Probiotics: The Next Generation
Evidently, we’ve entered the next generation of probiotics. From what I gather, next-generation probiotics are rationally designed to produce some desired effect - combat pathogens, for instance.
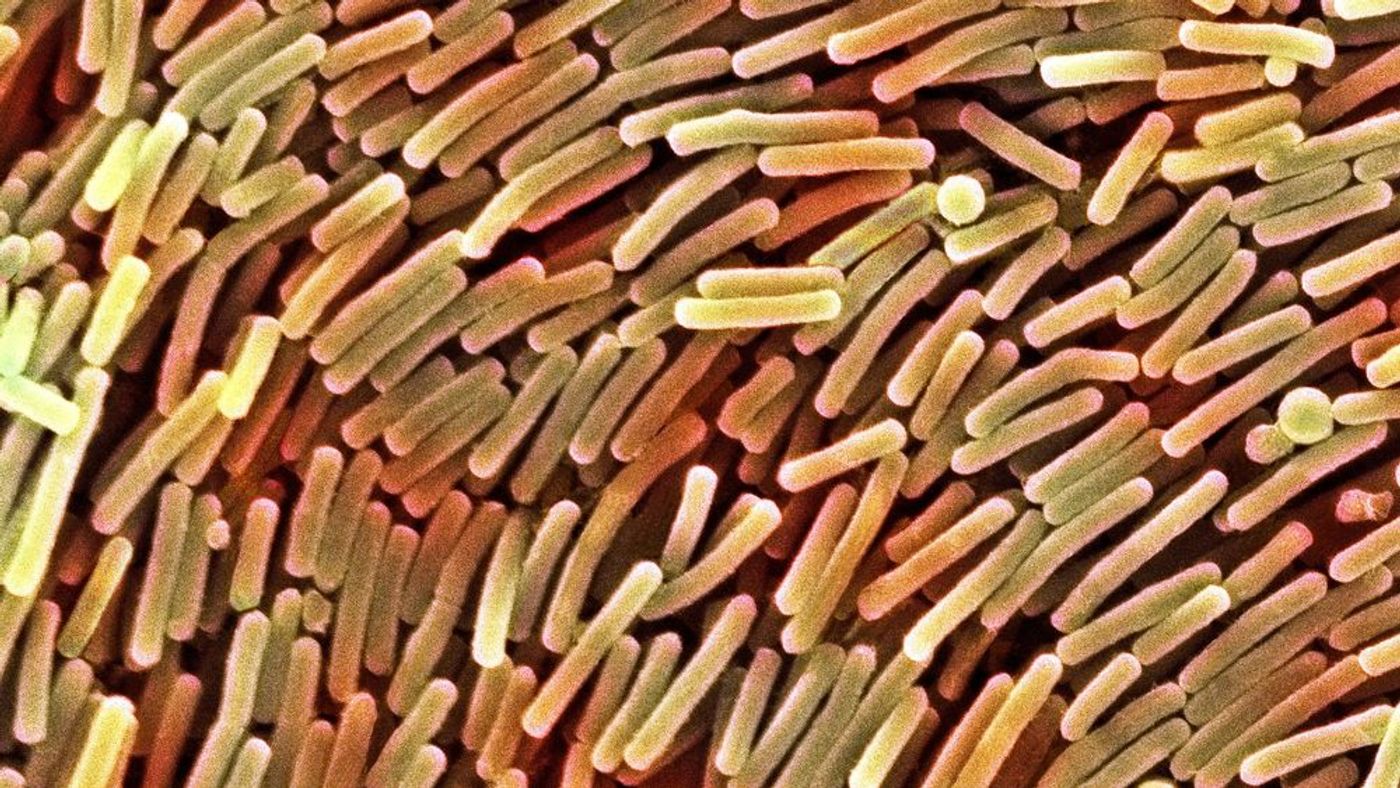
Researchers at Baylor College of Medicine found that the probiotic bacterium Lactobacillus reuteri produces an antimicrobial called reuterin, and this compound is able to kill Clostridium difficile. Interestingly, L. reuteri generates reuterin simply by fermenting glycerol.
Image: Micropia
People most often become infected with C. difficile after the prolonged use of antibiotics, wiping out their resident gut microbes and making way for C. difficile. Often, traditional antibiotics aren’t enough to control the infection. Thus, researchers are looking for other ways to prevent and control this pathogen.
According to study author Jennifer K. Spinler, “when repeated antibiotic treatments fail to eliminate C. difficile infections, some patients are resorting to fecal microbiome transplant -- the transfer of fecal matter from a healthy donor -- which treats the disease but also could have negative side effects. We wanted to find an alternative treatment, a prophylactic strategy based on probiotics that could help prevent C. difficile from thriving in the first place."
First, the team at Baylor looked for a probiotic strain of Lactobacillus that was resistant to the antibiotics used to treat C. difficile infections. After all, it’s no use if your probiotic bites the dust. Luckily, they identified two strains of L. reuteri that survived treatment with vancomycin, metronidazole, and fidaxomicin.
Next, they wanted to know if these strains could produce reuterin and kill C. difficile. Both strains of L. reuteri inhibited the growth of C. difficile in an agar plate-based assay. However, mutant L. reuteri that could not produce reuterin did not kill C. difficile, indicating that C. difficile was susceptible to reuterin.
Then, they validated their findings with human fecal mini-bioreactor arrays. These bioreactors help model what happens in the gut when C. difficile invades. When they added both L. reuteri and glycerol (required to make reuterin) to the bioreactors, the level of C. difficile was 105-fold lower than controls! Treatment with L. reuteri alone (no glycerol) or glycerol alone, however, did not decrease the amount of C. difficile. Interestingly, adding reuterin alone also had no effect on C. difficile, indicating that the presence of live L. reuteri cells is important.
Finally, they treated germ-free mice with L. reuteri and glycerol and applied the animals’ cecal contents to C. difficile. They wanted to see if the cecal contents (presumably containing reuterin) could inhibit this pathogen’s germination and growth. When the mice were treated with both L. reuteri and glycerol, the cecal contents inhibited C. difficile growth by 104-fold. If the mice were treated only with glycerol or L. reuteri, however, C. difficile was able to grow.
According to co-author Jennifer Auchtung, “although these results are too preliminary to be translated directly into human therapy, they provide a foundation upon which to further develop treatments based on co-administration of L. reuteri and glycerol to prevent C. difficile infection.”
Sources: Science Daily and Infection and Immunity