New Way Forward for Personalized Cancer Treatments
Clinical trials are often long and expensive. And despite the best efforts, clinical trials sometimes end with inconclusive results – an outcome that’s especially frustrating for patients. But, using big data, a new study found evidence to support more cell-based testing of cancer drugs to help doctors make more precise and effective treatment options for their patients, including more accurate assignment of the patients into appropriate clinical trials.
In its most basic form, cancer results from a collection of mutations that make the cells grow and divide uncontrollably. Specific mutations or sets of mutations lead to certain types of cancer, like breast and ovarian cancer, pancreatic cancer, or leukemia. Understanding the nuances between the mutations could help doctors predict how patients will respond to certain drugs, an endeavor that’s at the heart of the Precision Medicine Initiative.
Is there a way we can get to personalized medicine by using cancer cell lines? In many ways, this way of thinking is not new and researchers have done exactly this in the past. But researchers questioned the accuracy of cancer cell lines and whether they truly reflect the mutations observed in patients. No one has really studied this in a systematic manner, until now.
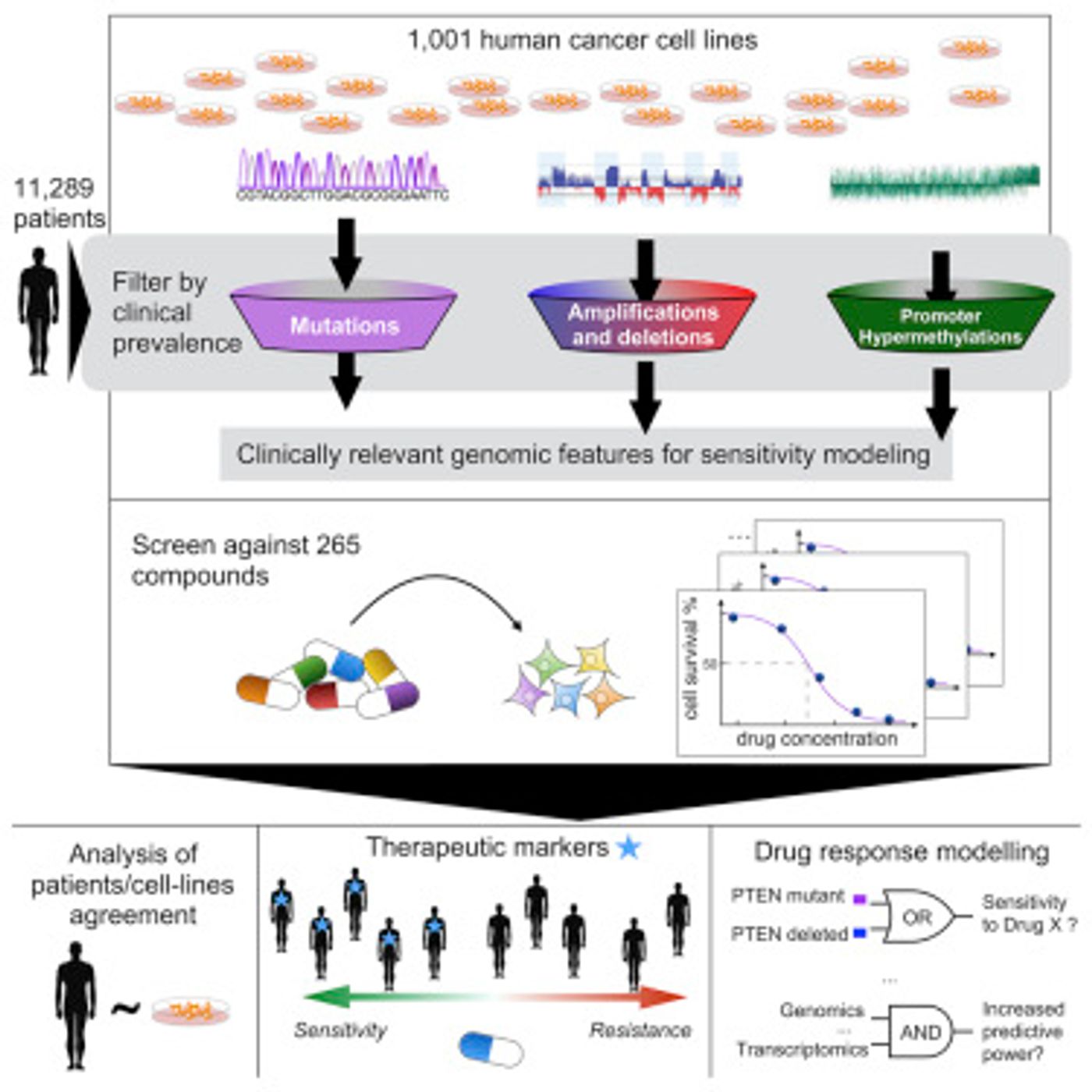
In the largest study to date, scientists from the Wellcome Trust Sanger Institute looked at molecular data from 11,289 patient samples tumors from 29 tissues. They then mapped the mutations to 1,001 known human cancer cell lines, and tested the cells’ reaction to 265 anti-cancer drugs.
They found that cancer cells from patients seem to faithfully mimic the mutations found in the patients. This confirms what researchers already suspected: that cancer cells can serve as good models for the patient’s cancer.
If the cancer cell lines can help doctors predict a good or bad drug response, patients can be treated with the appropriate drug the first time.
"If a cell line has the same genetic features as a patient's tumour, and that cell line responded to a specific drug, we can focus new research on this finding. This could ultimately help assign cancer patients into more precise groups based on how likely they are to respond to therapy. This resource can really help cancer research. Most importantly, it can be used to create tools for doctors to select a clinical trial which is most promising for their cancer patient. That is still a way off, but we are heading in the right direction,” said Francesco Iorio, joint first author and postdoctoral researcher at the Sanger Institute.
Cells have the ability to be easily manipulated and tested, unlike the cumbersome and costly clinical trials. "You can't screen hundreds of drugs across a single patient. It's not possible," said Ultan McDermott, a cancer specialist at the Sanger Institute. "But you can do that with cell lines—you can expose them to many different drugs and ask questions about which is more or less sensitive."
To help as many researchers and patients as possible, Garnett and his team are working to create a web portal to share their data. The idea is to have a database of cells and their mutations, and how the cells respond to certain drugs.
Additional source: Wellcome Trust Sanger Institute