Explaining the Alarming Rise of Superbugs During the Pandemic
The US Centers for Disease Control and Prevention (CDC) recently reported that during the pandemic, there was a significant increase in the number of antibiotic-resistant infections, caused by so-called superbugs. After the initial peaks of the pandemic, the CDC found that antibiotic-resistant bacterial infections that started while a person was hospitalized increased 15 percent in 2020 compared to 2019.
In the first year of the pandemic, antibiotic-resistant infections typically linked to a hospital or healthcare clinic caused the deaths of over 29,400 people; about 40 percent of these individuals were infected during their hospital stay.
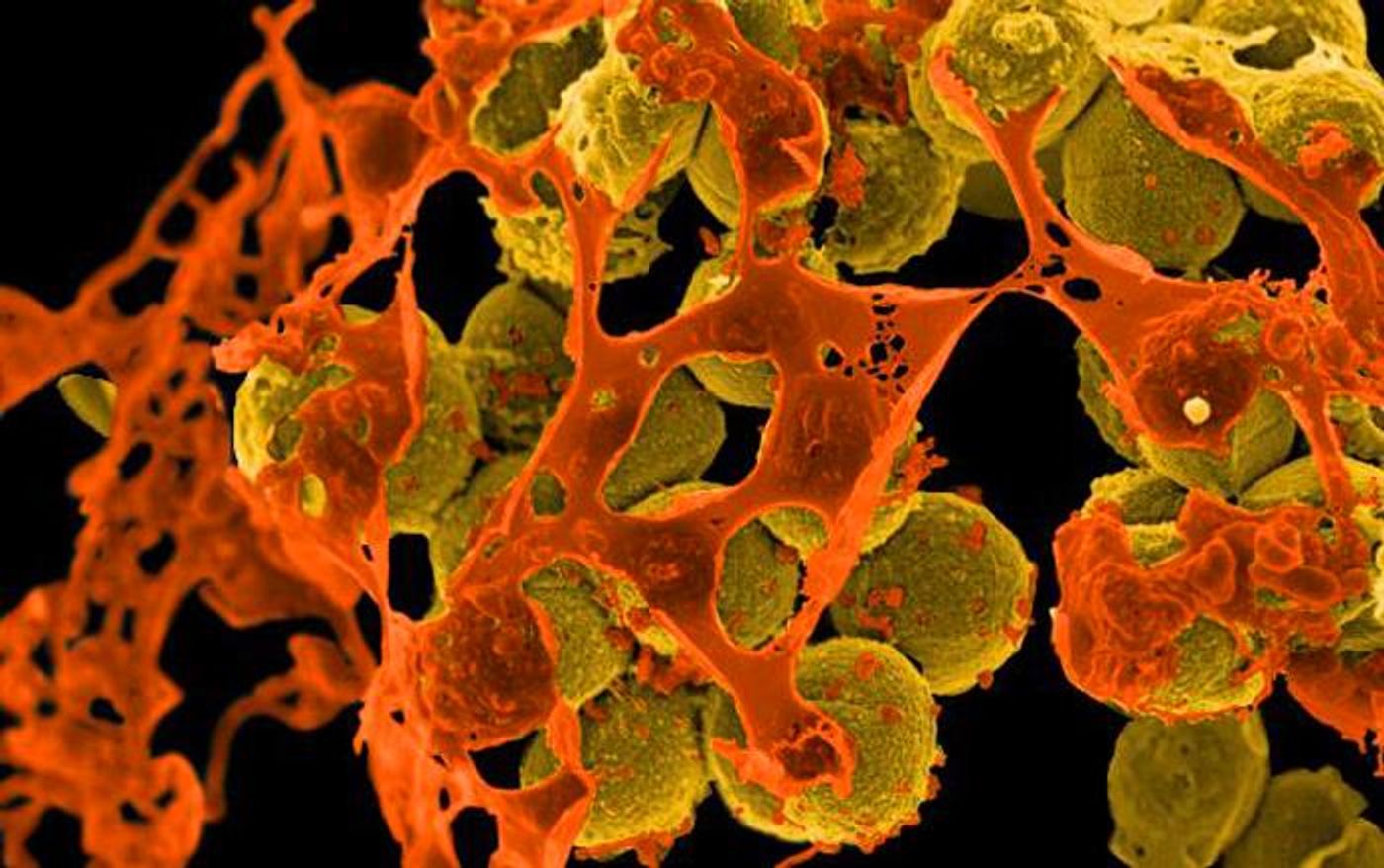
For example, there was a 32 percent increase in cases of multidrug-resistant Pseudomonas aeruginosa, and a 13 percent increase in methicillin-resistant Staphylococcus aureus (MRSA) infections.
The pandemic also wreaked havoc with the healthcare system, and the CDC acknowledged that these numbers may also be significantly undercounted.
This unfortunately reverses years of progress; between 2012 and 2018, deaths from antibiotic resistant infections dropped 18 percent overall and about 30 percent in hospitals.
Antibiotics are for battling bacteria, and they don't do anything for viruses, or fungi. So why did so many more people get antibiotic resistant infections? At the beginning of the pandemic, people had no idea how to treat it. In some cases, people were actually also getting bacterial infections once their immune systems had been weakened by the pandemic virus, and hospitals are, unfortunately, places where dangerous bacteria can cause infection.
There was a surge in antibiotic use for many reasons. It's estimated that 80 percent of Americans who got COVID-19 were given antibiotics. While some people needed those antibiotics, it is also likely that many of them were taken or prescribed unnecessarily. Research has indicated that when bacteria are exposed to antibiotics, they can evolve resistance, and then quickly share that resistance (by sharing a gene that makes that resistance possible).
The CDC and experts have stressed that we must return to best practices when it comes to antibiotic prescriptions and use. People should not take them unnecessarily, should not share them, and should take their entire prescription to completion, for example.
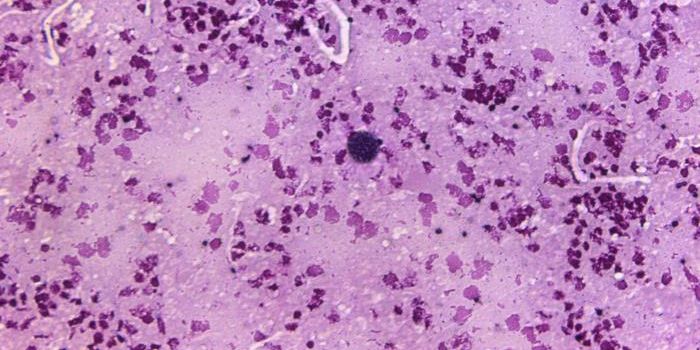
There was also an increase in resistant antifungals. Infections of Candida auris, for example, increased by an estimated 60 percent.
One pathogen improved. There were not as many Clostridioides difficile infections, potentially because people were more likely to go to the doctor if they felt sick, suggested the CDC.
This reversal comes at an unfortunate time when many old, reliable antibiotics are beginning to fail. The World Health Organization has warned that antibiotic resistant bacterial present a serious threat to human health, and notes that continuing to practice good hygiene, including proper hand washing, can help shield people from infection.
Sources: CDC, University of Colorado Boulder