The CDC's Plan to Combat 'Nightmare' Bacteria
We share the world with bacteria, and much of it is harmless. Some bacteria cause serious illnesses when they infect people, and we have been able to control many of these pathogenic microbes with antibiotics. But a few of those illnesses are becoming harder to treat; antibiotic-resistant bacteria are spreading, and are becoming a growing public health concern worldwide. Some have been called ‘nightmare bacteria’ because they are so deadly.
The misuse of antibiotics is a big reason why resistance is spreading. When only a portion of an antibiotic prescription is taken, a few bacteria survive in the patient, and they are left to multiply, creating a group of bacteria that isn’t affected by the drug. Bacteria can also easily share genes; many of those genes are carried on plasmids, which are independent of the bacterial genome.
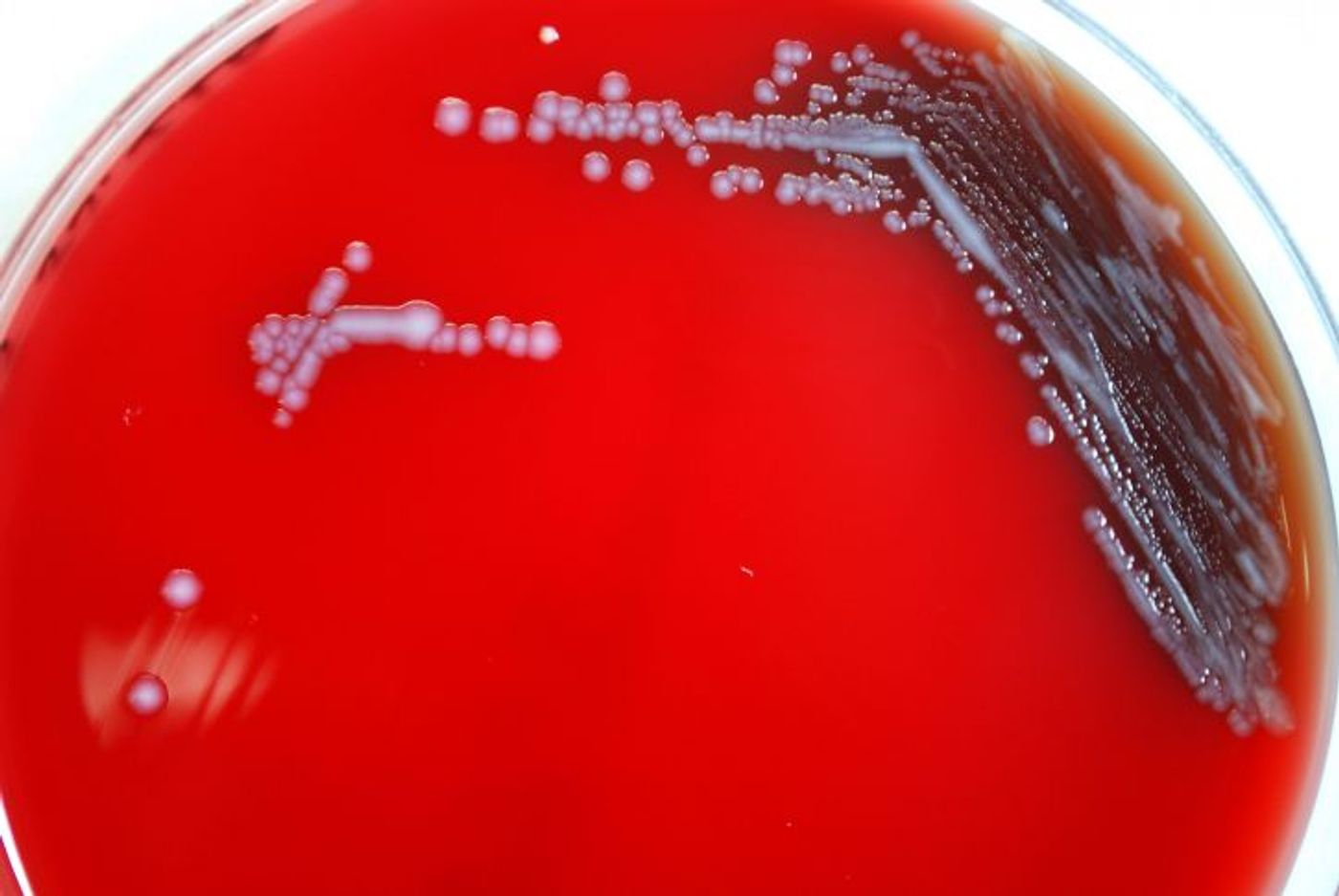
One of the biggest threats comes from carbapenemases, molecules that can make microbes impervious to carbapenems, which are some of the most potent antibiotics. The Enterobacteriaceae family of bacteria is the one that causes the most infections in hospitals, and that family began to pick up resistance to carbapenems. In 1988 these microbes, called CRE for carbapenem-resistant Enterobacteriaceae, were first identified. Plasmids spread carbapenem resistance, and efficiently enough that by 2001, the carbapenem-resistant bacteria were becoming impervious to other antibiotics as well. It became evident that more aggressive strategies were needed.
The Centers for Disease Control and Prevention (CDC) issued directives in 2009 to confront the problem, and there were updates in 2013 and 2015. Now the CDC wanted to survey the state of antibiotic resistance in the United States. Data from 2006 to 2015 from the National Healthcare Safety Network showed that there was a decline in the number of CRE infections in hospitals.
However, there are still a lot of antibiotic resistance genes lurking out there. Incredibly, fifteen percent of the bacterial samples tested carried some kind of resistance to antibiotics - some it was very unusual. "I was surprised by the numbers" of such bacteria commented Dr. Anne Schuchat, CDC’s principal deputy director. "This was more than I was expecting."
The CDC has created new guidelines so that antibiotic-resistant bacteria can now be rapidly identified and controlled, even the rare strains that apparently more common than was known. This work highlights the importance of prevention and containment strategies that work. Around 23,000 Americans are still killed by antibiotic-resistant bacteria every year, so there is plenty of room for improvement. It is also apparent that we can’t only be looking for antibiotic resistance we know about; we must look for emerging resistance as well.
Sources: CDC, Live Science