Do you suffer from stomach ulcers? There’s a good chance they’re due to Helicobacter pylori, one of my favorite bacteria!
H. pylori is a spiral-shaped (the “helico” part) Gram-negative bacterium that lives in your stomach - about 50% of the world’s population plays host to
H. pylori. In most cases, colonization causes few, if any, symptoms. That’s the case for about 80% of people. For the other 20%, however,
H. pylori can cause problems ranging from peptic and duodenal ulcers to cancer.
Why helix-shaped? Because it’s cool! Not really. The cells are probably shaped like a spiral because it helps them move through stomach mucous - kind of like a corkscrew travels through a wine cork. The cells aren’t always helix-shaped, however. They can morph into spheres under the right conditions, but they can’t be cultured when in this form.
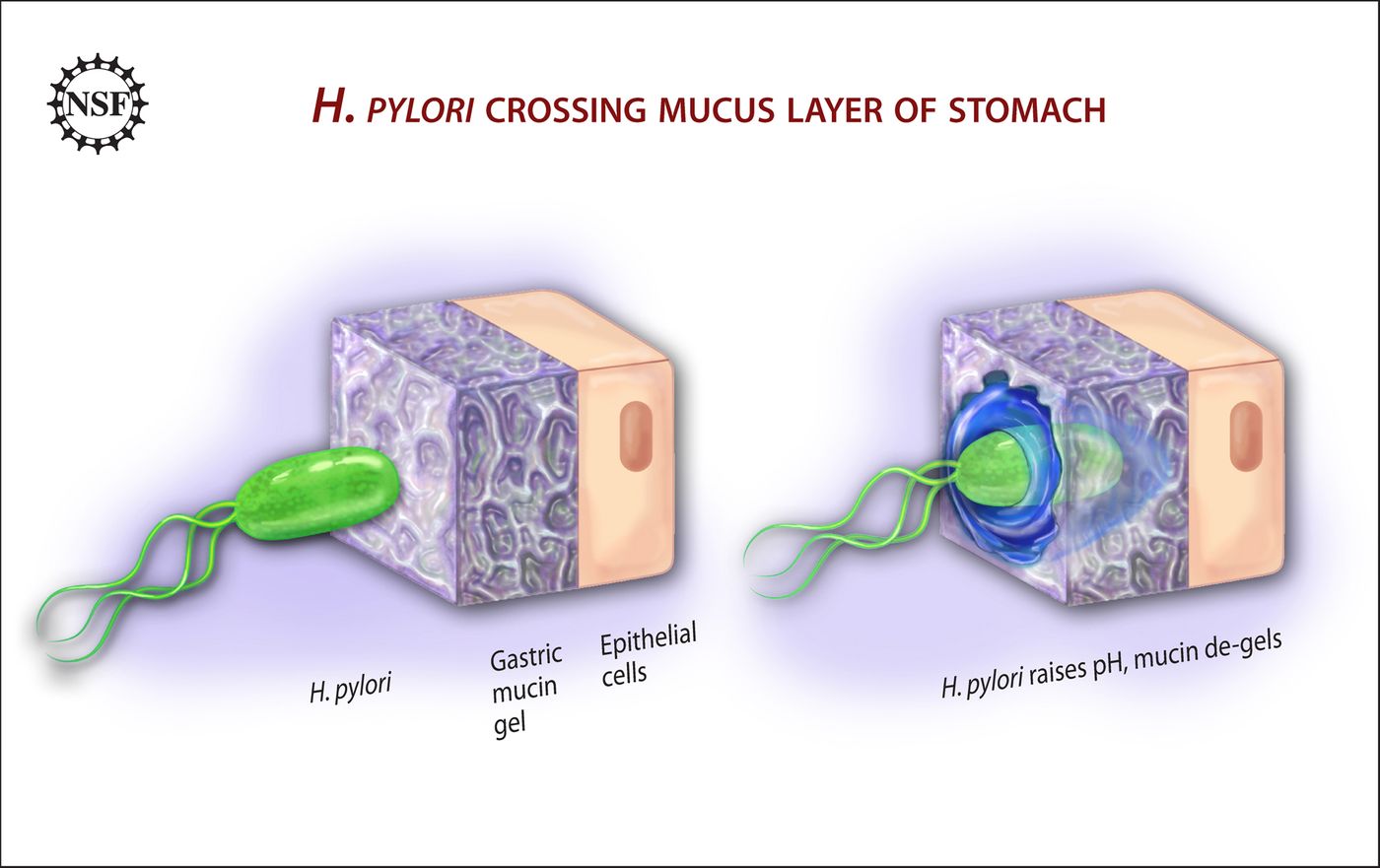
Hold up, you might be wondering how H. pylori survives in the stomach - it’s really acidic, right? Right, but these bacteria have a few tricks up their sleeves. The bacteria burrow their helix-shaped selves through your stomach mucous and cozy up next to your stomach’s epithelial layer - where it’s less acidic. H. pylori also produces urease, an enzyme that breaks down urea into ammonia and carbon dioxide; the ammonia then neutralizes the stomach acid, making it safe for the bacteria.
This all sounds pretty harmless, right? Well, not really. H. pylori damages the gastrointestinal tract in several ways. First, that ammonia? It damages your epithelial cells. The bacteria also produce proteases and a cytotoxin called CagA that, likewise, damage epithelial cells.
There are a couple of hypotheses to explain how H. pylori causes stomach cancer. One says that H. pylori induces an immune response that produces free radicals. These free radicals end up harming host cells, causing mutations that lead to cancer. A second explanation says that cancer occurs through a “perigenetic pathway”. Essentially, inflammatory molecules like TNF-alpha, produced during infection, cause epithelial cell junctions to break down, allowing cells with cancer-causing mutations to spread.
The connection between H. pylori, ulcers, and cancer has a unique origin story. In the early 1980s, Barry Marshall and Robin Warren, two Australian physicians, were convinced that
H. pylori was the cause of a stomach ulcer epidemic in Australia.
H. pylori only infects primates, and there was no way to ethically test the hypothesis on humans. So, like any good scientist, Marshall tested it on himself.
Marshall took bacteria from a patient with stomach ulcers, grew them up in the lab, and drank the culture. A few days later, he developed gastritis - what we now know to be a sign of H. pylori infection and a precursor to ulcers. A biopsy proved his hypothesis - H. pylori infects the stomach, causing ulcers. Both Marshall and Warren were awarded a Nobel Prize in 2005.
Here’s my question, how does H. pylori get into our stomachs in the first place? First of all, the human stomach appears to be the primo spot for these bacteria to grow. However, some strains have been isolated from domestic cats - but there’s no evidence that it is a zoonotic disease (don’t evict your cat just yet). The most likely scenario is that it is passed from human to human, and there are three possible routes.
First, is iatrogenic. This occurs when hospital instruments like endoscopes aren’t properly sterilized - the rates of iatrogenic transmission are considered negligible. The second is fecal-oral. While H. pylori prefers the stomach, it has been isolated from feces. Last, but not least, is oral-oral transmission; although, there’s not much evidence to support this.
Sources: MicrobeWiki,
Discover Magazine, Wikipedia,
Alimentary Pharmacology and Therapeutics,
World Health Organization