How Climate Change Worsened Zika Virus Defects
Image: Pixabay
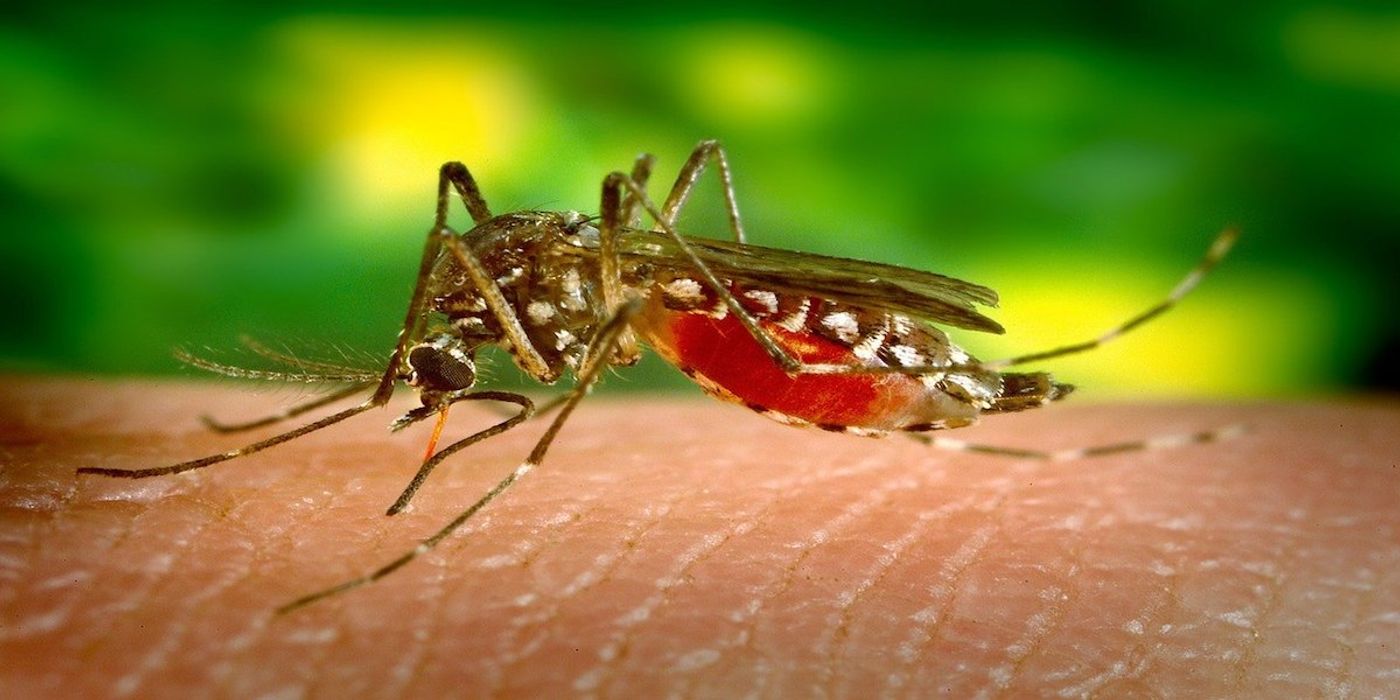
In 2015 a massive outbreak of the Zika virus started in Brazil and spread across 33 countries. The outbreak was especially frightening because mosquitos easily transmit the virus, and risk for pregnant women who contract it is the underdevelopment of their child's skull and brain (microcephaly). Depending on the severity of underdevelopment, microcephaly can cause seizures and developmental delays, among other disabilities.
You may not remember that at the same time, the epicenter of microcephaly cases related to the Zika virus was gripped in an ongoing drought.
In 2012, the northeastern state of Bahia, Brazil, entered a severe drought caused by the El Niño. Freshwater reservoirs evaporated quickly with the exceptional heat, and lack of replenishment. To ease the strain on drinking water resources, residents set up containers to catch the rain. Typically these rain-catchers are poorly covered, making them breeding grounds for Aedes aegypti, the mosquito that carries the Zika virus, and Dengue fever. Freshwater becomes saltier as water evaporates from reservoirs, prompting a bloom of Raphidiopsis raciborskii, bacteria that secrete the neurotoxin saxitoxin. These factors made the perfect storm for two separate, but simultaneous, public health threats.
Saxitoxin is a well-known concern of Brazil's freshwater resources, so R. raciborskii is closely monitored. During droughts, though, higher exposure to saxitoxin is unavoidable. Researchers at the University of Adelaide showed in mice that even in low doses, saxitoxin causes nerve cells to be underdeveloped, stifling communication from the body to the brain and within the brain itself. This finding was later confirmed in an investigation in French Polynesia, linking saxitoxin exposure to Guillian-Barre syndrome.
By 2015, Brazilians in the northeast of the country had been exposed to a higher concentration of saxitoxin for three years, while mosquito populations thrived in the abundance of warm, sedentary rainwater. It was under these conditions that the infamous Zika virus outbreak occurred and terrified expecting mothers everywhere.
Dr. Stevens Rehen, a neuroscientist at the Federal University of Rio de Janeiro, recognized the significance of increased exposure to the neurotoxin combined with Zika virus consequences that also stunt neural development, and began a series of experiments.
In March, Dr. Rehen'sRehen's team published a study showing that congenital disabilities caused by the Zika virus piggyback off the weakened state of the nervous system due to saxitoxin exposure. On its own, a long-term, low dosage of saxitoxin does not damage neurons, while the Zika virus can still cause abnormal brain development without the neurotoxin.
Dr. Rehen's research points to three alarming conclusions that foreshadow the worst ways climate change and pathogens can tangle. The researchers found that a combination of a sustained, low dosage of saxitoxin, and prenatal Zika virus exposure, results in an accumulation of dead cells, more than twice the abundance caused by Zika alone. Cells infected with both also showed a threefold increase in the amount of viral DNA in an infected individual. Worst of all, experiments with mice showed that while prenatal exposure to the Zika virus resulted in some neural-development issues (mostly minor), exposure to the Zika virus and contaminated water caused a severe reduction in brain and skull development, with the cortex reduced by about 30%.
As climate change intensifies weather events, the severity and number of occurrences of climate change and pathogens piggybacking off one another will increase too. Dr. Amy Vittor, who studies mosquito-transmitted diseases at the University of Florida, tells Climate Central, "If you have an increase in temperatures, you may see an increase in range of mosquitoes and the spread of virus." Citing examples of an extended West Nile season in North America, and increasing cases of Dengue Fever in recent years, Dr. Vittor draws a clear pattern of entangled risks that shows no sign of waning.
Sources: Climate Central, Internation Federation of the Red Cross (IFRC), Pedrosa et al., The Scientist, World Health Organization (WHO)