'Living Medicines' to Destroy Dangerous Biofilms
Bacteria that grow in colonies can be extremely difficult to eliminate; the bacteria in these groups often become resistant to drugs or antimicrobials. Known as biofilms, bacterial communities that grow on surfaces can be found in many places, including medical devices. Biofilms are far stronger than free-floating microbes on their own, and an estimated 80 percent of chronic infections are linked to biofilms. Scientists have now devised a new approach to attack these dangerous bugs, with a 'living medicine' that's made up of other microbes.
The medicine was tested on catheters that were infected with biofilms in three settings: in the lab, in tissue taken from an organism, and in a mouse model. When the mouse model of infection was treated with the 'living medicine,' 82 percent of infections were eliminated. The findings have been reported in Molecular Systems Biology.
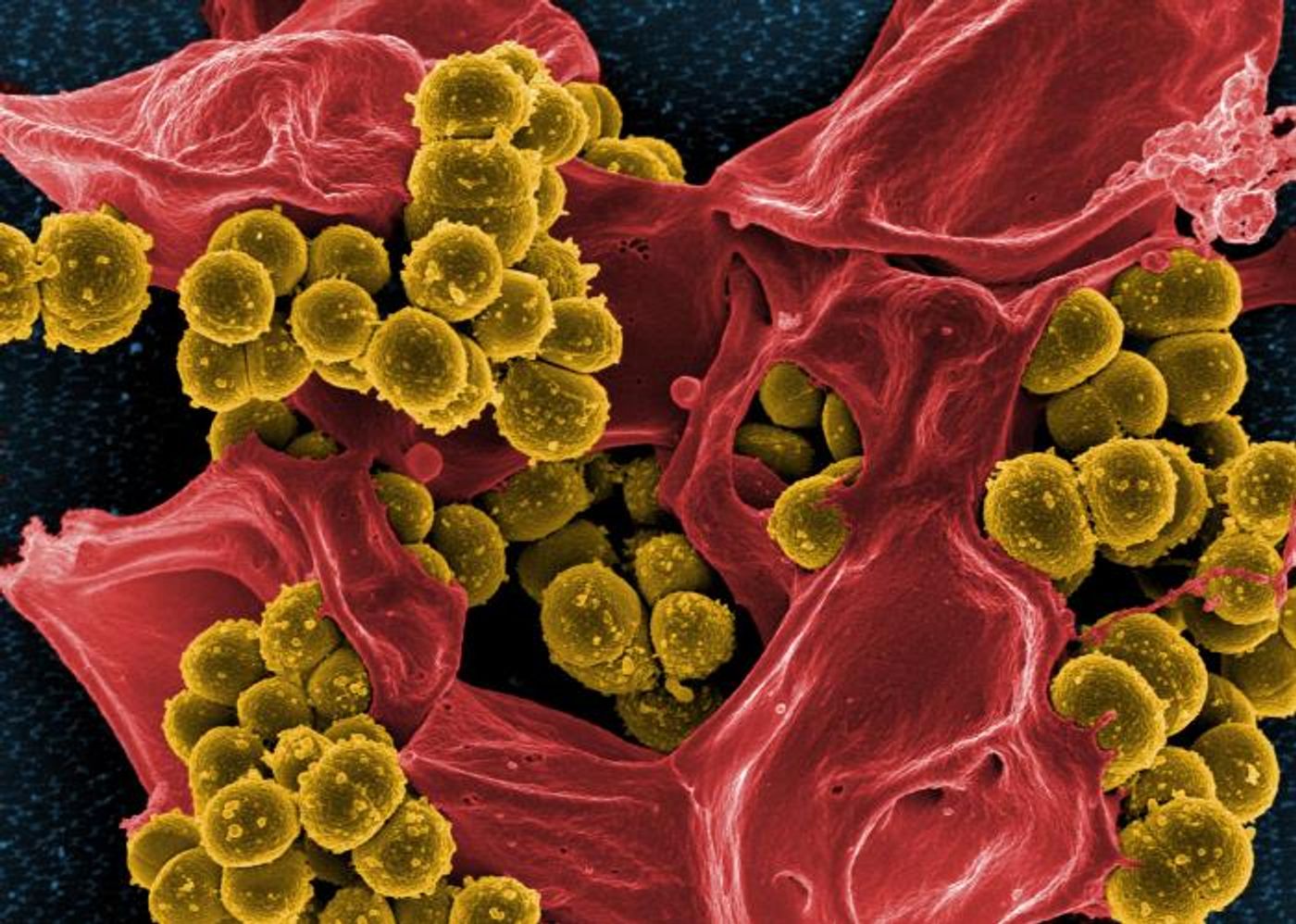
Many biofilms are caused by Staphylococcus aureus, and standard antibiotics cannot remove them. So if a patient has a medical implant infected by an S. aureus biofilm, enzymes or antibodies are sometimes useful, but these treatments can harm normal cells and cause side effects because they are not designed to specifically target the infection. Patients may have to undergo surgery to remove the infection.
Microbes are already engaged in a battle with one another for resources and survival. The researchers thought that the molecules produced by living microorganisms could be another way to treat biofilms. Bacterial genomes are also small and easily manipulated. In this study, the scientists selected a bacterium called Mycoplasma pneumoniae, which doesn't have a cell wall. As such, it can evade the immune system and can easily release therapeutic molecules. This microbe also tends to hold onto its DNA, which doesn't tend to mutate naturally, and not pass it to other microbes.
The researchers began by eliminating the pathogenicity of this bacterium so it would not make people sick. They also engineered the bacterial genome to easily release two enzymes that it was modified to produce. Each of those enzymes can dissolve biofilms.
The scientists are hopeful that these bacteria can be used first to remove biofilms from breathing tubes. Safety testing is complete. The next issue to address is manufacturing, "and we expect to start clinical trials in 2023," said co-corresponding study author María Lluch, Chief Science Officer of Pulmobiotics S.L.
This technique might be applicable to other health problems."Bacteria are ideal vehicles for 'living medicine' because they can carry any given therapeutic protein to treat the source of a disease," suggested study co-author Luis Serrano, ICREA Research Professor and Director of the Centre for Genomic Regulation. "One of the great benefits of the technology is that once they reach their destination, bacterial vectors offer continuous and localized production of the therapeutic molecule."
Sources: Centre for Genomic Regulation, Molecular Systems Biology