Symptoms of multiple sclerosis (MS) seem to get better in the winter and worse in the summer, so a group led by Francisco Quintana at the Ann Romney Center for Neurologic Diseases at Brigham and Women’s Hospital (BWH) sought an explanation.
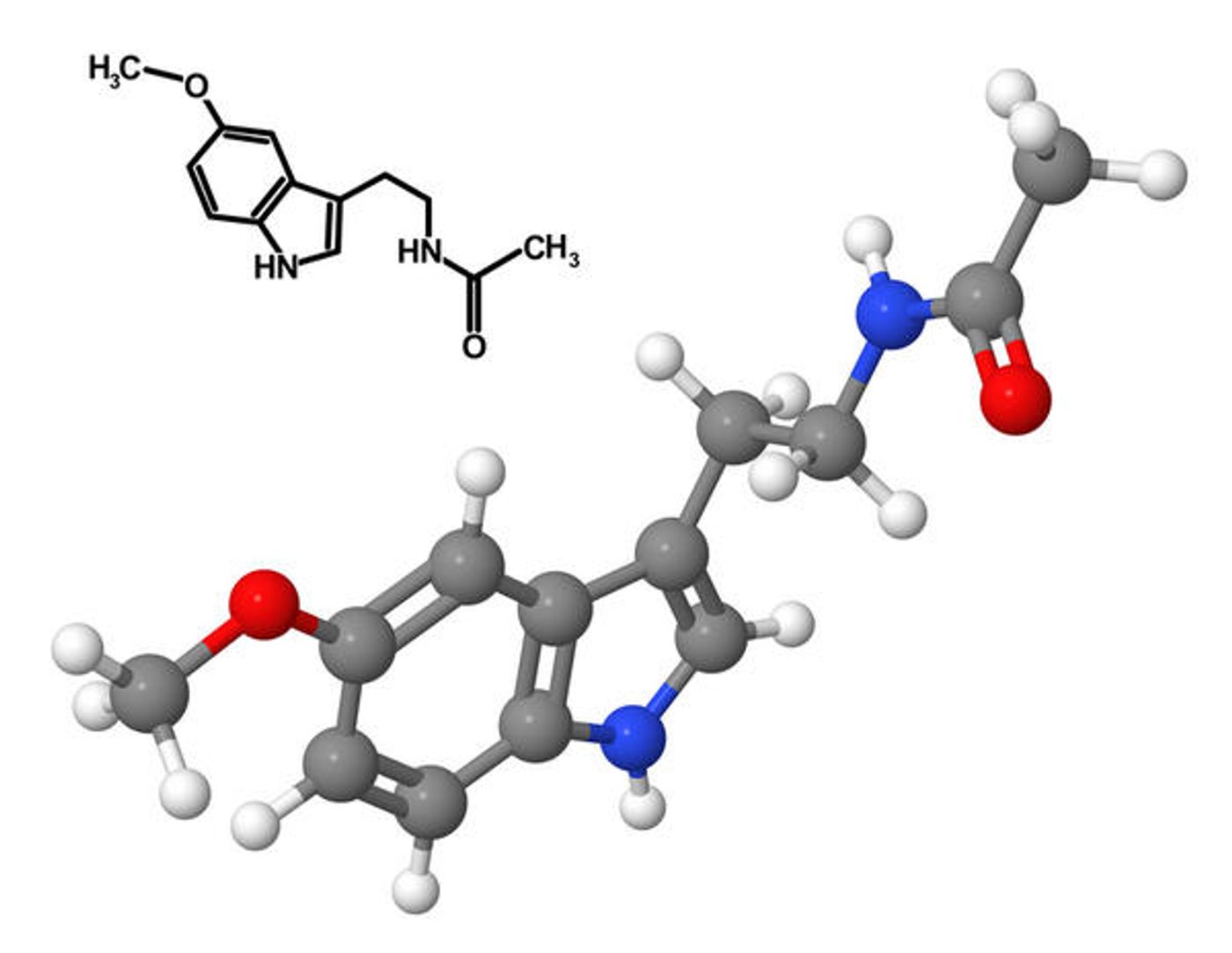
The researchers think they have found one that could lead to a deeper understanding of the disease and more targeted treatment options for patients. By looking at possible environmental factors and then at preclinical models of MS, the research team found that melatonin, a hormone involved in regulating a person’s sleep-wake cycle, may influence MS disease activity. The team reported its findings in Cell, and the work was covered in the
Harvard Gazette and
Bioscience Technology.
While the work does not mean that MS patients should start taking supplements of melatonin, the new approach can be viewed as a first step toward better and more targeted therapies, the researchers said. According to co-corresponding author Quintana, associate professor in the Ann Romney Center and at Harvard Medical School, “We know that for multiple sclerosis and most autoimmune diseases, both genetic and environmental factors play an important role, but in the last decade or so, most research has focused only on the genetic side of the equation. But we wanted to see what environmental factors would reveal to us about this disease. We knew that MS disease activity changed with the seasons. What we’ve uncovered offers an explanation for why that is the case.”
Working with the Center for Research on Neuroimmunological Diseases (CIEN) at the Raul Carrea Institute for Neurological Research (FLENI) in Argentina, Quintana’s team started by studying patients. During the fall and winter, the group of 139 relapsing remitting MS patients experienced a significant improvement in symptoms, a phenomenon observed in prior studies. The team explored a variety of environmental factors potentially linked to MS symptoms, including vitamin D levels, UV incidence and upper respiratory tract infections, but the factor consistently associated with severity of MS symptoms was melatonin. During the longer days of the spring and summer, melatonin levels are lower; during the shorter days of the fall and winter, levels are higher.
Based on this finding, the team studied the role that melatonin may play on a cellular level. With a mouse model and human cells, they determined the effects of melatonin on certain types of cells that affect the immune response that leads to MS symptoms. The team discovered that melatonin affected the roles of two kinds of cells that are important in MS disease progression: pathogenic T cells, which directly attack and destroy tissue, and regulatory T cells, which are supposed to keep pathogenic T cells in check.
According to Quintana, “We found that melatonin has a protective effect. It dampens the immune response and helps keep the bad guys — or pathogenic T cells — at bay. In the future, melatonin or its derivatives may be used in MS patients after appropriate clinical trials are conducted and dosage is established. However, extreme caution should be exercised: Our data do not show that melatonin or its analogs are effective in treating MS.”