Polarity of Cancer Cells Affects Metastatic Ability
After the word “cancer”, perhaps the next most worrisome word in oncology is “metastasis”. Metastases are highly concerning and indicate cancer progression and potential aggressiveness of disease. Research had contributed to the body of knowledge surrounding cancer and outlined the basic steps of metastatic development. The progression of metastasis starts with dedifferentiation of tumor cells, the disconnection of those cells from the primary tumor and intravasation into the blood or lymph circulation, persistence in the circulation environment, extravasation from minor vessels into distant organs and metastatic growth in that new location.
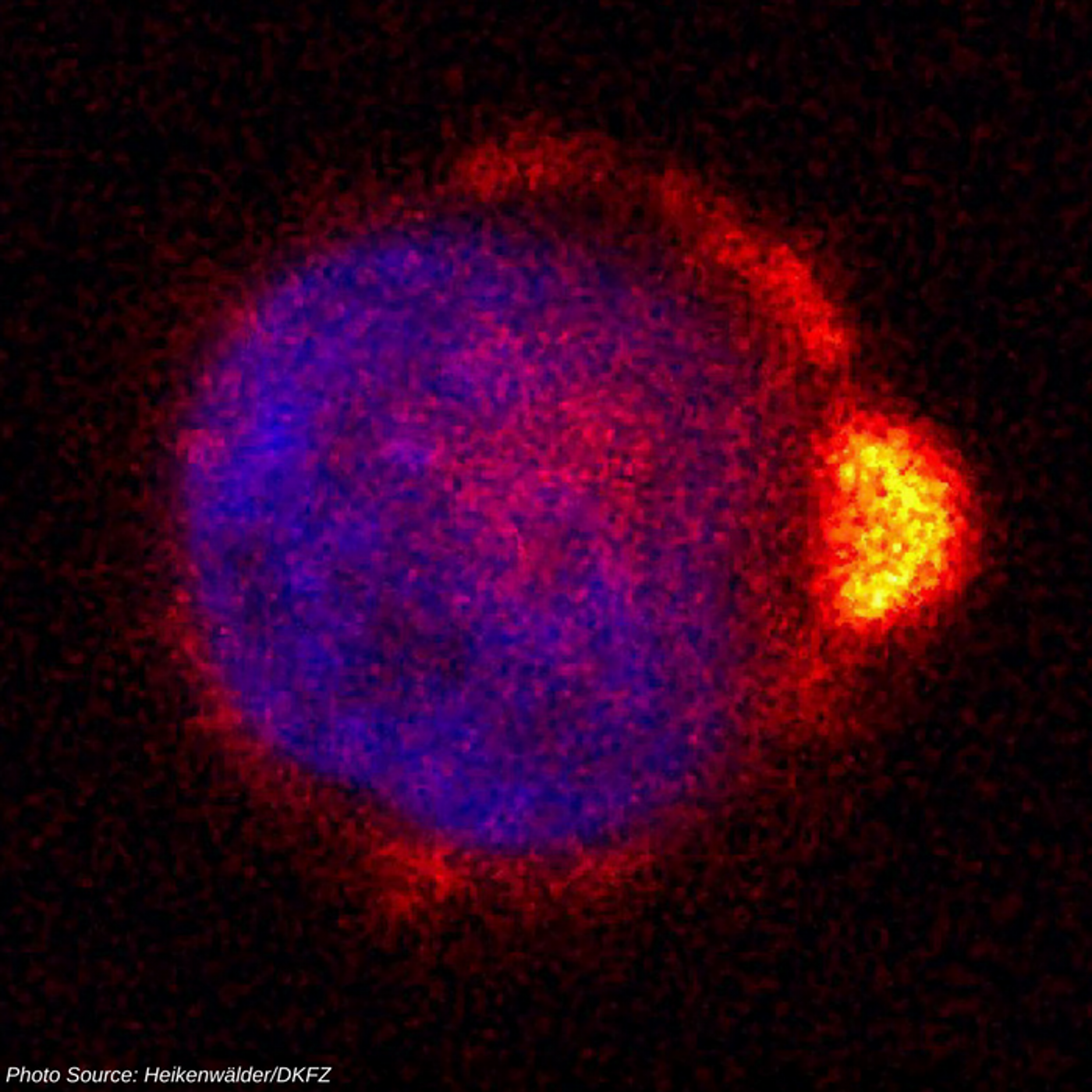
As part of the metastatic process, tumor cells develop polarity based on the needs of the cell. This is not uncommon as a cellular mechanism to carry out physiological processes of the body. Healthy cells depolarize and repolarize to convey messages. Similarly, tumor cells depolarize and repolarize based on their position within the metastatic process cascade. Primary tumors, and established secondary tumors, have been found to have apical-basal polarity. Cells with apical-basal polarity are a result of the manner in which phospholipids, protein complexes, and cytoskeletal components within the plasma membrane are distributed. This contributes to ion exchange and a barrier function to safeguard directionality of secretion and absorption. A common healthy tissue example exhibiting apical-basal polarity are epithelial cells. When tumor cells are in the process of metastasizing, their polarity shifts to front-back polarity. This shift occurs because protein complexes and microtubules move to the front of the cell and the basement membrane degrades to become more flexible. When cells are in a liquid phase, the part of the metastasis progression when tumor cells are exploiting the circulatory system, a study published in Nature Communications in late February 2018, identified another type of polarity which they called single cell (sc) polarity. Single cell polarity is maintained by the utilization of an actin and ezrin-rich pole which positively impacts cellular attachment, adhesion, transmigration, and metastasis. The researchers examined polarity markers within individual human melanoma cells in suspension using labeled probes to known intracellular molecules. Clearly noted was a polar accumulation of actin, plasma membrane receptors, and intercellular adhesion molecules creating a kind of bump on one side of the cell. Additionally, the group investigated tumor cells from liquid phase biopsies of patients to confirm that these observations held true for cells in vivo. They confirmed their observations and evaluated effects of general depolarization on migration patterns and length of migration.
The research data illuminates the correlation of sc polarity with the metastatic properties of tumor cells and provides hypotheses about the mechanisms and value of these cellular changes. The sc pole (aka the bump) with accumulated intracellular glycosylated proteins may lead to nonspecific contact with substrate and enhance early attachment. An additional finding included a pre-polarization stage which promoted full adhesion of these cells to begin colonization of that potential new tumor site. Researchers used knockdown models of ezrin and melanoma cell adhesion molecules alongside normal and overexpression models to evaluate the impact of expression of these complexes on sc polarity. The findings demonstrated consistently that the adhesion molecule knockdown models reduced adhesion abilities under flow or fluid conditions. Overexpression models indicated increased transmigration abilities through a layer of human umbilical vein endothelial cells.
This evidence furthers the need for additional research into mitigating these cellular changes and finding medicines that could target these roaming cells before metastasis occurs.
Video Caption: In migrating cells, patches of actin filaments (red) are found at the front, while the protein Callipygian (green) is found at the back. Video Credit: Kristin Swaney, Johns Hopkins Medicine
Sources: German Cancer Research Center DKFZ, Nature Communications, MechanoBiology Information,