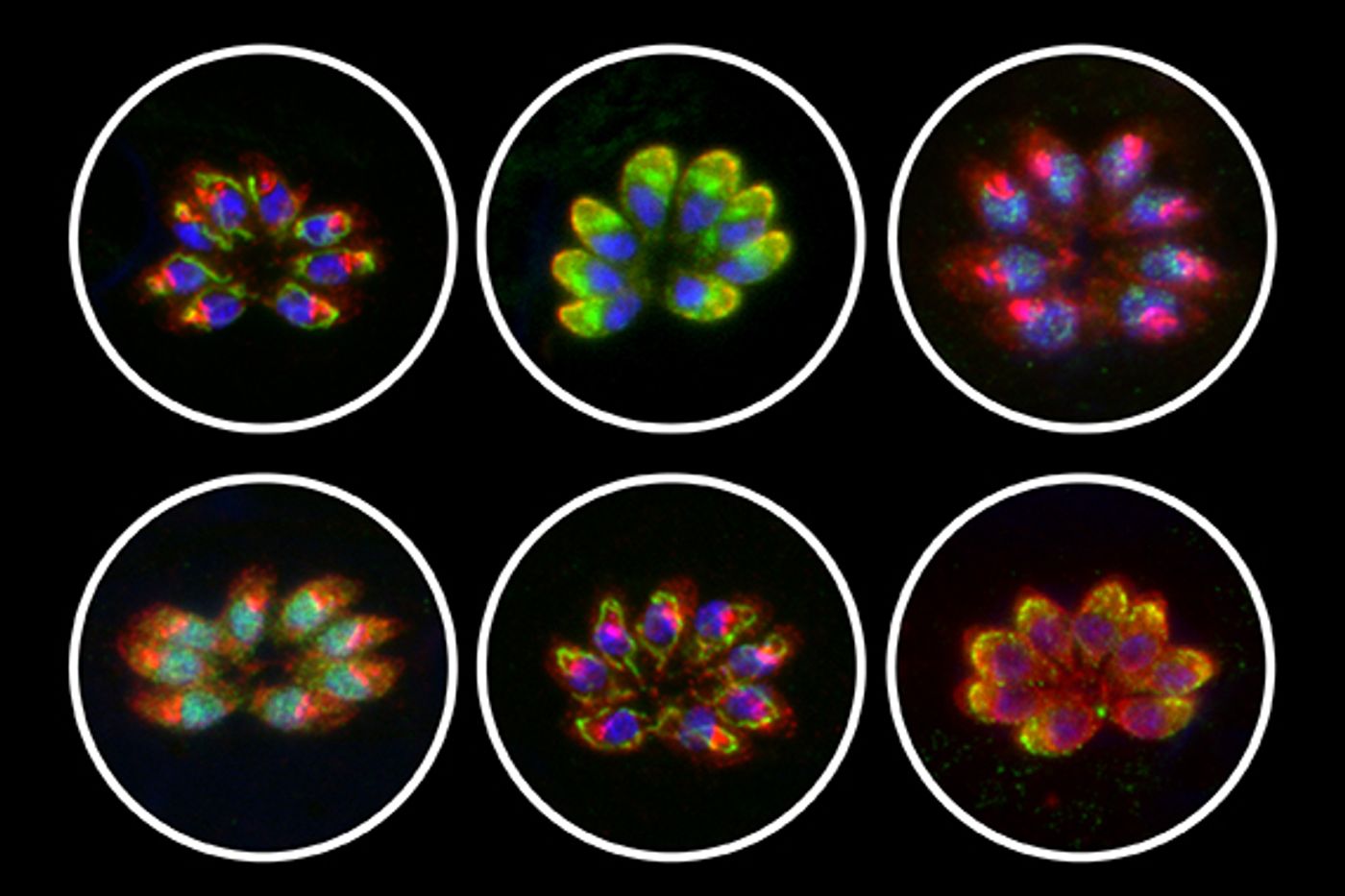
After performing the first genome wide screen of Apicomplexa, researchers have identified a potential mechanism for the microbe’s pathogenicity. Infection with an Apicomplexa, a phylum of single-celled, eukaryotic organisms, can cause malaria, babesiosis, cryptosporidiosis, and toxoplasmosis in humans and babesiosis, theileriosis and East Coast fever in cattle. For a review of those parasitic infections, check out the video below. The new work, performed by researchers at Whitehead Institute for Biomedical Research, revealed a protein seen in all apicomplexans.
"There's never been a really good way of looking at the function of all genes in any apicomplexan parasite," explained Whitehead Fellow Sebastian Lourido. "We've introduced a method to assess the function of the entire genome. This technology can be used to study a variety of topics, from nutrient acquisition and responses to immune pressures to epistasis and genetic interactions. This is an important leap forward in what's possible to investigate in these parasites."
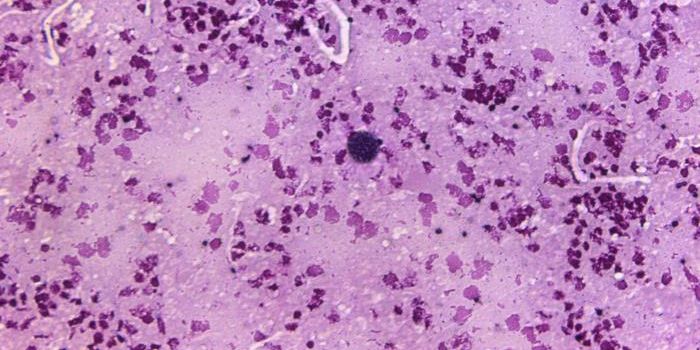
Apicomplexans cause serious heath problems to millions of people worldwide. One such problem is T. gondii; estimated by the CDC to be carried by roughly 60 million Americans. Infection can occur from cat feces or eating undercooked meat, and while symptoms are usually mild and don’t last long, it can cause seizures and possibly, fatal encephalitis in those with weak immune systems such as cancer patients, young children or the elderly. It can be especially damaging to a fetus; an infected mother can transmit the parasite, which can result in miscarriage, damage to the developing child, or stillbirth.
Researchers might be able to use T.gondii as a model organism for the study of an even more dangerous apicomplexan that causes malaria. That parasite is Plasmodium falciparum, and the CDC estimates that it killed more than 430,000 people in 2015. Scientists had to troubleshoot techniques for knocking out genes in T.gondii, however, as typical methods were not working well.
In doing so, the investigators created a CRISPR/Cas9 gene editing system that utilized a Cas9 with reduced efficacy to lessen toxic side effects on the genome. The team then altered each of the 8,158 genes in the T.gondii genome to elucidate functionality. That work indicated 200 genes that had roles in infection of human cells. If you would like to learn more about how CRISPR/Cas9 works from one of the inventors of the technique, check out the video below.
Of those genes, one codes for a protein named claudin-like apicomplexan microneme protein (CLAMP) by the team. It exerts a strong influence on host cell invasion. In collaboration with the lab of Jacquin Niles at MIT, the team reduced the protein in P. falciparum to investigate the role of the protein and confirm its necessity in another apicomplexan organism. It was found that without a functional CLAMP protein, the malaria parasites could not grow in red blood cells.
While the genome-wide CRISPR/Cas9 system has worked well in T. gondii, there is no equivalent strategy for P. falciparum. The team has
published their research in Cell.
"Malaria is really difficult to manipulate in the same way," explained a co-author of the Cell paper Diego Huet, a postdoctoral researcher in the Lourido lab. "Because its genome is adenine (A)- and thymine (T)-rich, it is difficult to generate the cuts where you want. Malaria parasites also lack the non-homologous end-joining pathway of DNA repair, requiring a repair template when making cuts with CRISPR/Cas9. These issues represent a technical hurdle to similar genome-wide approaches in this parasite, making Toxoplasma an even more important model for malaria. There is so much we can study."
Saima Sidik, a study co-author and a research assistant in the Lourido lab added, "Now we can start altering the environment the parasites are in and see how they react. We can permute the environment by adding drugs, adding immune pressures, or trying different cell types for the parasites to invade. We can knock down the whole genome in a week, whereas before we could only do maybe one gene a month. With CRISPR screening, the possibilities are endless."
If you would like to know more about malaria, please watch the video above.
Sources:
AAAS/Eurekalert! via
Whitehead Institute,
CDC,
University of Maryland Institute for Genome Sciences,
Cell