrin to anchor its biofilms. The group reasoned that they could use a
plasminogen activator (PA) to break up the fibrin and prevent biofilm formation.
To test this idea, the researchers, let by study author Jakub Kwiecinski, coated polystyrene surfaces with PA, inoculated them with bacteria, and looked for biofilms. PA treatment delayed biofilm formation on polystyrene for up to 32 hours after bacteria were added. Since PA treatment prevented biofilm formation, the group wanted to know if the bacteria would be more susceptible to antibiotics. They found that a high dose of antibiotic (over 1,000 μg/ml) had little effect on bacteria in biofilms. However, bacteria on PA-treated surfaces were killed with much lower doses of antibiotic (4-128 μg/ml). Finally, they inoculated coverslips with bacteria and implanted them into mice subcutaneously. After 3 days, biofilms did not form on the PA-coated coverslips, and there were 20-fold fewer viable bacteria compared to controls.
According to Kwiecinski, “we hypothesized that if we forced the human body to start dissolving those clots, we could prevent the biofilm from developing … this deprives
S. aureus of a scaffold for biofilm formation and prevents infection”. The group hopes that coating medical devices with plasminogen activator could dramatically reduce hospital-acquired infections.
Sources:
Applied and Environmental Microbiology,
American Society for Microbiology, Wikipedia