Chances are you’ve heard of Lyme disease, but do you really know what causes it?
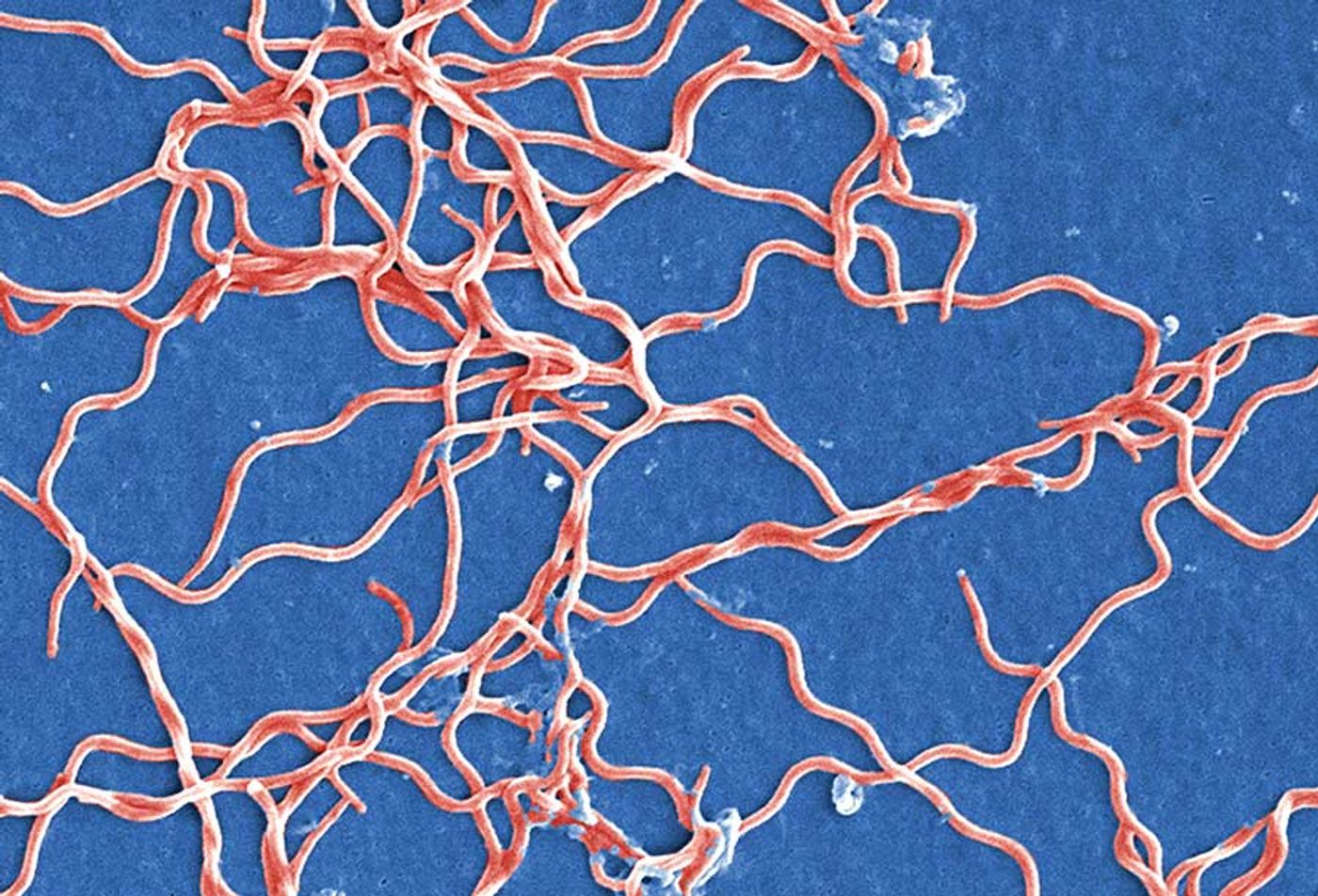
Lyme disease is caused by bacteria in the genus Borrelia ---
Borrelia burgdorferi and
Borrelia garinii are the most prevalent disease-causing species in the US.
Borrelia are actually pretty neat bacteria (if you can look past the Lyme disease stuff). They’re spiral-shaped and aren’t classified as either Gram-positive or negative. Instead, they’re referred to as “diderms”. This is because their outer membrane lacks LPS, and their flagellum is found inside the periplasmic space (in between the outer and inner membranes). Pretty weird.
Borrelia can also survive without iron, making it an ideal pathogen. (The growth of many pathogens is limited by their ability to acquire iron.) Iron is a component of many enzymes, but Borrelia uses manganese instead of iron. Pretty nifty. These manganese-based enzymes could even be therapeutic targets for treating Lyme disease.
According to Valeria Culotta, a microbiologist at Johns Hopkins University, “The only therapy for Lyme disease right now is antibiotics like penicillin, which are effective if the disease is detected early enough … we’d like to find targets inside pathogenic cells that could thwart their growth. The best targets are enzymes that the pathogens have, but people do not, so they would kill the pathogens but not harm people.
Borrelia’s distinctive manganese-containing enzymes such as superoxide dismutase may have such attributes.”
So, how does Borrelia cause Lyme disease? It’s actually a pretty complicated process. Lyme disease is spread to humans when we get bit by a tick that is carrying Borrelia. Deer ticks, and other hard-bodied Ixodes ticks, pick up Borrelia when they bite and feed on small mammals such as mice.
In order to pass from its mammalian to tick host, Borrelia has to regulate the expression of its cell surface proteins. Borrelia uses a protein called OspA to bind to TROSPA (tick receptor for OspA) in the tick’s midgut. In order to reinfect mammals, Borrelia has to migrate to the tick’s salivary glands; this requires the bacteria to downregulate OspA and produce more OspC, which binds to the tick protein Salp15.
Lyme disease is then transmitted to humans by a tick bite --- the bacteria migrate from the tick’s salivary gland into the skin and bloodstream. This isn’t a quick process, however. The ticks have to remain attached to the unlucky human for 36-48 hours for bacterial transmission to occur.
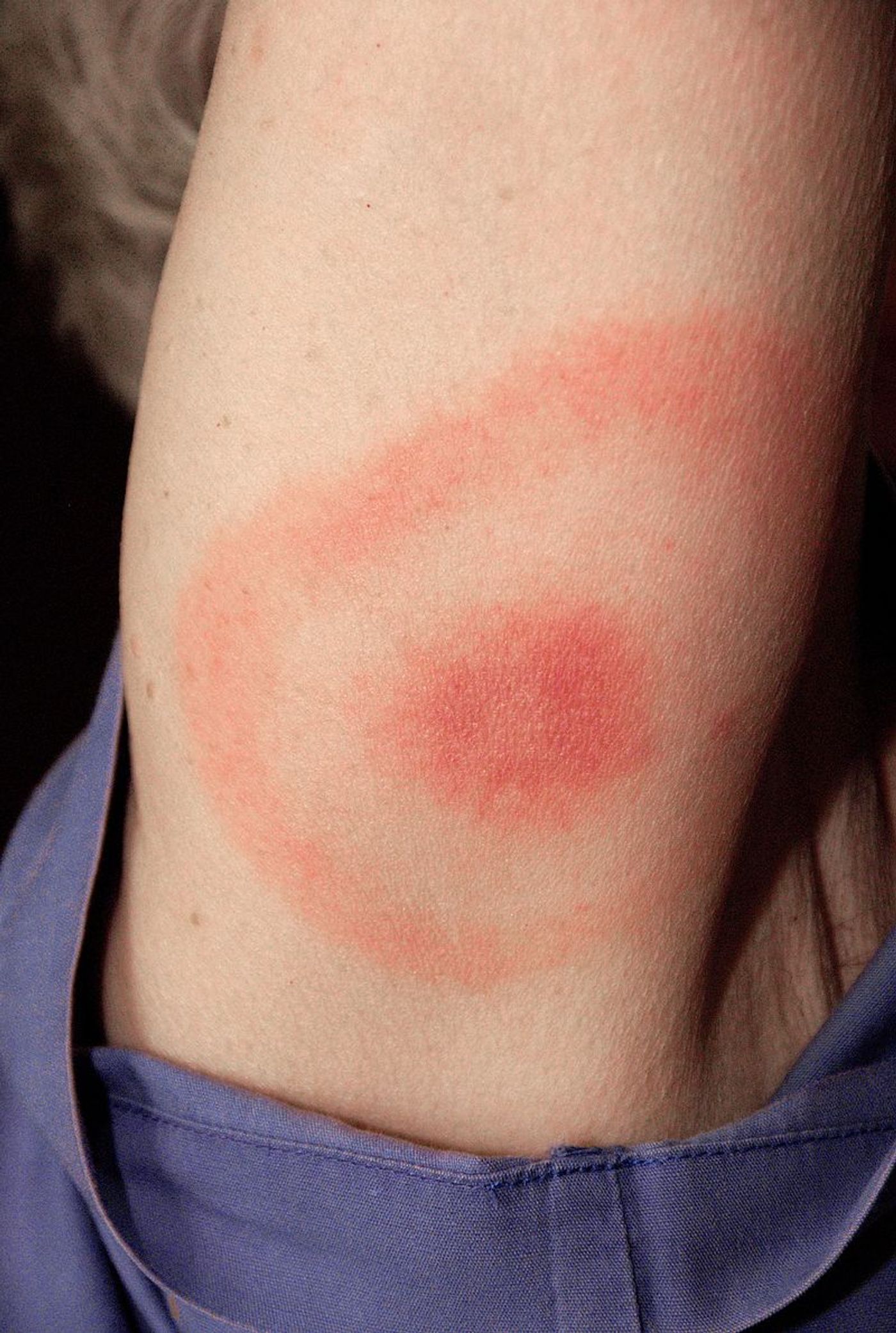
If all of these things occur, people usually develop a bull’s-eye rash (an erythema migrans) at the site of the tick bite. This rash can develop anytime between 3 and 32 days after the bite --- that’s quite a range! Flu-like symptoms sometimes accompany the rash. If people are treated with antibiotics at this point, the disease usually does not progress to a more advanced stage.
Bacteria in the skin are usually destroyed by neutrophils, but, for some reason, neutrophils don’t get recruited to sites of Borrelia infection. This means the bacteria can sneak through the skin and make their way into the bloodstream.
Once in the bloodstream, the bacteria bind the host protease plasmin --- this helps the bacteria disseminate through the blood. As the bacteria spread, people can develop neuroborreliosis. This can cause facial palsy or meningitis. If left untreated, Lyme disease can become a severe, chronic affliction. Chronic encephalomyelitis can develop, causing migraines and motor-control issues. The bacteria probably induce astrogliosis, a process that causes astrocytes in the brain to replicate and then die --- this may contribute to neurological issues.
Lyme arthritis also commonly develops in the knees. Lyme endocarditis, an infection of the heart, is more rare, but can be very serious.
Late-stage, chronic Lyme disease can also be misdiagnosed because the symptoms are often nonspecific, and it is difficult to diagnose. Common misdiagnoses include rheumatoid arthritis, multiple sclerosis, and even Alzheimer’s disease.
Tune in later this week for a closer look at how Lyme disease is spreading across the US and the search for a vaccine.
Sources: Trends in Parasitology,
Clinical Microbiology and Infection,
Lyme Disease Association,
Woods Hole Oceanographic Institute, Wikipedia, MicrobeWiki