Experts Call for Alternatives to Antibiotics for Small Infections
Scientists anticipate that at the current rate of antibiotic prescriptions, bacteria will evolve to the point of making antibiotics virtually useless by the middle of the 21st century. From the Georgia Institute of Technology, scientists describe the need for new strategies to prevent this from happening.
What contributes to antibiotic resistance? Many different things, including doctors writing prescriptions for antibiotics for a patient’s sore throat without knowing if the infection is actually a bacterial problem, as opposed to a viral problem. Antibiotics are completely ineffective at fighting viruses.
Additionally, broad-spectrum antibiotic drugs are often prescribed to treat minor infections. This is a kind of drug that kills the both the bacteria responsible and other types of bacteria, many of which are actually playing positive roles in the human body, like protection against “bad” bacteria. The same type of broad-spectrum drugs also tend to kill the weakest population of bacteria, leaving the strongest, most-resistant leftover to multiply.
"Then later, if you have to have surgery, you have a problem,” explained Georgia Tech associate professor Sam Brown. “Or you give that resistant [bacteria] to an elderly relative."
So why are existing strategies not working to reverse the effects or to prevent further antibiotic resistance? In general, scientists are focusing on new drug development strategies in the context of severe infections instead of in small infections. The need for effective antibiotics in cases of severe infections is certainly dire, but according to the study scientists, it is the small infections that contribute most toward bacterial resistance to antibiotics in the first place.
"Antibiotic prescriptions against those smaller ailments account for about 90 percent of antibiotic use, and so are likely to be the major driver of resistance evolution," Brown explained. "It might make more sense to give antibiotics less often and preserve their effectiveness for when they're really needed. And develop alternate treatments for the small infections.”
The journey to new drug development has not been free of obstacles; in fact, the journey has been more obstacles than triumphs. Scientists have had difficulty finding effective alternatives to currently-used antibiotics. Until a solution can be found, experts from the study suggest that using antibiotics should be reserved for the most severe infections.
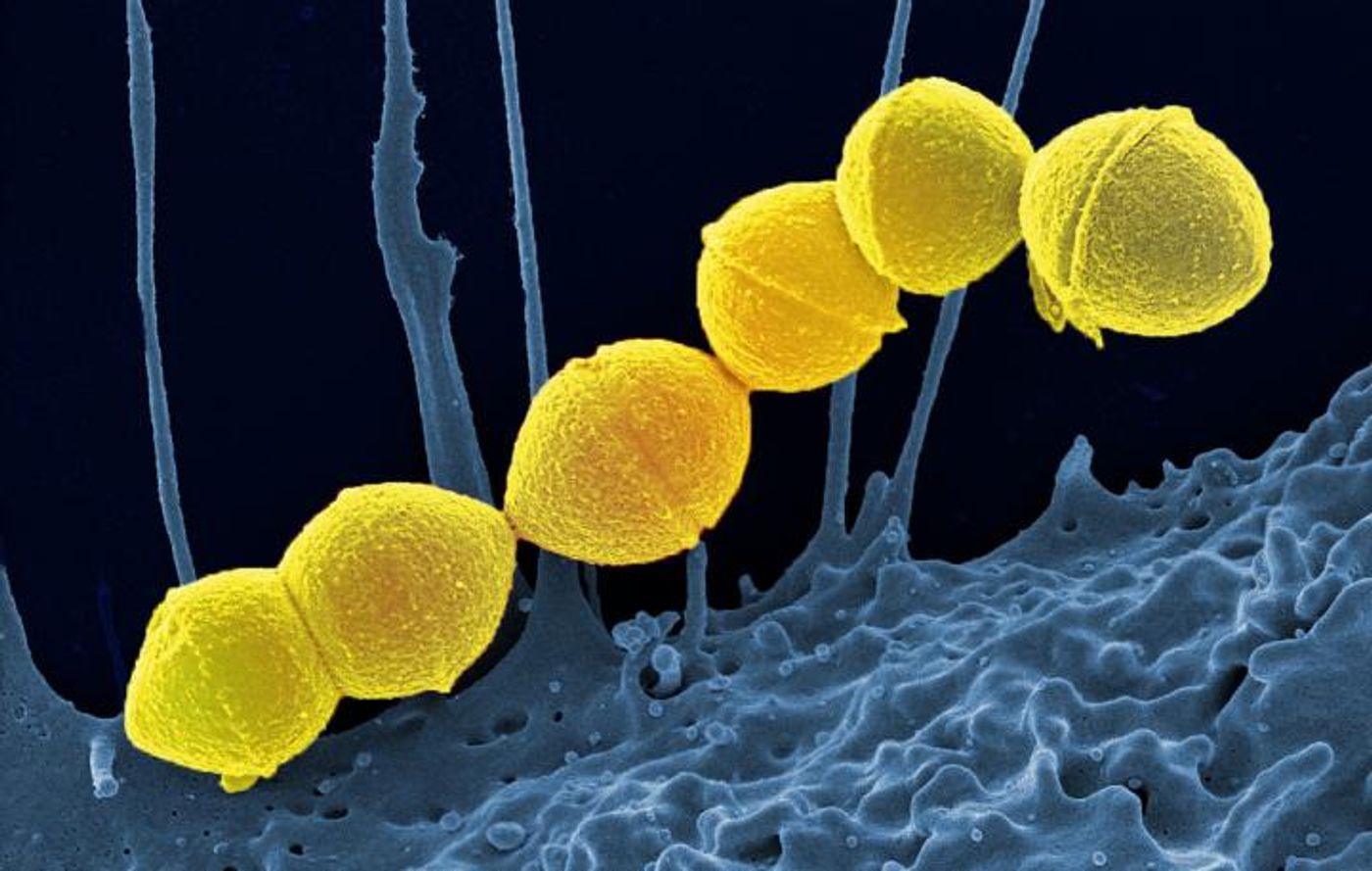
For minor but common bacterial infections, they suggest non-antibiotic therapies. For example, a drug could target the spread of bacteria as well as symptoms of an infection, like inflammation during strep throat. In theory, non-antibiotic drugs could hinder the infection just enough to let the immune system take over a kill the infection on its own.
The present study was published in the journal PLOS Biology.
Source: Georgia Institute of Technology