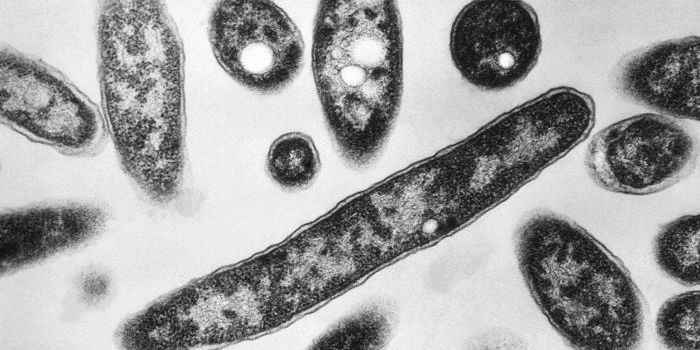
Clostridium difficile loves to infect the gut, and these infections (CDIs) can be nasty and difficult to treat. These spore-forming bacteria are often resistant to antibiotics and grow within a protective pseudomembrane in the gut where they cause diarrhea and colitis.
University of Leicester researchers recently reported on the successful use of a bacteriophage cocktail to treat CDI. This technique, often called “phage therapy”, uses bacteriophages to infect and kill pathogenic bacteria without harming the human host.
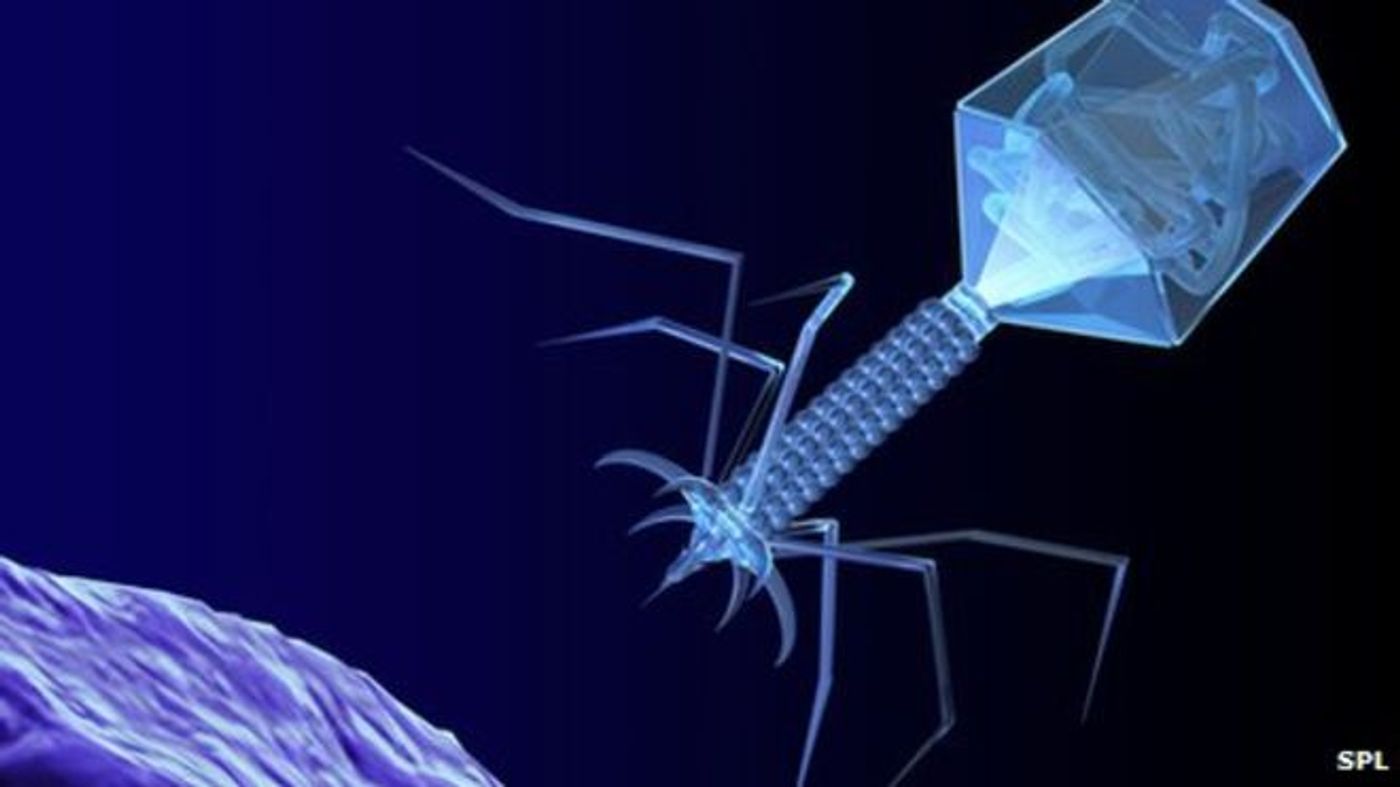 (Side note.) The idea of phage therapy
(Side note.) The idea of phage therapy has been around for quite some time. Bacteriophages were first described in the early 1900s, and the
Eliava Institute opened in Georgia (the country) in 1923 to research phage therapy. In fact, phage therapy is widely used in a number of European countries, but it has not caught on in the US.
(Back to your regularly scheduled programming.) The University of Leicester group tested various phages for their ability to kill (lyse) C. difficile in vitro. The phages lysed 86% of the clinical C. difficile strains tested. Specifically, the phages were effective against 12 of the 13 most common strains found in the UK.
Then they tested their phage cocktails - mixtures of phages in various combinations - in a hamster model of CDI. They found that certain cocktails reduced the bacterial load in the intestinal lumen by 4 logs and in intestinal tissues by 2 logs.
This is great, except that most of the hamsters still had relatively large amounts of the bacteria in their guts even after phage treatment. The point is, yes, the phage cocktails definitely reduced the overall bacterial burden, but they did not “cure” the animals of the infection.
Essentially, phage therapy bought the animals a bit more time. The animals were sacrificed once they reached a predetermined experimental endpoint (once their body temperature dropped to a certain point, for example). For untreated animals, this was after about 60 hours. However, animals treated with the phage cocktail took about twice as long to reach the same endpoint.
Phage therapy isn’t a cure-all (at least not for CDI). But, it could put a chink in C. difficile’s armor, helping clinicians combat these potentially deadly infections. According to M. Scott Salka, CEO of AmpliPhi Biociences (the company that funded this study), “the prevalence of
C. difficile, the high costs of infection control, and the challenge of finding alternative treatments all contribute to the significant clinical and financial burden that CDI imposes on healthcare systems. The positive outcomes of these studies validate phage-based therapy as a promising approach that has the potential to address the growing challenge of CDI.”
Sources: Antimicrobial Agents and Chemotherapy, MedicalXpress, Wikipedia