Cleansers, Antibiotics may Contribute to Growth of MRSA in the Home
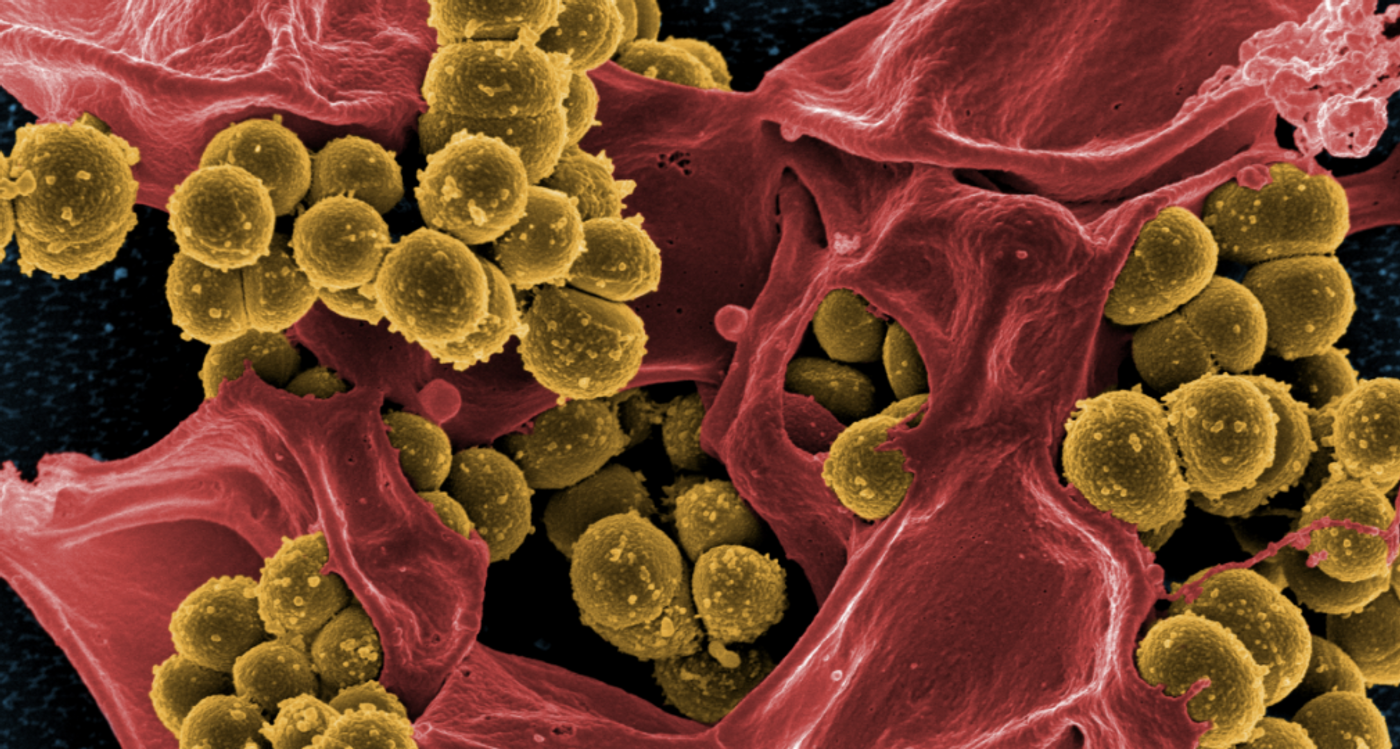
Researchers have found that some things typically found in our home environments may be contributing to the reinfection of people and pets with MRSA, methicillin-resistant Staphylococcus aureus, a dangerous pathogen. Cleaning agents that kill microbes, like bleach, and antibiotic use by people and on pets have been associated with both MRSA reinfection and treatment failure. This work has been reported in the journal Applied and Environmental Microbiology, and it shows that antibiotics must be used carefully, as they may do more harm than good in some cases.
Reinfection with MRSA and resistance to treatment were the focus of this study, said corresponding author Jonathan Shahbazian, MPH. The investigators also showed that one antibiotic, clindamycin, is not associated with a risk of multi-drug resistant bacteria in the home, whether it is used in humans or their pets.
However, an antibiotic called mupirocin, which treats skin infections and can remove MRSA from the nasal passages, thus stopping it from spreading in a sneeze, is also weakly associated with mupirocin resistance in the home environment.
That might complicate efforts to remove pathogenic bacteria from the home using techniques “that rely on [the] use of nasal mupirocin ointment," said Shahbazian. In addition, one hundred percent of MRSA samples that had been obtained from rural homes were found to be multidrug resistant, "suggesting living in a rural household may be a risk factor for multidrug resistance,” added Shahbazian.
"We also found the presence of domestic pets was associated with multidrug-resistant MRSA in the home environment, while the presence of unwanted pests, such as mice or cockroaches, was associated with non-multidrug resistant MRSA strains," said Shahbazian.
For this work, the scientists gathered samples from household environments and companion animals that were enrolled in a large, randomized trial, which was conducted over a fourteen month period. The researchers wondered if common tools used to eradicate MRSA, such as chlorhexidine body wash or mupirocin ointment, had successfully reduced the recurrence of MRSA among kids and adults who had been diagnosed with a MRSA infection of the skin or soft tissue. In 65 homes, sampling was repeated for three months after residents had received treatment for MRSA. In control homes, the sampling was done after residents had been given information about MRSA.
"Based on the evidence, we strongly suspect that environmental contamination of the home with MRSA contributes to recurrence," explained Mr. Shahbazian. The researchers also think that selective pressures on household environmental MRSA pathogens encourage the growth of multidrug-resistant strains. "We hypothesize that infected or colonized people and companion animals shed MRSA into the home environment," which can then sicken household members again.
Learn more about MRSA from the video.
The investigators found that a thorough understanding of what creates multidrug-resistant strains of MRSA in home environments, which makes them much more challenging to effectively treat, may help identify which homes are more likely to contain multidrug-resistant MRSA. That knowledge could then be used to eradicate the pathogen completely.
Sources: AAAS/Eurekalert! Via American Society for Microbiology, Applied and Environmental Microbiology