Metastatic melanoma is one of the most savage killers in its ability to escape detection and spread to other parts of the body. Clinically graded as stage IV melanoma, the metastatic form of this disease affects vital organs like the lungs, liver, and the brain.
Now researchers at Tel Aviv University (TAU) may have made headway to detecting possible
brain metastases before it happens. And providing even a short window of opportunity before melanoma overtakes the brain could possibly mean reversing the death sentence for some of these patients.
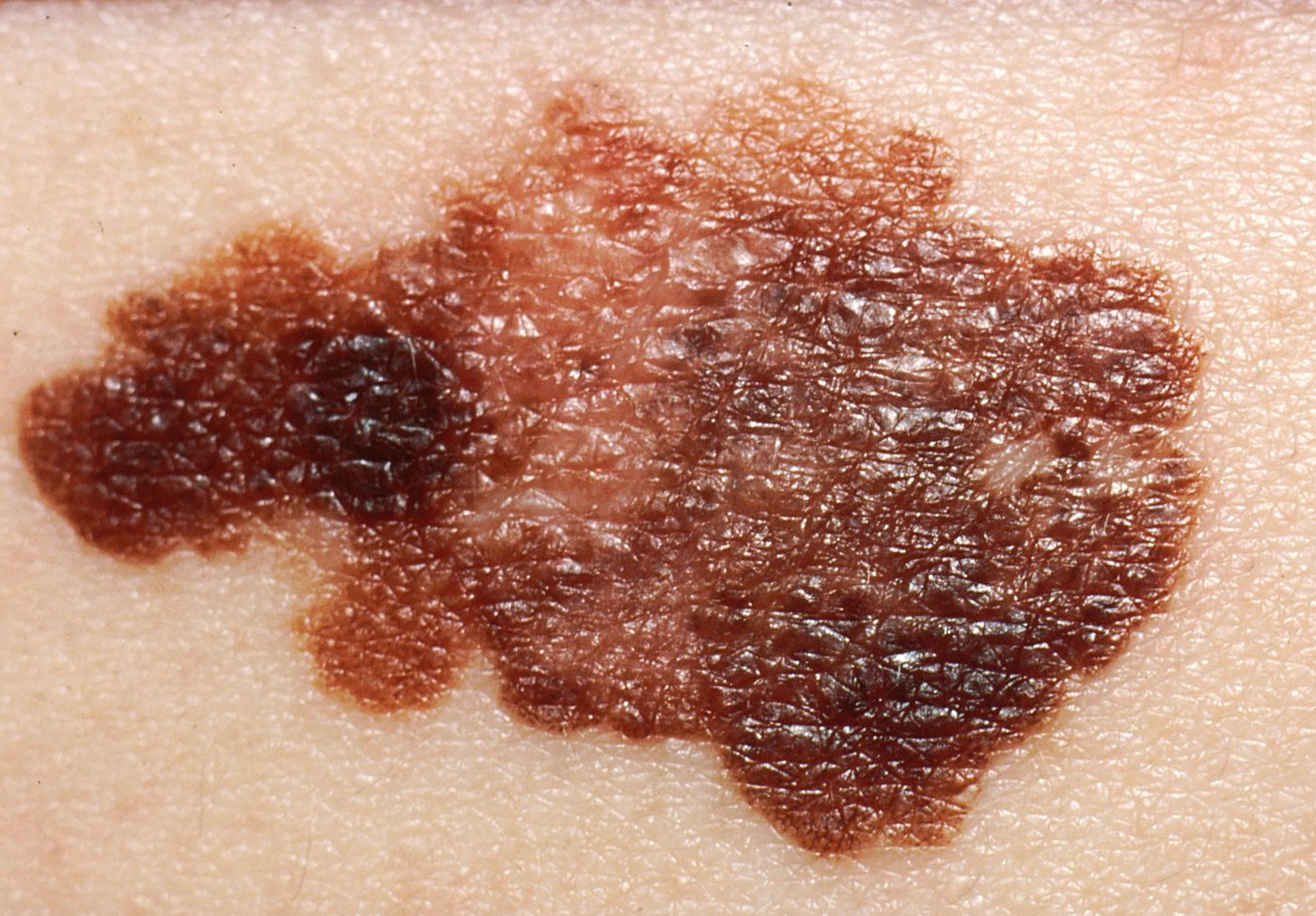
Melanoma is a deadly form of skin cancer caused by ultraviolet radiation damages to the skin cells. According to the World Health Organization, between 2 and 3 million people worldwide have skin cancer. And of that, about 132,000 people have melanoma. The incidence of skin cancer is only rising, as experts believe the depletion of the ozone layer will result in an additional 300,000 new cases every year.
One of the biggest challenges in treating melanoma successfully is the high probability of relapse after initial treatment success. This happens because one of melanoma’s nasty tricks includes subverting the body’s defenses. In the case of the brain, the researchers show that micro-tumor cells can hoodwink the brain’s defense mechanism into letting the tumor cells cross into the brain.
"Every organ in body has a defense system that detects intruders," explained Neta Erez, professor at the Department of Pathology at TAU, and senior author of the study. "Much of this is regulated by support cells in the brain. When there is tissue damage due to a stroke or viral infection, these cells are activated and induce an inflammatory response.”
To protect the body, the brain is activates a process known as astrogliosis. This causes a surge in the number of astrocytes in the brain, which function in neural repair. "At the earliest stages of metastasis, we already see astrogliosis and inflammation. The brain perceives the micrometastatic invasion as tissue damage, activating inflammation -- its natural defense mechanism. We found that the inflammation unfortunately gets hijacked by tumor cells that are able to grow faster and penetrate deeper because the blood vessels in the brain are more permeable than in any other part of the body. We found that all of this happens very early on," said Erez.
This mechanism appears to be how melanoma cells linger around even after removal of the primary tumor. Thus, as is often the case, patients who are treated for melanoma can be lulled into a false sense of security only to find out the cancer was still there all along.
Erez refers to melanoma’s silent spread as a “black box.” But finding out metastases happen isn’t enough to save patients; Erez is moving swiftly to ways to block this action. "We're hoping to develop the detection tools for humans that we developed in mice," Erez said. "We're also trying to find molecular targets that will allow us to prevent metastasis rather than trying to treat it."
Additional source:
Tel Aviv University press release









