The eye microbiome?
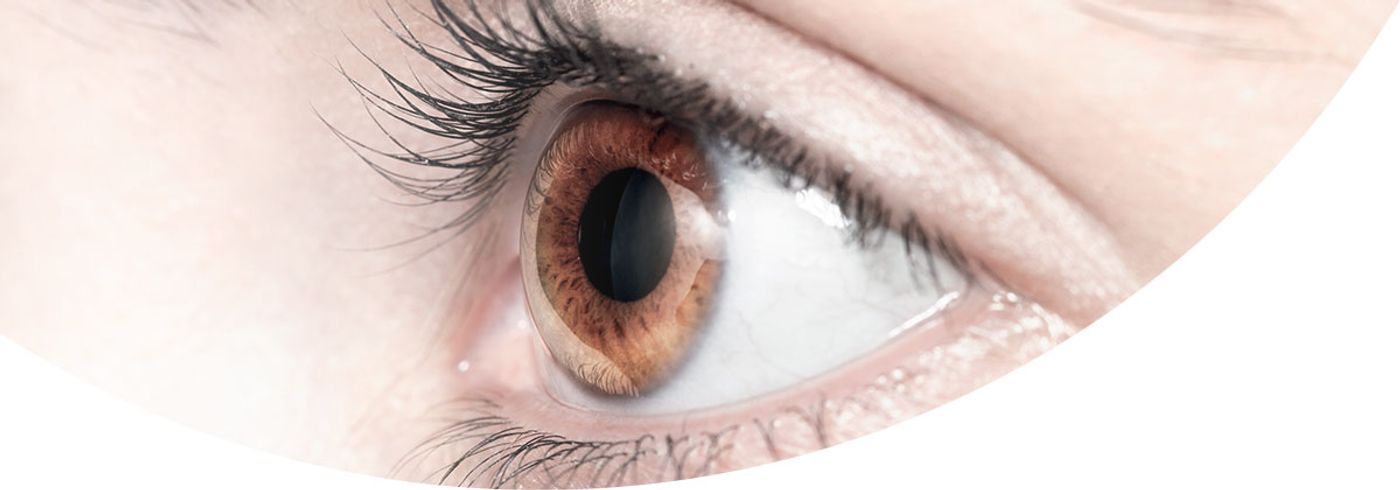
The gut microbiome seems to always make the news, but what about the eye microbiome? Did you even know there was such a thing?
Actually, the existence of an ocular microbiome has been debated - after all, tears contain lysozyme, antimicrobial peptides, and other protective substances. However, researchers at the National Eye Institute have isolated Corynebacterium mastitidis from mouse conjunctiva. What’s more, they also demonstrated that this commensal microbe has an important immunological role in the eye.
Image: Hoya.eu
They report in the journal Immunity that C. mastitidis elicits the production of IL-17 by mucosal γδ T cells (yes, the eye is considered a mucosal site). What’s more, this commensal-specific immune response actually protected the mice from the pathogens Candida albicans and Pseudomonas aeruginosa.
To determine if C. mastitidis could activate immune cells, the researchers added a lysate of the bacterial cells to a culture of dendritic cells and γδ T cells. The C. mastitidis lysate induced the γδ T cells to produce IL-17. Curiously, a lysate of S. aureus had no effect.
To verify that C. mastitidis was responsible for stimulating IL-17 production, they treated the mice with ocular antibiotics. The expression of key genes, including those that produce IL-17, was reduced in the mice that were treated with antibiotics. As expected, fewer IL-17-producing γδ T cells were recruited to the ocular surface in the mice treated with antibiotics. Interestingly, the antibiotic-treated mice did not produce the antimicrobial peptide S100A8 that is found in tears.
Next, they tested whether the presence of C. mastitidis could protect the mice from an ocular infection by the fungus Candida albicans. They applied C. albicans to the conjunctiva and, after 15 hours, collected the corneas. Mice that lacked C. mastitidis (that had been treated with antibiotics) had 10-fold more C. albicans DNA in corneal homogenates. These mice also experienced tissue damage associated with a fungal infection. According to the authors, the results “suggested that bacteria at the ocular surface, which can be eliminated by antibiotic treatment, were necessary to tune local host defense for protection against fungal infection.”
Finally, they investigated whether C. mastitidis could prime the immune system to fight off a bacterial pathogen as well. The researchers applied Pseudomonas aeruginosa to the ocular surface and analyzed the bacterial burden after 48 hours. As for C. albicans, mice that were colonized with C. mastitidis had a much lower bacterial burden and experienced less tissue damage.
Sources: Cell Immunity and Science Daily