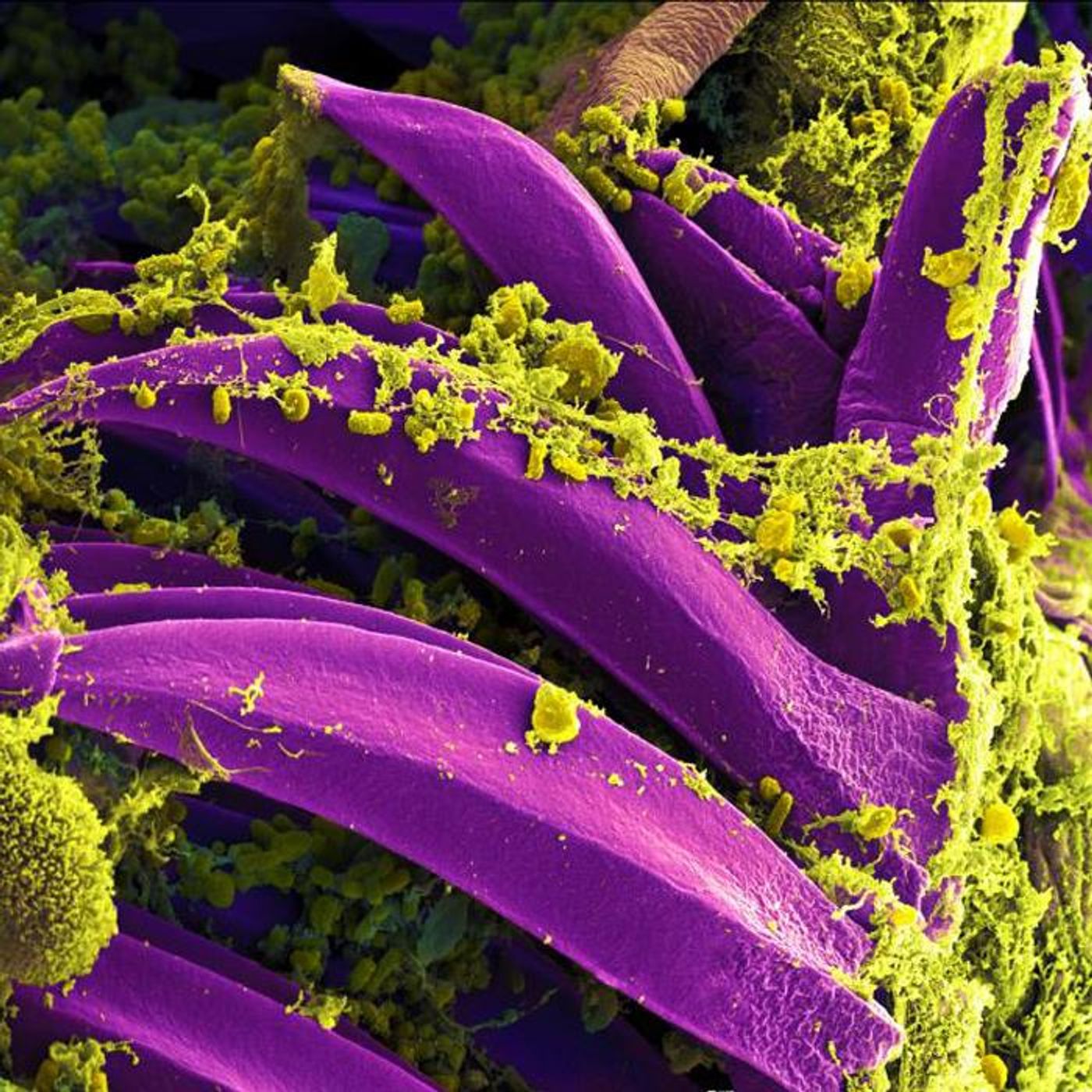
The Bubonic Plague May Have Had a Lasting Impact on Humans
The bubonic plague is caused by a bacterium, Yersinia pestis, which is transmitted to humans by fleas. The bacterium can also cause two other types of plague disease. There were several major bubonic plague pandemics that originated in East Asia and spread to Europe and beyond; the first around 540, the next in the 1330s, and another in the 1900s. The second pandemic was so serious, it's thought to have killed a third of the European population.
Researchers have now examined samples from 36 bubonic plague victims buried in a mass grave in Germany in the town of Ellwangen. The work has suggested that the plague triggered evolutionary adaptations in some people, so future generations were better at fighting off this pathogen. The findings have been reported in Molecular Biology and Evolution.
In this study, DNA samples from bubonic plague victims were compared to DNA samples from 50 individuals that are current residents of Ellwangen - the same town of the victims, where bubonic plague outbreaks happened in the 16th and 17th centuries. The researchers examined the frequency of small changes in the sequences of immune genes.
"We found that innate immune markers increased in frequency in modern people from the town compared to plague victims," said co-senior study author Paul Norman, Ph.D., an associate professor in the Division of Personalized Medicine at the University of Colorado School of Medicine. "This suggests these markers might have evolved to resist the plague."
The researchers found evidence that suggested that the frequency of some gene variants began to change, in genes for two innate pattern-recognition receptors and four Human Leukocyte Antigen molecules. These genes are involved in the immune system's response to infection.
"We propose that these frequency changes could have resulted from Y. pestis plague exposure during the 16th century," Norman said.
The plague circulated in Europe for thousands of years, so certain immunity gene variants may have been selected in the population long ago and during more recent epidemics. Even though the plague tended to kill people who were infected, not everyone died. So some people may have been protected from the disease caused by the pathogen (while others were more vulnerable to severe cases). It shows how people that were naturally better at fighting the illness were more likely to pass those gene variants down to future generations, who would then be less susceptible.
"I think this study shows that we can focus on these same families of genes in looking at immunity in modern pandemics," Norman added. "We know these genes were heavily involved in driving resistance to infections."
This research has also shown that even when pandemics are devastating, people still survive. "It sheds light on our own evolution," Norman said. "There will always be people who have some resistance. They just don't get sick and die and the human population bounces back."
However, he noted that we can't simply rely on natural immunity to get us through disease outbreaks. "I wouldn't want to discourage anyone from taking a vaccine for the current pandemic," Norman noted. "It's a much safer bet than counting on your genes to save you."
Sources: AAAS/Eurekalert! via University of Colorado Anschutz Medical Campus, Molecular Biology and Evolution