How Do mRNA Vaccines Work?
Scientists working today are usually a part of a team, and many advancements and discoveries that are now made don't trace neatly back to a single person. The vaccines that have been developed in record time for COVID-19 are examples of that; researchers working together, building on previous efforts, have engineered these desperately needed medicines.
The Pfizer and Moderna vaccines that the FDA has approved for use are both mRNA (messenger RNA) vaccines.
Since our immune system has a memory, it can (usually) fight a pathogen more effectively when it encounters that pathogen for a second time. So vaccines are used to 'teach' your immune system about an infection, giving it the first exposure, without making the body sick. Many traditional vaccines use inactivated or weakened forms of pathogens to trigger an immune response and create the immunological memory of the infection. But mRNA vaccines work in a different way.
Animal cells keep the genome, or DNA in the nucleus. Cellular machines can transcribe active genes from the DNA into another molecule called mRNA. The mRNA is then used in another part of the cell to generate proteins that are required for carrying out biological functions.
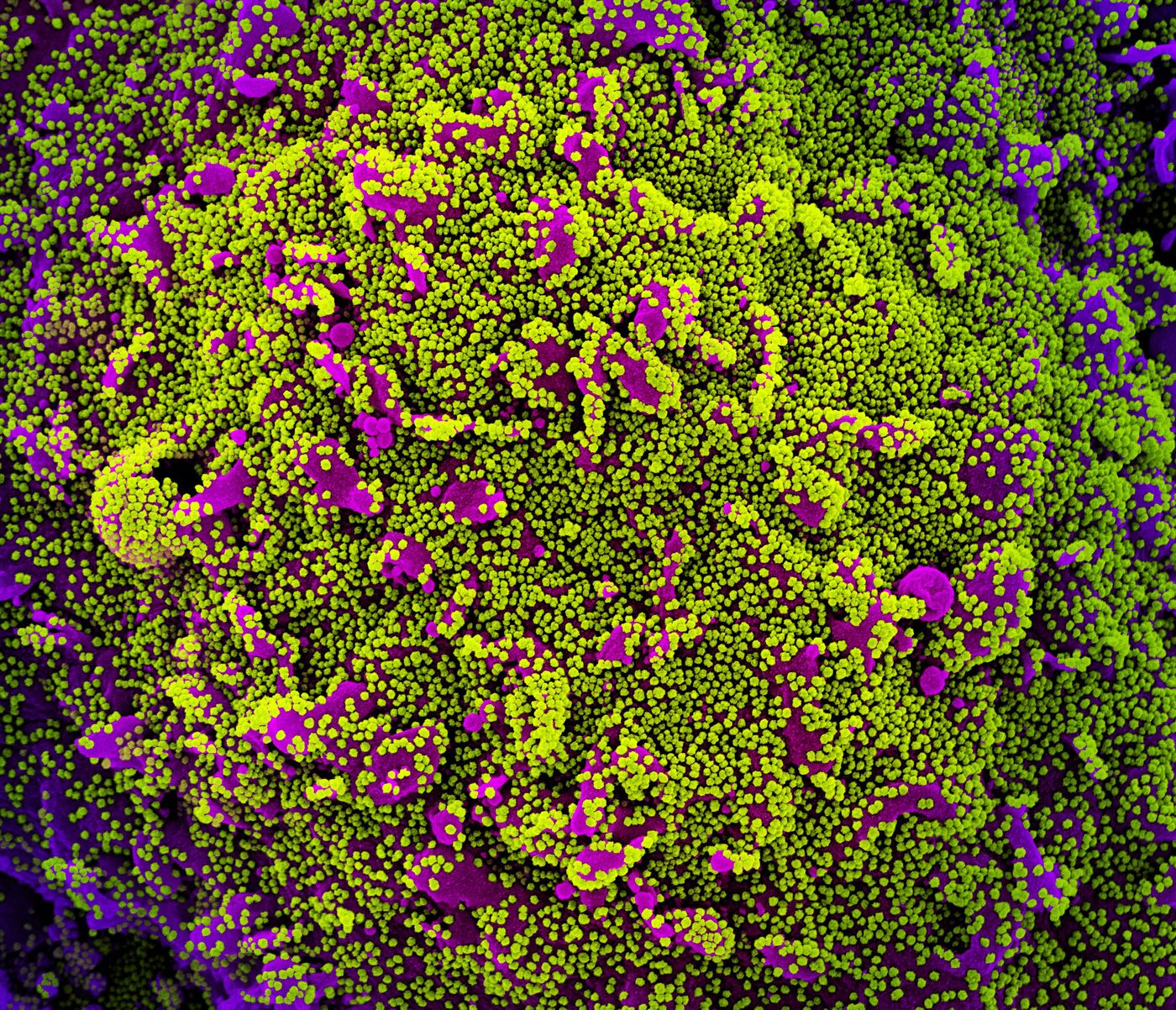
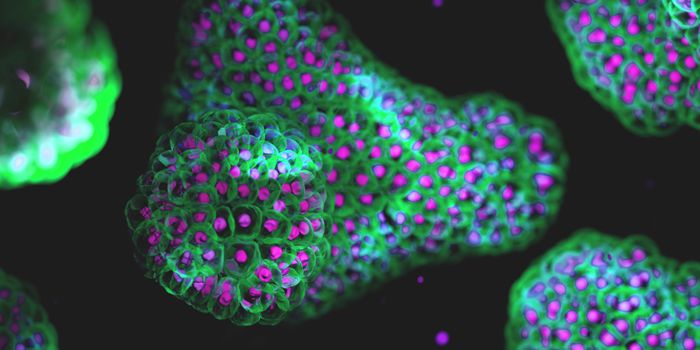
Viruses are different. Some, like the SARS-CoV-2 virus that causes COVID-19, are RNA viruses; their genomes are made of RNA. When they infect cells, their RNA genome is dumped into a host animal cell. These RNA molecules are then transcribed by the host cell's machinery into viral proteins that take the host cell over and spread more infectious particles to other cells.
In the case of mRNA vaccines, the body is exposed to a piece of viral mRNA that encodes for a harmless viral protein - the mRNA that's injected as the vaccine is contained inside of lipid nanoparticles that help it get into cells. But once that viral protein is made by cells, the immune system will mount a response against it. Because the piece of mRNA encodes for only one portion of a viral protein that's ineffective at causing an infection on its own or creating more viral particles, it cannot cause an illness. But it's sufficient to train the immune system. It takes a few days after the vaccine is administered for the body to generate viral proteins from the mRNA and then respond. Once that happens, however, a vaccinated person's immune system will have been trained to attack the COVID-19 virus in the case of infection.
Cells break down mRNA quickly once it's used, so these molecules will not linger in the body. They also do not enter the nucleus so they will not impact a person's DNA.
Scientist Katalin Karikó has been studying mRNA vaccines for years, and now works at BioNTech, a German research company. She spent years getting grant rejections for her ideas about mRNA vaccines and left the University of Pennsylvania after being demoted. But now she may be on track to win the Nobel Prize, and her efforts are helping to end a global pandemic.
Karikó and her co-authors from a 2014 review on mRNA vaccines that was published in Nature Review Drug Discovery, Ugur Sahin and Özlem Türeci, are the leaders of the work behind the Pfizer vaccine.
The authors noted in that review that this concept originated with a team including physician-scientist Jon A. Wolff, reporting in Science in 1990. Wolff and co-authors showed that when mRNA was injected into mouse skeletal muscle, it would be transcribed into protein. Later efforts showed that this was a feasible approach for vaccination.
Sources: CDC, NPR, Science, Nature Reviews Drug Discovery