Deadly Microbe Linked to Childhood Brain Disorder
Pediatric hydrocephalus - excessive fluid on the brain of a child - has been connected to a bacterial pathogen. Hydrocephalus is the most common reason why children must undergo neurosurgery. The most common cause of pediatric hydrocephalus is post-infectious hydrocephalus (PIH). It's thought that about half of all the new cases of pediatric hydrocephalus come after an infection. The problem is especially bad in low- and middle-income countries in sub-Saharan Africa.
When infants get a serious infection, it may lead to neonatal sepsis, which often comes before PIH. As an infant grows, it may take a few months for hydrocephalus to become apparent as cerebrospinal fluid accumulates. Without surgery, these infants will often die in early childhood.
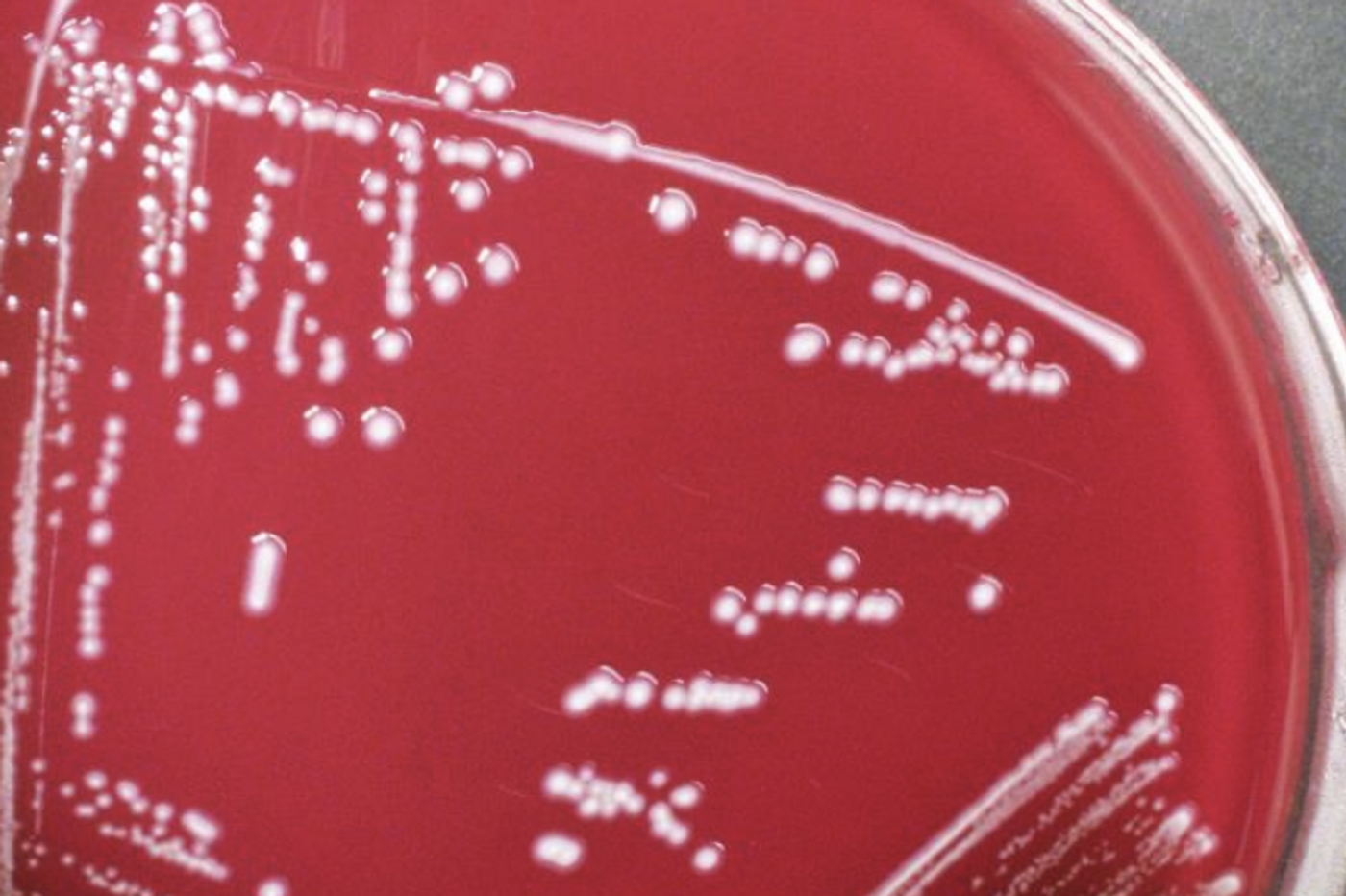
In new work reported in Science Translational Medicine, the co-first author of the study, Brent L. Williams, Ph.D., assistant professor of epidemiology at the Center for Infection and Immunity (CII) at Columbia University Mailman School of Public Health analyzed samples of cerebrospinal fluid (CSF) that clinicians in Uganda had obtained consecutively from one hundred PIH patients and infants with non-post-infectious hydrocephalus (NPIH). The samples were checked for bacterial and fungal microbes.
Paenibacillus bacteria were found in CSF that was obtained from patients with PIH, but not in controls. At Pennsylvania State University, a Paenibacillus strain was isolated and characterized by the senior study author Steven Schiff, M.D., and colleagues. The amount of Paenibacillus was connected to brain imaging scores used to measure hydrocephalus as well as the levels of immune cells, which can indicate the severity of an infection.
"This discovery has the potential to reduce morbidity and mortality of this central nervous system disease in millions of children in sub-Saharan Africa by shifting treatment from surgery to antibiotics and vaccines," noted the co-senior author W. Ian Lipkin, MD, John Snow Professor and CII Director.
"Now that we have identified a pathogen that may be responsible for some cases of post-infectious hydrocephalus, we can develop new, more sensitive tests to quickly detect an infection, assess its severity, identify the source of such infections, and hopefully provide targeted treatments to prevent the development of hydrocephalus" added Williams.
Sources: AAAS/Eurekalert! via Columbia University, Science Translational Medicine