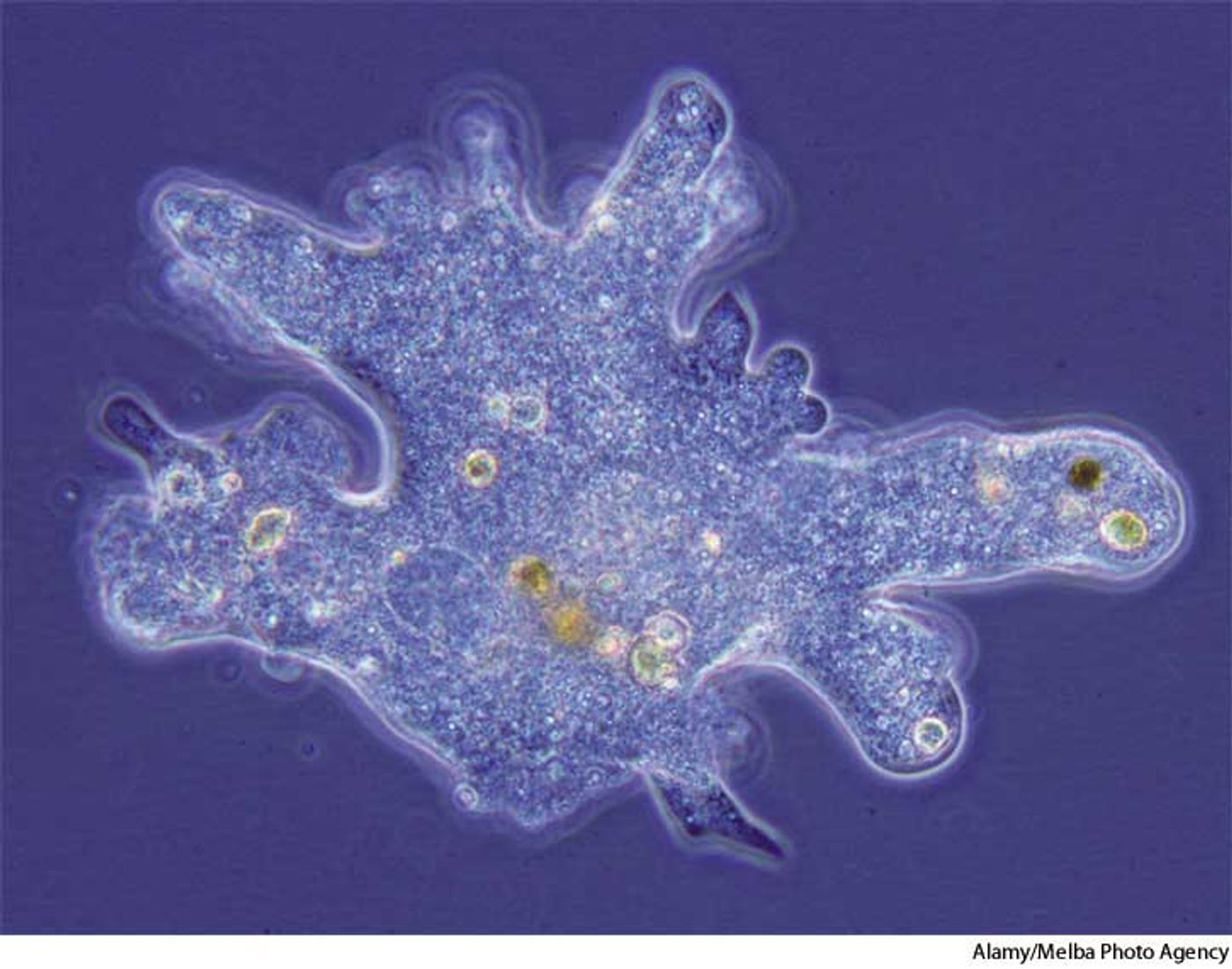
The amoeba's microbiome
With all the talk of the human microbiome, it’s worth pointing out that other organisms- even teeny tiny ones - have microbiomes of their own.
Even amoebas, you ask? Yep, even amoebas.
Image: Alamy/Melba Photo Agency
While free-living amoebas feed on bacteria, some bacteria actually live inside amoebas - sometimes as endosymbionts and sometimes as pathogens. When an amoeba “eats” a bacterium, it is usually digested inside of a phagolysosome. Some bacteria can actually resist this digestion, and that may be how they became endosymbionts in the first place.
Nineteen different bacterial endosymbionts have been identified in amoebas with rRNA sequencing technology, and these comprise 5 different lineages. The number of bacteria in one amoeba can range from between 5 and 100. Some of these bacteria live freely in the cytoplasm, but some hang out in host-derived vacuoles - phagolysosomes modified by the bacteria.
Some of these bacteria aren’t so friendly, however. Some endosymbionts actually lyse their amoeba hosts (in which case, it’s not really correct to call them endosymbionts). For example, O. thessalonicensis lives happily inside an amoeba at 22oC. Turn the heat up to 30oC, however, and these bacteria lyse their amoebas! The change in temperature may signal danger, prompting the bacteria to produce virulence factors.
Interestingly, most of the endosymbionts of amoebas belong to the order Chlamydiales. Some familiar human pathogens also fall into this lineage. For example, Chlamydophila pneumoniae causes community-acquired pneumonia, especially in people with chronic health conditions. Chlamydia trachomatis, of course, causes the STI chlamydia.
Could these chlamydia-related endosymbionts cause disease in humans? Some of these strains have actually been identified (through rRNA and antibody titers) in patients with pneumonia and other respiratory diseases, suggesting that the amoebas may help to spread these potential pathogens.
Indeed, amoebas appear to act as reservoirs and vehicles (tiny Trojan horses?) for Legionella pneumophila. Amoebas and Legionella both live in similar environments (like hot water tanks) and amoebas are often transient hosts of Legionella.
Legionella causes legionellosis, a respiratory illness that occurs when the bacteria are inhaled with aerosolized contaminated water. In 1980, Rowbotham and colleagues proposed that people don’t get legionellosis by inhaling free bacteria. Instead, he reasoned, the disease is transmitted when people inhale amoebas (or vesicles) that contain Legionella! Consistent with this, free-living amoeba are required for Legionella to reproduce in aquatic biofilms.
Some pathogenic species of Mycobacterium can also live inside amoebas. In some cases, endosymbiosis may actually make these bacteria more virulent! M. avium (a human respiratory pathogen) is more virulent when it is grown in amoebas than in broth culture - they invade intestinal epithelial cells and macrophages more readily. M. avium’s intracellular lifestyle also makes it resistant to various drugs, such as the antimicrobials used to treat M. avium in people with AIDS.
As I mentioned earlier, “endosymbiosis” may not be the best term to describe every relationship between amoebas and intracellular bacteria - endosymbiosis implies that both parties benefit from the relationship. In some cases, however, it seems that only the bacteria benefit. To reflect this, some reports describe “amoeba-resistant” microorganisms. These organisms survive phagocytosis by an amoeba and are often capable of multiplying within their host.
As far as amoeba-resistant bacteria go, Listeria monocytogenes, Burkholderia cepacia, and Pseudomonas aeruginosa will all live inside an amoeba if given the chance, as will some human pathogens. These include Chlamydophila pneumoniae (mentioned earlier), Simkania negevensis, Bradyrhizobium japonicum, and Coxiella burnetii.
Sources: The Journal of Eukaryotic Microbiology, Clinical Microbiology Reviews, Journal of Bacteriology