Patients who have experienced certain cardiac conditions or blood clots often are placed on blood thinners to avoid further issues. The most common drug is warfarin, known by its brand name as Coumadin. The problem with the drug is that while it will help prevent clots or other conditions, it increases the risk for intra-cranial bleeding and stroke. A new study, published March 9, 2016 in the journal JAMA Cardiology puts that risk at a much higher level than what doctors have known up to now.
One of the most common conditions for which Coumadin is prescribed is
atrial fibrillation or “a-fib.” It’s a disruption in the heart rhythm and the electrical signals that cause it to beat regularly. When it occurs, instead of blood moving in and out of the atria of the heart normally, the beats are irregular and as a result, blood can pool in the heart chamber and cause a clot. A blood clot in the heart can cause cardiac arrest, or, if it travels to the brain, a devastating stroke.
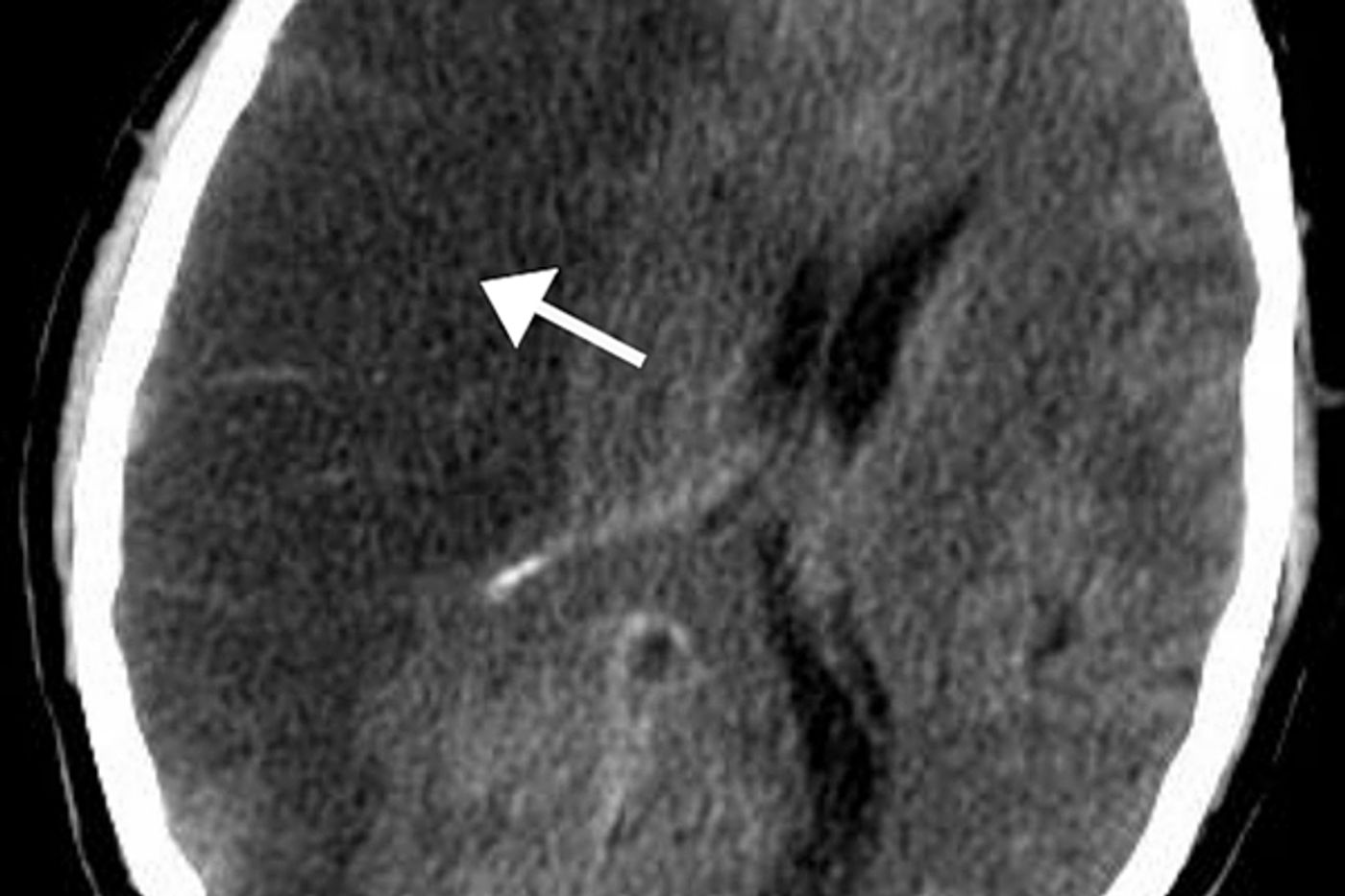
In the most recent research on warfarin, doctors looked at the records of almost 32,000 veterans aged 75 or older who had A-fib. Their analysis found that nearly 1 in 3 of these patients experienced an intracranial bleed while on the medication.
Dr. John Dodson, the lead author of the study and an assistant professor in medicine at NYU Langone Medical Center, said in
a press release, "Atrial fibrillation ("a-fib") is a common heart rhythm disorder in elderly patients. And in patients with a-fib, treatment with the blood thinner warfarin reduces the risk of stroke by nearly two-thirds.However, many clinicians are hesitant to prescribe warfarin in elderly patients, often because of concerns over head trauma due to falls, which can result in catastrophic bleeding." said Dodson. He is assistant professor of medicine at NYU Langone Medical Center in New York City. Dodson said that there were no large studies that had looked at the incidence of brain bleeds in patients and what risk factors might put patients in more danger.
Dodson and the team of researchers that worked on
the study analyzed data from the Veterans Administration and tracked patients and outcomes over a 10 year period (2002-2012) The finding of nearly one third of patients experiencing a brain bleed was surprising, especially given that many patients still experienced a stroke, so the increased risk was without benefit in some cases. The study also detailed other conditions that could increase the risk for this kind of bleeding in the brain and they included the use of anti-seizure medication, and co-morbid conditions of anemia, dementia and depression.
The challenge in using blood thinning drugs is to balance the need to prevent clots with the risk of stroke and brain bleeds that can be life-altering as well as life-threatening. Dr. Richard Temes, director of the Center for Neurocritical Care at North Shore University Hospital in Manhasset, N.Y. who was not involved in the study told
Newsmax, “As physicians, we need to carefully weigh the risks of using blood thinners in the elderly population, which is prone to falls and head injury, with the risks of stroke.”
Take a look at the video below to see more about the study and the dilemma many doctors face when prescribing blood thinners to elderly patients.