What Causes False Positives? Understanding Blood Culture Contamination
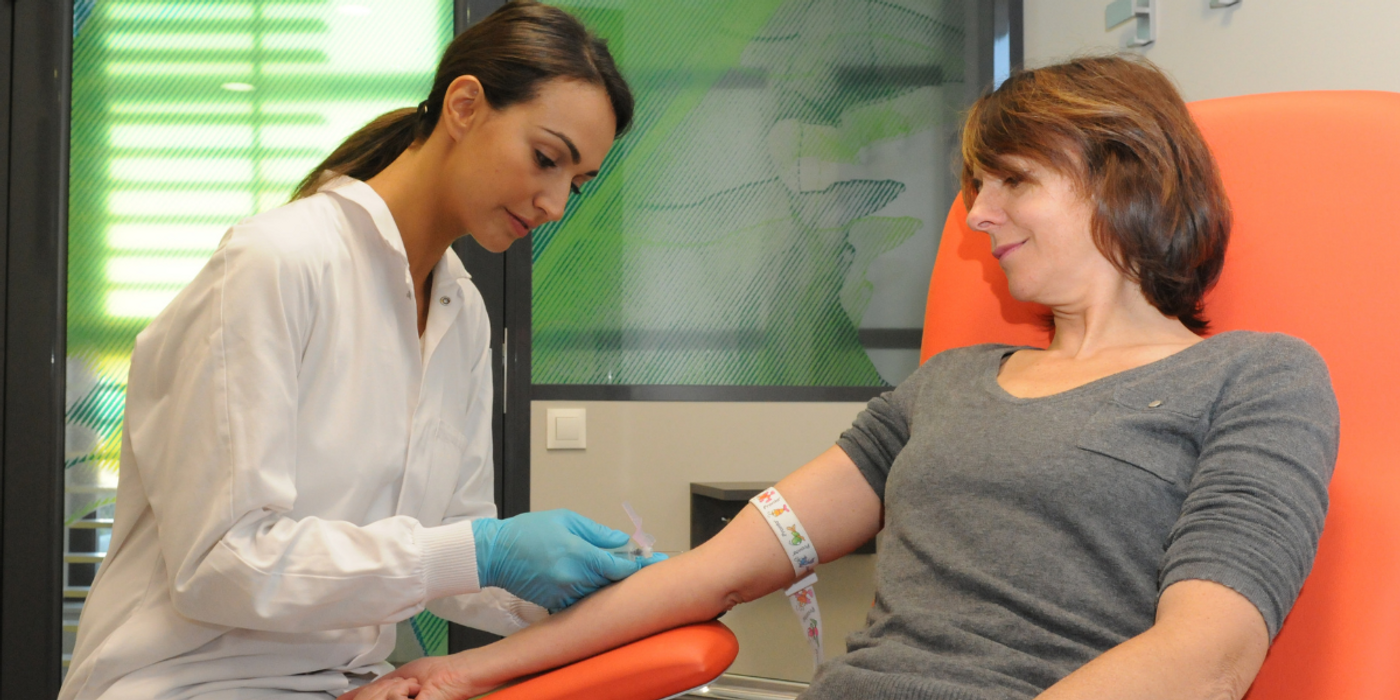
Blood culture is the most widely used diagnostic tool for the detection of bacteremia and fungemia. It is the most important way to diagnose the etiology of bloodstream infections and has major implications for the treatment of those patients. However, blood cultures are frequently contaminated, which can lead to a “false positive” result. This can lead to substantial costs for the laboratory as well as negative outcomes among patients for whom blood cultures have been drawn.1
Blood culture contamination is defined as the presence of microorganisms in the blood culture bottle that entered during sampling but was not actually circulating in the patient’s bloodstream. Healthcare institutions in the United States are held to a performance standard of less than 3% contamination rates for blood culture,2 but numerous studies have shown contamination rates to be far higher than the 3% standard, with some studies showing as high as, “one-half of all positive blood cultures were judged by infectious disease physicians to represent contamination.”1 There are many possible sources of blood culture contamination, with some frequent sources including:1
- Poor blood culture collection technique
- Insufficient disinfection of the skin
- Collection of blood from an indwelling vascular catheter
The impact of blood culture contamination is felt in the microbiology laboratory and beyond. Contamination can have negative impacts on the lab, hospital system, and patients, with far-ranging consequences such as:1
- Increased staff workload, when many microbiology laboratories struggle with staffing shortages
- Unnecessary and expensive additional laboratory testing – up to 80% increase in microbiology charges
- Unnecessary antimicrobial therapy, which is associated with antimicrobial resistance
- Up to five days longer length of hospital stay for patients
Strategies to Reduce Contamination
Thankfully, there are proven strategies to help reduce blood culture contamination. A study from the British Journal of Biomedical Science found that “the introduction of blood culture packs and staff training has reduced contamination rate significantly from 43% to 25% of the total number positives, equating to an overall reduction of 42%.”3 Utilizing pre-assembled blood culture collection kits and staff education are both practical and effective tools for reducing blood culture contamination.
Acquiring the right blood culture collection kits may seem an intimidating task, which is why having an experienced blood culture partner is an essential component of reducing contamination. The study cited previously leveraged BACT/ALERT WORKSAFE™ blood culture collection kits from bioMérieux, which include blood culture bottles as well as tools for optimal blood culture collection, such as antiseptic swabs, alcohol prep pads, and blood culture bottle adapters. These convenient kits come in variants for adult and pediatric blood cultures and help simplify the blood culture collection process.
With high levels of staff turnover and staffing shortages impacting healthcare systems as a result of COVID-19, keeping both employees up to date on blood culture education is a challenge, but it is not one that needs to be borne alone. bioMérieux cited earlier, has over 300 dedicated customer support personnel, with both field and remote teams available to provide blood culture collection training programs for Nursing, Phlebotomy, and Laboratory staff, in addition to an open access online library of 25+ videos on blood culture education.
With a positive blood culture being a key diagnostic tool for managing patients with signs of bloodstream infections, healthcare systems, and diagnostic equipment manufacturers can work together to reduce the serious danger to patient well-being that a “false positive” from blood culture contamination presents.
To learn more about bioMérieux’s blood culture solutions, visit their website or contact CustomerDelight@biomerieux.com.
References
- Doern GV, Carroll KC, Diekema DJ, et al. Practical Guidance for Clinical Microbiology Laboratories: A Comprehensive Update on the Problem of Blood Culture Contamination and a Discussion of Methods for Addressing the Problem. Clinical Microbiology Reviews. 2019;33(1). doi:10.1128/cmr.00009-19
- Wilson ML. Principles and Procedures for Blood Cultures: Approved Guideline. Wayne, PA: Clinical and Laboratory Standards Institute; 2007.
- Bamber AI, Cunniffe JG, Nayar D, Gangul R, Falconer E. Effectiveness of introducing blood culture collection packs to reduce contamination rates. British Journal of Biomedical Science. 2009;66(1):6-9. doi:10.1080/09674845.2009.11730236