There is an old saying that goes, “When you know better, you do better.” It’s true. When there is an abundance of experience, there is usually an accompanying abundance of knowledge. Experience is the best teacher. A new study out of Canada has shown this to be the case when it comes to treating patients who have suffered an ischemic stroke.
Of course it’s important to know what exactly an
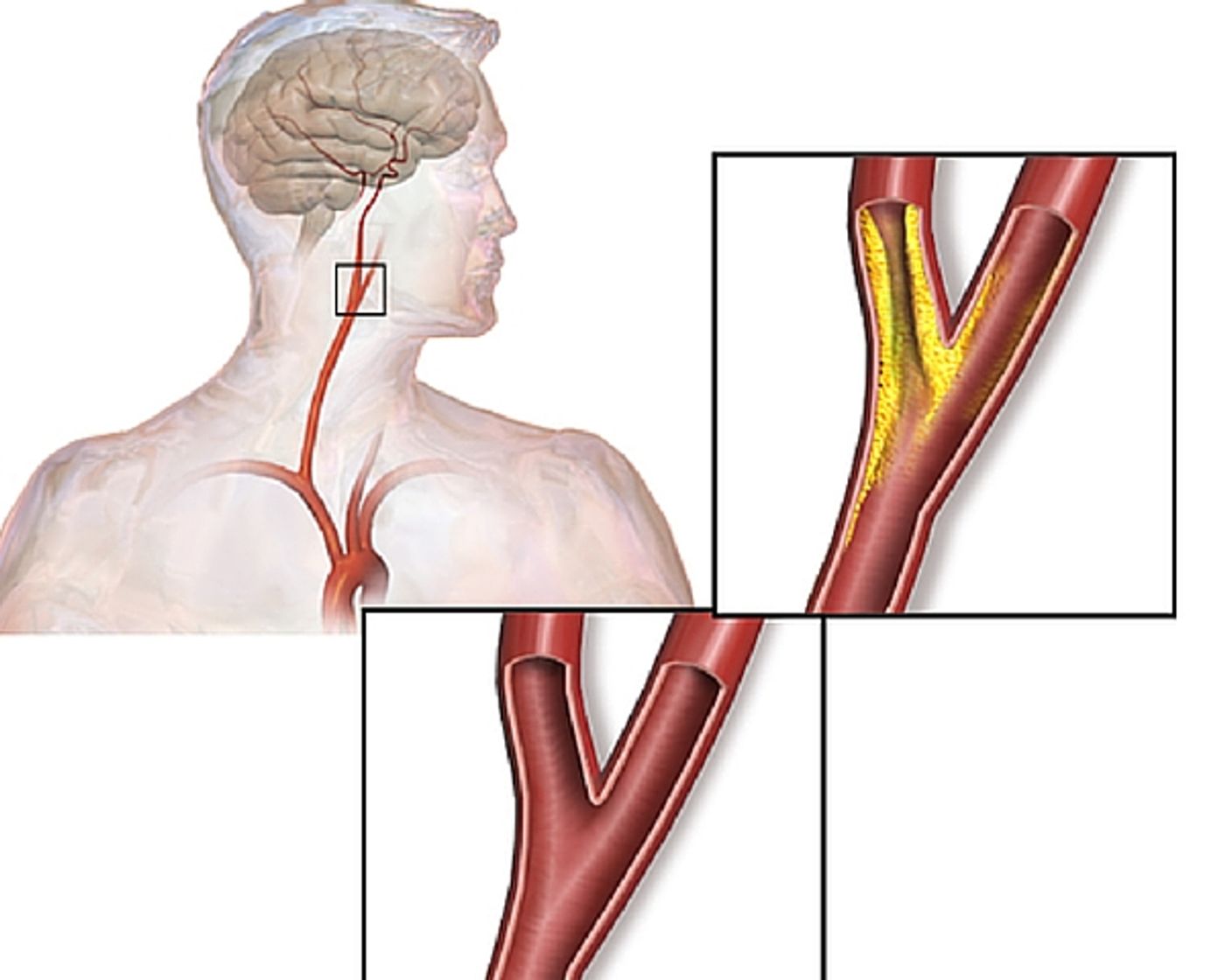
ischemic stroke entails. Ischemic strokes are the most common kind, making up about 87% of all strokes. They are the result of an obstruction within a blood vessel supplying blood to the brain. These obstructions are usually fatty deposits that are lurking in the walls of the blood vessels that supply oxygen to the brain. These deposits can come from external factors like diet or smoking, or they can be genetic and follow family history. They can cause two kinds of obstructions that lead to ischemic strokes. One is a cerebral thrombosis, or blood clot, that develops in one of the blood vessels in the brain. The other is a cerebral embolism. This is usually a clot that is on the move. They normally develop in other parts of the body, and travel along the circulatory system until they hit a vessel to narrow to allow it to pass.
Both of these obstructions can have different causes, but the result is often the same. Blood flow to the brain is compromised and damage can be anywhere from moderate to severe depending on how soon the patient is treated. A recent study from the Institute for Clinical Evaluative Sciences (ICES) and the Ontario Stroke Network (OSN) suggests that not only does it matter how soon a patient is treated, but where that patient is seen is also a significant factor.
The study showed that patients admitted to hospitals that do not see large volumes of ischemic stroke cases are more likely to die within 30 days than patients admitted to hospitals that see large numbers of stroke patients. The province of Ontario has had an established regionalized stroke system in place since 2005. There are currently 28 Ontario hospitals designated as stroke centers, each with protocols and the capacity for appropriate diagnostic tests, expert care and resources for follow up treatment.
The study, published in the journal Circulation: Cardiovascular Quality and Outcomes () is the largest to date to examine the links between stroke care volume and mortality. The researchers reviewed all 73,000 adult ischemic stroke cases at 162 Ontario hospitals in a seven year period between 2005 and 2012. In order to get the best look at the data, the team excluded strokes that happened in the hospital and they followed the anonymous data culled from patient charts to identify deaths that occurred at seven and 30 days following the initial stroke event. Adjusting for various patient risk factors, they compared the likelihood of mortality for each hospital.
In a press release from ICES, lead author Ruth Hall, a scientist at the organization and a lead researcher at the Ontario Stroke Network said, “We found that stroke patients treated at smaller volume hospitals had a 47 per cent higher risk of dying in the first week compared to patients admitted to larger volume hospitals, and a 37 per cent higher risk of dying after 30 days. However, we found no statistically significant difference in rates of death after stroke between medium and high volume hospitals.”
In the same release, Dr. Mark Bayley, a senior author on the paper who is also an adjunct scientist at ICES, and Chair of the OSN Stroke Evaluation and Quality Committee said, “Our study strongly supports the recommendations of the Quality Based Procedures Clinical Handbook for Stroke produced by Health Quality Ontario, the Ministry of Health and Long-Term Care and the Ontario Stroke Network. These findings demonstrate that by consolidating acute stroke care in each region in Ontario, we can ensure that every person experiencing stroke will receive the best possible care.” Check out the video below to hear from Dr. Hall and get more information on the study.