Jessica Wagenseil, PhD, and her team from Washington University in St. Louis compared plaque buildup in two mice groups: one with genetic predisposition for hypertension and increased artery stiffness, and one “normal.” After feeding both groups a high-fat diet for 16 weeks, Wagenseil predicted a stark difference in plaque buildup between the two groups. What she found, though, strayed completely from her initial hypothesis and is now changing the way scientists understand the process of atherosclerosis.
Wagenseil anticipated the genetically vulnerable mice to have more plaque buildup than the genetically unaltered mice, but the levels were essentially the same. If hypertension and increased artery stiffness are not directly causing plaque buildup, what third factor is involved?
Previous studies in both animals and humans showed a connection between hypertension, increased arterial stiffness, and fragmentation of the arterial wall elastic fibers. When their results surprisingly showed no difference between the two mice groups’ plaque buildup, the researchers looked for evidence of elastic fiber fragmentation.
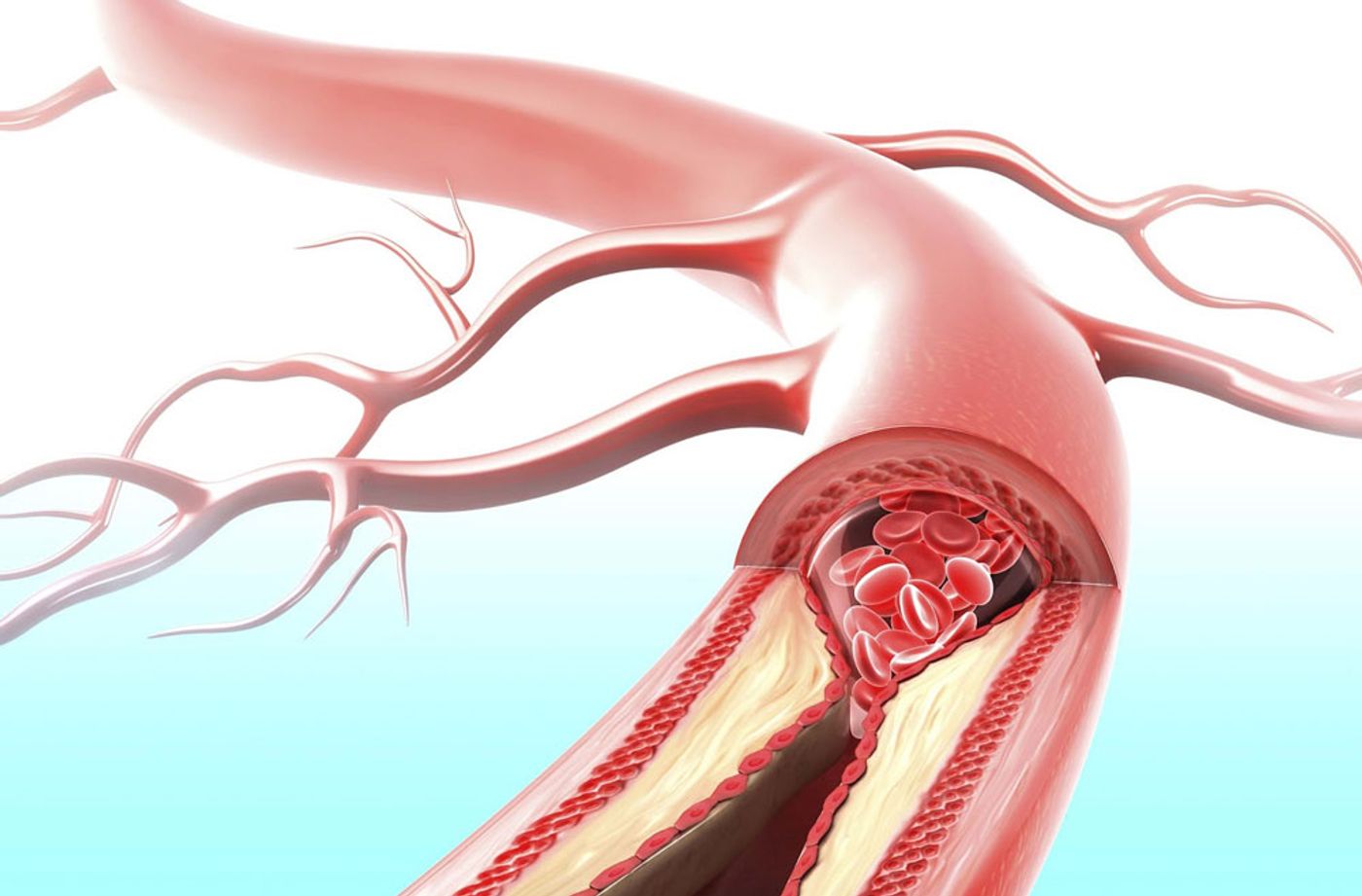
Providing multiple structural functions, elastin and collagen combine in the extracellular matrix in the vessel walls. Elastin is organized as a “fenestrated network” of elastic fibers in the medial layer of arteries, and these networks participate in the cardiac cycle as the artery extends to make room during cyclic loading. Elastic fiber networks are prone to degradation and fragmentation as the body ages or becomes diseased.
"Our surprising results suggest that treating patients for hypertension and arterial stiffness may have no effect on plaque buildup because we are not treating the underlying defect of elastic fiber fragmentation," said Wagenseil. Plaque is made up of fat, cholesterol, calcium, and other substances found in the blood, and it hardens and narrows the arteries.
Wagenseil and her team measured serum cholesterol, cytokine levels, blood pressure, aortic compliance (artery stiffness) and plaque accumulation throughout their study. While they did find evidence of reduced amounts of elastic fibers leading to hypertension and increased arterial stiffness, the fibers were not actually fragmented.
"We found that hypertension and arterial stiffness alone, without elastic fiber fragmentation, have no effect on plaque buildup,” Wagenseil said.
As an unforeseen direct cause of plaque buildup, understanding the development of fragmented elastic fibers could improve doctors’ ability to detect atherosclerosis, the process that leads to coronary artery disease. Heart disease remains the leading cause of death in the United States, leading to more than 600,000 deaths annually. Additionally, a better understanding of the risk factors for plaque buildup will improve prevention efforts, diagnoses, and treatment options.
"The next step is to determine how fragmentation affects the movement and activation of molecules and cells that are involved in plaque formation,” Wagenseil said.
Wagenseil’s study was recently published in the journal
Atherosclerosis.
Sources:
Washington University in St. Louis,
Journal of Cardiovascular Translational Research,
Centers for Disease Control and Prevention,
National Heart, Lung, and Blood Institute