Differences between Hodgkin and non-Hodgkin Lymphoma
Lymphoma, broadly, describes a type of cancer that develops in the lymph system, a complex network made up of organs, nodes, ducts, and vessels. Lymph, a clear or white fluid consisting of white blood cells, also known as lymphocytes, and intestinal fluid, called chyle. The lymphatic system transports lymph between bodily tissues and the blood, and the movement of lymphocytes throughout the body is an essential component of the immune response.
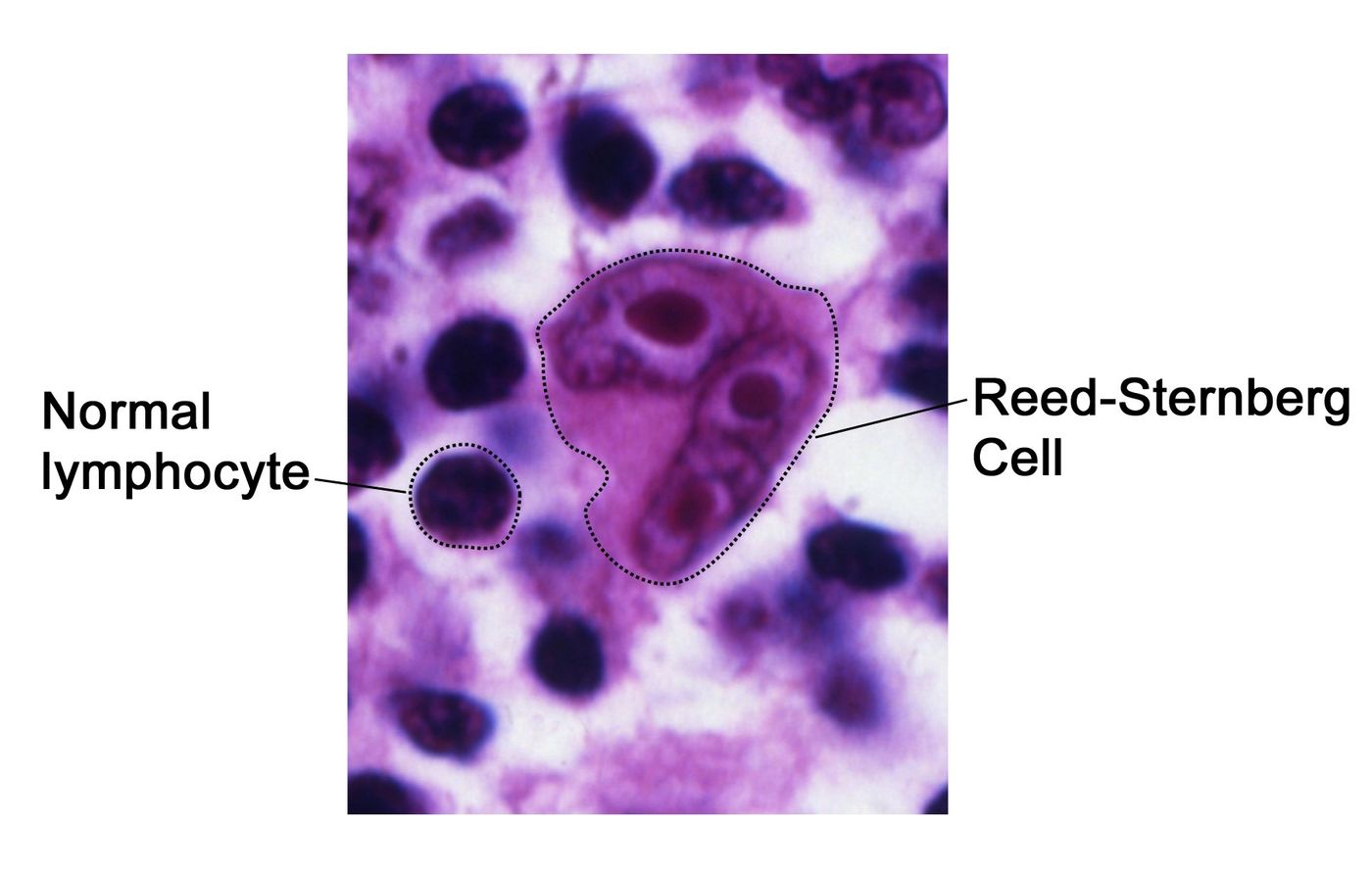
Lymphoma is divided into two main classifications: Hodgkin lymphoma and non-Hodgkin Lymphoma (NHL). While both Hodgkin and non-Hodgkin’s lymphomas impact the lymph system, doctors can distinguish them by evaluating a biopsy for Reed-Sternberg cells, present only in Hodgkin lymphoma. Reed-Stemberg cells originate from lymphocytes that have mutated to become enlarged and multinucleated. NHL can be divided into more than 30 subtypes, including aggressive cancers like Burkitt lymphoma, diffuse large B cell lymphoma, and mantle cell lymphoma, and slower-growing cancers like follicular lymphoma, cutaneous T-cell lymphoma, and marginal zone B-cell lymphoma.
Hodgkin lymphoma is a relatively rare malignancy with less than 9,000 new diagnoses expected in the US in 2022. On the other hand, NHL remains one of the most common cancers, with over 80,000 new cases expected. When diagnosed early, both types of lymphoma respond well to established treatments, and both have favorable five-year survival rates, currently 87%, and 73% for Hodgkin and NHL respectively.
Because NHL, often diagnosed at a later stage than Hodgkin lymphoma, generates a broader range of treatment modalities. Hodgkin lymphoma is generally treated with chemotherapy or radiotherapy. Occasionally, cancers not responding to these standard approaches may be treated with targeted therapies or immunotherapies.
Compared to Hodgkin Lymphoma, many more subtypes of NHL exist, making the disease more challenging to treat in a broad sense. In fact, NHL has nine standard treatments chosen based on an individual patient's clinical and demographic characteristics. In addition to chemotherapy or radiotherapy treatment options, emerging targeted therapies and immunotherapeutic approaches have become more common.
Several monoclonal antibodies, manufactured proteins that seek out a specific target on the surface of lymphocytes, have become standard treatments for types of NHL. One monoclonal antibody, rituximab, targets a molecule called CD20. When administered, rituximab is directed towards CD20 expressing lymphoma cells where it attacks the cancer cell.
Other targeted therapies used for treating NHL include proteasome inhibitors. Proteasomes, molecules that degrade damaged proteins, facilitate cancer cell survival by clearing out unneeded cellular components. When a proteasome inhibitor, such as Bortezomib, blocks this “clean-up” process, damaged proteins build up in the cell, causing it to die.
Immunotherapies, which boost a patient’s own immune system to help it better attack cancer cells, have also emerged as a viable NHL treatment. CAR T cells, T cells specially engineered to seek out and destroy a patient’s cancer cells, are used in some cases where lymphoma has relapsed or not responded to treatment.
Stay tuned to upcoming Labroots articles on new advances in lymphoma research!
Sources: NCI (Hodgkin lymphoma), NCI (non-Hodgkin Lymphoma), NCI Visuals Online